Anti-angiogenic therapy for cancer: current progress, unresolved questions and future directions
- PMID: 24482243
- PMCID: PMC4061466
- DOI: 10.1007/s10456-014-9420-y
Anti-angiogenic therapy for cancer: current progress, unresolved questions and future directions
Erratum in
- Angiogenesis. 2014 Jul;17(3):495-7
Abstract
Tumours require a vascular supply to grow and can achieve this via the expression of pro-angiogenic growth factors, including members of the vascular endothelial growth factor (VEGF) family of ligands. Since one or more of the VEGF ligand family is overexpressed in most solid cancers, there was great optimism that inhibition of the VEGF pathway would represent an effective anti-angiogenic therapy for most tumour types. Encouragingly, VEGF pathway targeted drugs such as bevacizumab, sunitinib and aflibercept have shown activity in certain settings. However, inhibition of VEGF signalling is not effective in all cancers, prompting the need to further understand how the vasculature can be effectively targeted in tumours. Here we present a succinct review of the progress with VEGF-targeted therapy and the unresolved questions that exist in the field: including its use in different disease stages (metastatic, adjuvant, neoadjuvant), interactions with chemotherapy, duration and scheduling of therapy, potential predictive biomarkers and proposed mechanisms of resistance, including paradoxical effects such as enhanced tumour aggressiveness. In terms of future directions, we discuss the need to delineate further the complexities of tumour vascularisation if we are to develop more effective and personalised anti-angiogenic therapies.
Figures

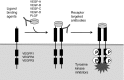


References
-
- Folkman J. Tumor angiogenesis: therapeutic implications. N Engl J Med. 1971;285(21):1182–1186. - PubMed
-
- Leite de Oliveira R, Hamm A, Mazzone M. Growing tumor vessels: more than one way to skin a cat—implications for angiogenesis targeted cancer therapies. Mol Aspects Med. 2011;32(2):71–87. - PubMed
-
- Ellis LM, Hicklin DJ. VEGF-targeted therapy: mechanisms of anti-tumour activity. Nat Rev Cancer. 2008;8(8):579–591. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

