Trends in the national distribution of laparoscopic hysterectomies from 2003 to 2010
- PMID: 24462854
- PMCID: PMC4318237
- DOI: 10.1016/j.jmig.2014.01.012
Trends in the national distribution of laparoscopic hysterectomies from 2003 to 2010
Abstract
Study objective: The purpose of this analysis was to compare the trends in undergoing laparoscopic hysterectomy (versus abdominal or vaginal hysterectomy) based on patient age, race, median income and insurance type, from 2003 to 2010.
Design: Retrospective study (Canadian Task Force classification II-3).
Setting: National sample of hospital admissions after hysterectomy.
Patients: Health Cost and Utilization Project-Nationwide Inpatient Sample database was used to review records of women who underwent hysterectomy for either menorrhagia or leiomyoma from 2003-2010.
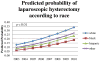
Intervention: The predicted probability of undergoing laparoscopic hysterectomy was determined for each year according to patient age, race, median income, and insurance type. The slopes of these values (i.e. the trend) was compared for each subgroup (i.e. black, white, Asian, etc.) in these categories.
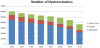
Main results: A total of 530, 154 cases were included in this study. Total number of hysterectomies decreased by 39% from 60,364 to 36,835 from 2003 to 2010. The percent of hysterectomies that were laparoscopic increased from 11% in 2003 to 29% in 2010. All groups analyzed experienced an increase in predicted probability of undergoing a laparoscopic hysterectomy. Of all women undergoing hysterectomy, the probability of undergoing a laparoscopic hysterectomy remained highest for women who were less than 35 years old, white, with the highest median income, and with private insurance from 2003-2010. The slope was significantly greater for (1) white females versus all other races analyzed (p<0.01), (2) females in the highest income quartile versus females in the lowest income quartile (p<0.01) and (3) females with private insurance versus females with Medicaid (p<0.01) or Medicare (p<0.01).
Conclusions: There remains a gap in distribution of laparoscopic hysterectomies with regards to age, race, median income and insurance type that does not seem to be closing, despite the increased availability of laparoscopic hysterectomies.
Keywords: Disparity; Laparoscopic hysterectomies.
Copyright © 2014 AAGL. Published by Elsevier Inc. All rights reserved.
Figures
Similar articles
-
Socioeconomic and racial predictors of undergoing laparoscopic hysterectomy for selected benign diseases: analysis of 341487 hysterectomies.J Minim Invasive Gynecol. 2008 Jan-Feb;15(1):11-5. doi: 10.1016/j.jmig.2007.07.014. J Minim Invasive Gynecol. 2008. PMID: 18262137
-
Disparities in use of laparoscopic hysterectomies: a nationwide analysis.J Minim Invasive Gynecol. 2014 Mar-Apr;21(2):223-7. doi: 10.1016/j.jmig.2013.08.709. Epub 2013 Sep 4. J Minim Invasive Gynecol. 2014. PMID: 24012920 Free PMC article.
-
Social determinants of access to minimally invasive hysterectomy: reevaluating the relationship between race and route of hysterectomy for benign disease.Am J Obstet Gynecol. 2017 Nov;217(5):572.e1-572.e10. doi: 10.1016/j.ajog.2017.07.036. Epub 2017 Aug 4. Am J Obstet Gynecol. 2017. PMID: 28784416
-
Health Care Disparities in Patients Undergoing Hysterectomy for Benign Indications: A Systematic Review.Obstet Gynecol. 2023 Nov 1;142(5):1044-1054. doi: 10.1097/AOG.0000000000005389. Obstet Gynecol. 2023. PMID: 37826848
-
Trends in Hysterectomies and Oophorectomies in Hospital Inpatient and Ambulatory Settings, 2005–2013.2016 Nov. In: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006 Feb–. Statistical Brief #214. 2016 Nov. In: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006 Feb–. Statistical Brief #214. PMID: 28080006 Free Books & Documents. Review. No abstract available.
Cited by
-
Association of demographic, clinical, and hospital-related factors with use of robotic hysterectomy for benign indications: A national database study.Int J Med Robot. 2020 Aug;16(4):e2107. doi: 10.1002/rcs.2107. Epub 2020 Apr 16. Int J Med Robot. 2020. PMID: 32276286 Free PMC article.
-
Predictors of the cost of hysterectomy for benign indications.J Gynecol Obstet Hum Reprod. 2021 Feb;50(2):101936. doi: 10.1016/j.jogoh.2020.101936. Epub 2020 Oct 9. J Gynecol Obstet Hum Reprod. 2021. PMID: 33039600 Free PMC article.
-
Cost drivers for benign hysterectomy within a health care system: Influence of patient, perioperative, and hospital factors.Int J Gynaecol Obstet. 2023 May;161(2):616-623. doi: 10.1002/ijgo.14593. Epub 2022 Dec 14. Int J Gynaecol Obstet. 2023. PMID: 36436911 Free PMC article.
-
Disparities in Treatment Decisions for Abnormal Uterine Bleeding.J Womens Health (Larchmt). 2021 Oct;30(10):1519-1525. doi: 10.1089/jwh.2020.8800. Epub 2021 Feb 12. J Womens Health (Larchmt). 2021. PMID: 33577392 Free PMC article.
-
Racial Disparities in Minimally Invasive Benign Hysterectomy.JSLS. 2024 Jul-Sep;28(3):e2024.00018. doi: 10.4293/JSLS.2024.00018. Epub 2025 Jan 2. JSLS. 2024. PMID: 39749229 Free PMC article.
References
-
- Abenhaim HA, Azziz R, Hu J, Bartolucci A, Tulandi T. Socioeconomic and racial predictors of undergoing laparoscopic hysterectomy for selected benign diseases: analysis of 341487 hysterectomies. Journal of minimally invasive gynecology. 2008 Jan-Feb;15(1):11–15. - PubMed
-
- Learman LA, Summitt RL, Jr, Varner RE, et al. A randomized comparison of total or supracervical hysterectomy: surgical complications and clinical outcomes. Obstet Gynecol. 2003 Sep;102(3):453–462. - PubMed
-
- Garry R. The benefits and problems associated with minimal access surgery. Aust N Z J Obstet Gynaecol. 2002 Aug;42(3):239–244. - PubMed
-
- Farquhar CM, Steiner CA. Hysterectomy rates in the United States 1990–1997. Obstet Gynecol. 2002 Feb;99(2):229–234. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous