Incidence trends and predictors for cost and average lengths of stay in colorectal cancer surgery
- PMID: 24574722
- PMCID: PMC3923028
- DOI: 10.3748/wjg.v20.i2.532
Incidence trends and predictors for cost and average lengths of stay in colorectal cancer surgery
Abstract
Aim: To evaluate the changing trends and outcomes of colorectal cancer (CRC) surgery performed at a large single institution in Taiwan.
Methods: This study retrospectively analyzed 778 patients who received colorectal cancer surgery at E-Da Hospital in Taiwan from 2004 to 2009. These patients were from health examination, inpatient or emergency settings. The following attributes were analyzed in patients who had undergone CRC surgical procedures: gender, age, source, surgical type, tumor number, tumor size, number of lymph node metastasis, pathologic differentiation, chemotherapy, distant metastases, tumor site, tumor stage, average hospitalization cost and average lengths of stay (ALOS). The odds ratio and 95% confidence intervals were calculated to assess the relative rate of change. Regression models were employed to predict average hospitalization cost and ALOS.
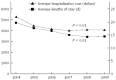
Results: The study sample included 458 (58.87%) males and 320 (41.13%) females with a mean age of 64.53 years (standard deviation, 12.33 years; range, 28-86 years). The principal patient source came from inpatient and emergency room (96.02%). The principal tumor sites were noted at the sigmoid colon (35.73%) and rectum (30.46%). Most patients exhibited a tumor stage of 2 (37.28%) or 3 (34.19%). The number of new CRC surgeries performed per 100000 persons was 12.21 in 2004 and gradually increased to 17.89 in 2009, representing a change of 46.52%. During the same period, the average hospitalization cost and ALOS decreased from $5303 to $4062 and from 19.7 to 14.4 d, respectively. The following factors were associated with considerably decreased hospital resource utilization: age, source, surgical type, tumor size, tumor site, and tumor stage.
Conclusion: These results can be generalized to patient populations elsewhere in Taiwan and to other countries with similar patient profiles.
Keywords: Average hospitalization cost; Average lengths of stay; Colorectal cancer; Colorectal cancer surgery; Incidence trend.
Figures
Similar articles
-
A cost-utility analysis of laparoscopic vs open treatment of colorectal cancer in a public hospital of the Greek National Health System.J BUON. 2013 Jan-Mar;18(1):86-97. J BUON. 2013. PMID: 23613393
-
Cost savings for elective laparoscopic resection compared with open resection for colorectal cancer in a region of high uptake.Surg Endosc. 2014 May;28(5):1515-21. doi: 10.1007/s00464-013-3345-1. Epub 2013 Dec 14. Surg Endosc. 2014. PMID: 24337191
-
Optimizing clinical and economic outcomes of surgical therapy for patients with colorectal cancer and synchronous liver metastases.J Am Coll Surg. 2012 Aug;215(2):262-70. doi: 10.1016/j.jamcollsurg.2012.03.021. Epub 2012 May 4. J Am Coll Surg. 2012. PMID: 22560316 Free PMC article.
-
Laparoscopic-assisted colorectal surgery: review of results in 752 patients.Gastroenterologist. 1995 Mar;3(1):75-89. Gastroenterologist. 1995. PMID: 7743123 Review.
-
New and Recurrent Colorectal Cancers After Resection: a Systematic Review and Meta-analysis of Endoscopic Surveillance Studies.Gastroenterology. 2019 Apr;156(5):1309-1323.e3. doi: 10.1053/j.gastro.2018.12.006. Epub 2018 Dec 13. Gastroenterology. 2019. PMID: 30553914
Cited by
-
Enhanced recovery after surgery in colon and rectal surgery: identification of predictive variables of failure in a monocentric series including 733 patients.Updates Surg. 2021 Feb;73(1):111-121. doi: 10.1007/s13304-020-00848-w. Epub 2020 Jul 8. Updates Surg. 2021. PMID: 32638264
-
Treatment Outcomes of Patients With Colorectal Cancer Enrolled in a Comprehensive Benefits Program of the National Insurance System in the Philippines: Data From the Pilot Site.JCO Glob Oncol. 2020 Feb;6:35-46. doi: 10.1200/JGO.19.00332. JCO Glob Oncol. 2020. PMID: 32031435 Free PMC article.
-
Is ERAS in laparoscopic surgery for colorectal cancer changing risk factors for delayed recovery?Med Oncol. 2016 Mar;33(3):25. doi: 10.1007/s12032-016-0738-8. Epub 2016 Feb 12. Med Oncol. 2016. PMID: 26873739 Free PMC article.
-
Musashi-1 promotes a cancer stem cell lineage and chemoresistance in colorectal cancer cells.Sci Rep. 2017 May 19;7(1):2172. doi: 10.1038/s41598-017-02057-9. Sci Rep. 2017. PMID: 28526879 Free PMC article.
-
Hospitalizations and length of stay of cancer patients: A cohort study in the Brazilian Public Health System.PLoS One. 2020 May 20;15(5):e0233293. doi: 10.1371/journal.pone.0233293. eCollection 2020. PLoS One. 2020. PMID: 32433706 Free PMC article.
References
-
- Zhang S, Cui Y, Weng Z, Gong X, Chen M, Zhong B. Changes on the disease pattern of primary colorectal cancers in Southern China: a retrospective study of 20 years. Int J Colorectal Dis. 2009;24:943–949. - PubMed
-
- Jemal A, Siegel R, Ward E, Hao Y, Xu J, Murray T, Thun MJ. Cancer statistics, 2008. CA Cancer J Clin. 2008;58:71–96. - PubMed
-
- Ferlay J, Autier P, Boniol M, Heanue M, Colombet M, Boyle P. Estimates of the cancer incidence and mortality in Europe in 2006. Ann Oncol. 2007;18:581–592. - PubMed
-
- van den Hout WB, van den Brink M, Stiggelbout AM, van de Velde CJ, Kievit J. Cost-effectiveness analysis of colorectal cancer treatments. Eur J Cancer. 2002;38:953–963. - PubMed
-
- Delcò F, Egger R, Bauerfeind P, Beglinger C. Hospital health care resource utilization and costs of colorectal cancer during the first 3-year period following diagnosis in Switzerland. Aliment Pharmacol Ther. 2005;21:615–622. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical