Magnetic resonance imaging in breath-hold divers with cerebral decompression sickness
- PMID: 24575029
- PMCID: PMC3934779
- DOI: 10.1159/000357169
Magnetic resonance imaging in breath-hold divers with cerebral decompression sickness
Abstract
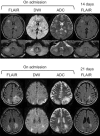
The mechanism of cerebral decompression sickness (DCS) is still unclear. We report 2 cases of breath-hold divers with cerebral DCS in whom magnetic resonance imaging (MRI) demonstrated distinctive characteristics. One case presented right hemiparesthesia, diplopia, and gait disturbance after breath-hold diving into the sea at a depth of 20 m. Brain MRI with fluid-attenuated inversion recovery (FLAIR) sequence revealed multiple hyperintense lesions in the right frontal lobe, bilateral thalamus, pons, and right cerebellar hemisphere. The second case presented visual and gait disturbance after repetitive breath-hold diving into the sea. FLAIR imaging showed hyperintense areas in the bilateral occipito-parietal lobes. In both cases, diffusion-weighted imaging and apparent diffusion coefficient mapping revealed hyperintense areas in the lesions identified by FLAIR. Moreover, follow-up MRI showed attenuation of the FLAIR signal abnormalities. These findings are suggestive of transient hyperpermeability in the microvasculature as a possible cause of cerebral DCS.
Keywords: Blood-brain barrier; Decompression illness; Magnetic resonance imaging; Vasogenic edema.
Figures
Similar articles
-
Breath-Hold Diving-Related Decompression Sickness with Brain Involvement: From Neuroimaging to Pathophysiology.Tomography. 2022 Apr 19;8(3):1172-1183. doi: 10.3390/tomography8030096. Tomography. 2022. PMID: 35645382 Free PMC article. Review.
-
Brain damage in commercial breath-hold divers.PLoS One. 2014 Aug 12;9(8):e105006. doi: 10.1371/journal.pone.0105006. eCollection 2014. PLoS One. 2014. PMID: 25115903 Free PMC article.
-
[Neurological decompression illness in a Japanese breath-held diver: a case report].Rinsho Shinkeigaku. 2012;52(10):757-61. doi: 10.5692/clinicalneurol.52.757. Rinsho Shinkeigaku. 2012. PMID: 23064626 Review. Japanese.
-
Evaluation of possible prognostic factors of fulminant acute disseminated encephalomyelitis (ADEM) on magnetic resonance imaging with fluid-attenuated inversion recovery (FLAIR) and diffusion-weighted imaging.Acta Radiol. 2009 Apr;50(3):334-9. doi: 10.1080/02841850902736617. Acta Radiol. 2009. PMID: 19235577
-
Decompression sickness in breath-hold diving, and its probable connection to the growth and dissolution of small arterial gas emboli.Math Biosci. 2015 Apr;262:1-9. doi: 10.1016/j.mbs.2015.01.001. Epub 2015 Jan 15. Math Biosci. 2015. PMID: 25598211
Cited by
-
Breath Tools: A Synthesis of Evidence-Based Breathing Strategies to Enhance Human Running.Front Physiol. 2022 Mar 17;13:813243. doi: 10.3389/fphys.2022.813243. eCollection 2022. Front Physiol. 2022. PMID: 35370762 Free PMC article. Review.
-
Breath-Hold Diving-Related Decompression Sickness with Brain Involvement: From Neuroimaging to Pathophysiology.Tomography. 2022 Apr 19;8(3):1172-1183. doi: 10.3390/tomography8030096. Tomography. 2022. PMID: 35645382 Free PMC article. Review.
-
Investigation of Brain Impairment Using Diffusion-Weighted and Diffusion Tensor Magnetic Resonance Imaging in Experienced Healthy Divers.Med Sci Monit. 2018 Nov 17;24:8279-8289. doi: 10.12659/MSM.911475. Med Sci Monit. 2018. PMID: 30447152 Free PMC article.
-
The risk of decompression illness in breath-hold divers: a systematic review.Diving Hyperb Med. 2023 Mar 31;53(1):31-41. doi: 10.28920/dhm53.1.31-41. Diving Hyperb Med. 2023. PMID: 36966520 Free PMC article.
-
Physiology, pathophysiology and (mal)adaptations to chronic apnoeic training: a state-of-the-art review.Eur J Appl Physiol. 2021 Jun;121(6):1543-1566. doi: 10.1007/s00421-021-04664-x. Epub 2021 Mar 31. Eur J Appl Physiol. 2021. PMID: 33791844 Free PMC article. Review.
References
-
- Vann RD, Butler FK, Mitchell SJ, Moon RE. Decompression illness. Lancet. 2011;377:153–164. - PubMed
-
- Bove AA. Risk of decompression sickness with patent foramen ovale. Undersea Hyperb Med. 1998;25:175–178. - PubMed
-
- Kohshi K, Wong RM, Abe H, Katoh T, Okudera T, Mano Y. Neurological manifestations in Japanese ama divers. Undersea Hyperb Med. 2005;32:11–20. - PubMed
-
- Schwerzmann M, Seiler C, Lipp E, Guzman R, Lovblad KO, Kraus M, Kucher N. Relation between directly detected patent foramen ovale and ischemic brain lesions in sport divers. Ann Intern Med. 2001;134:21–24. - PubMed
-
- Warren LP, Jr, Djang WT, Moon RE, Camporesi EM, Sallee DS, Anthony DC, Massey EW, Burger PC, Heinz ER. Neuroimaging of scuba diving injuries to the CNS. AJR Am J Roentgenol. 1988;151:1003–1008. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources