Late antibody-mediated rejection after ABO-incompatible kidney transplantation during Gram-negative sepsis
- PMID: 24517251
- PMCID: PMC3925416
- DOI: 10.1186/1471-2369-15-31
Late antibody-mediated rejection after ABO-incompatible kidney transplantation during Gram-negative sepsis
Abstract
Background: The major challenge in ABO-incompatible transplantation is to minimize antibody-mediated rejection. Effective reduction of the anti-ABO blood group antibodies at the time of transplantation has made ABO-incompatible kidney transplantation a growing practice in our hospital and in centers worldwide. ABO antibodies result from contact with A- and B-like antigens in the intestines via nutrients and bacteria. We demonstrate a patient with fulminant antibody-mediated rejection late after ABO-incompatible kidney transplantation, whose anti-A antibody titers rose dramatically following Serratia marcescens sepsis.
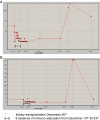
Case presentation: A 58-year-old woman underwent an ABO-incompatible kidney transplantation for end-stage renal disease secondary to autosomal dominant polycystic kidney disease. It concerned a blood group A1 to O donation. Pre-desensitization titers were 64 for anti-blood group A IgM and 32 for anti-blood group A IgG titers. Desensitization treatment consisted of rituximab, tacrolimus, mycophenolate mofetil, corticosteroids, immunoadsorption and intravenous immunoglobulins. She was readmitted to our hospital 11 weeks after transplantation for S. marcescens urosepsis. Her anti-A IgM titer rose to >5000 and she developed a fulminant antibody-mediated rejection.We hypothesized that the (overwhelming) presence in the blood of S. marcescens stimulated anti-A antibody formation, as S. marcescens might share epitopes with blood group A antigen. Unfortunately we could not demonstrate interaction between blood group A and S. marcescens in incubation experiments.
Conclusion: Two features of this post-transplant course are remarkably different from other reports of acute rejection in ABO-incompatible kidney transplantation: first, the late occurrence 12 weeks after kidney transplantation and second, the very high anti-A IgM titers (>5000), suggesting recent boosting of anti-A antibody formation by S. marcescens.
Figures

Similar articles
-
Evaluation of blood group antibodies in ABO-incompatible living-donor kidney transplantation.Int J Urol. 2015 Oct;22(10):931-6. doi: 10.1111/iju.12845. Epub 2015 Jun 23. Int J Urol. 2015. PMID: 26108258
-
Long-term desensitization for ABO-incompatible living related kidney transplantation recipients with high refractory and rebound anti-blood type antibody: case report.BMC Nephrol. 2018 Oct 5;19(1):254. doi: 10.1186/s12882-018-1053-8. BMC Nephrol. 2018. PMID: 30290778 Free PMC article.
-
Association between response to rituximab and antibody-mediated rejection in ABO-incompatible living kidney transplantation.Int J Urol. 2019 Dec;26(12):1114-1120. doi: 10.1111/iju.14108. Epub 2019 Sep 14. Int J Urol. 2019. PMID: 31522467
-
Isoagglutinin adsorption in ABO-incompatible transplantation.Transfus Apher Sci. 2010 Oct;43(2):231-5. doi: 10.1016/j.transci.2010.07.016. Epub 2010 Jul 27. Transfus Apher Sci. 2010. PMID: 20667787 Review.
-
Xenotransplantation and ABO incompatible transplantation: the similarities they share.Transfus Apher Sci. 2006 Aug;35(1):45-58. doi: 10.1016/j.transci.2006.05.007. Epub 2006 Aug 14. Transfus Apher Sci. 2006. PMID: 16905361 Review.
Cited by
-
Laboratory support of ABO antibody monitoring for ABO-incompatible solid organ transplantation.Korean J Transplant. 2022 Jun 30;36(2):99-103. doi: 10.4285/kjt.22.0011. Epub 2022 May 24. Korean J Transplant. 2022. PMID: 35919194 Free PMC article. Review.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

