Non-invasive measurement of brain temperature with microwave radiometry: demonstration in a head phantom and clinical case
- PMID: 24571829
- PMCID: PMC4066964
- DOI: 10.15274/NRJ-2014-10001
Non-invasive measurement of brain temperature with microwave radiometry: demonstration in a head phantom and clinical case
Abstract
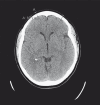
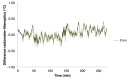
This study characterizes the sensitivity and accuracy of a non-invasive microwave radiometric thermometer intended for monitoring body core temperature directly in brain to assist rapid recovery from hypothermia such as occurs during surgical procedures. To study this approach, a human head model was constructed with separate brain and scalp regions consisting of tissue equivalent liquids circulating at independent temperatures on either side of intact skull. This test setup provided differential surface/deep tissue temperatures for quantifying sensitivity to change in brain temperature independent of scalp and surrounding environment. A single band radiometer was calibrated and tested in a multilayer model of the human head with differential scalp and brain temperature. Following calibration of a 500MHz bandwidth microwave radiometer in the head model, feasibility of clinical monitoring was assessed in a pediatric patient during a 2-hour surgery. The results of phantom testing showed that calculated radiometric equivalent brain temperature agreed within 0.4°C of measured temperature when the brain phantom was lowered 10°C and returned to original temperature (37°C), while scalp was maintained constant over a 4.6-hour experiment. The intended clinical use of this system was demonstrated by monitoring brain temperature during surgery of a pediatric patient. Over the 2-hour surgery, the radiometrically measured brain temperature tracked within 1-2°C of rectal and nasopharynx temperatures, except during rapid cooldown and heatup periods when brain temperature deviated 2-4°C from slower responding core temperature surrogates. In summary, the radiometer demonstrated long term stability, accuracy and sensitivity sufficient for clinical monitoring of deep brain temperature during surgery.
Keywords: brain temperature; core temperature; microwave radiometry; non-invasive thermometry.
Figures





References
-
- Frank SM, Fleisher LA, Breslow MJ, et al. Perioperative maintenance of normothermia reduces the incidence of morbid cardiac events. A randomized clinical trial. JAMA. 1997;277(14):1127–1134. doi: 10.1001/jama.1997.0354038004102. - DOI - PubMed
-
- Kurz A, Sessler DI, Lenhardt R. Perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization. N Engl J Med. 1996;334(19):1209–1215. doi: 10.1056/NEJM199605093341901. - DOI - PubMed
-
- Polderman KH. Mechanisms of action, physiological effects, and complications of hypothermia. Crit Care Med. 2009;37(7 Suppl):S186–S202. doi: 10.1097/CCM.0b013e3181aa5241. - DOI - PubMed
-
- Schmied H, Kurz A, Sessler DI, et al. Mild hypothermia increases blood loss and transfusion requirements during total hip arthroplasty. Lancet. 1996;347(8997):289–292. doi: 10.1016/S0140-6736(96)90466-3. - DOI - PubMed
-
- Winkler M, Akça O, Birkenberg B, et al. Aggressive warming reduces blood loss during hip arthroplasty. Anesth Analg. 2000;91(4):978–984. doi: 10.1097/00000539-200010000-00039. - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

