Objective factors associated with physicians' and nurses' perceptions of intensive care unit capacity strain
- PMID: 24575984
- PMCID: PMC3972969
- DOI: 10.1513/AnnalsATS.201306-141OC
Objective factors associated with physicians' and nurses' perceptions of intensive care unit capacity strain
Abstract
Rationale: Time-varying demand for critical care may strain the capacities of intensive care units (ICUs) to provide optimal care. Intensivists and ICU nurses may be the best judges of the strain on their ICU. Yet, it is not clear what ICU and hospital factors contribute to this perceived sense of strain among ICU providers.
Objectives: To identify measureable ICU and hospital factors associated with perceived strain by intensivists and ICU nurses.
Methods: During a 6-month prospective cohort study, we surveyed nurses and physicians responsible for bed management regarding the ability of a 24-bed medical ICU (MICU) to provide optimal critical care. We simultaneously assessed time-varying ICU-level factors, including patient census, number of admissions, average patient acuity, number of interhospital transfer requests, and censuses of other hospital units. To identify factors associated with strain, we used an algorithm for covariate selection in regression models that selects variables that contribute sufficiently to model prediction to justify their inclusion.
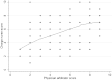
Measurements and main results: Of 254 surveys, 226 (89%) were completed by 18 charge nurses and 17 physicians. On a scale of 1 to 10 (where a higher score indicated more strain), the median perceived strain score among nurses was 6 (interquartile range, 3-7) and among physicians was 5 (interquartile range, 3-7), with moderate correlation within days (interclass correlation coefficient, 0.45; 95% confidence interval: 0.30, 0.60). Average patient acuity, MICU census, number of MICU admissions, and general ward census were included in the most efficient model of strain perceived by nurses. Only MICU census was strongly associated with strain perceived by physicians.
Conclusions: A model containing commonly available metrics of ICU census, average patient acuity, and the proportion of new admissions has validity as a model of ICU nurses' perceived ICU capacity strain. However, only ICU census was associated with increased perceived capacity strain by physicians, highlighting the need for involvement of multiple stakeholder groups to improve our understanding of ICU capacity strain.
Figures
Comment in
-
What we talk about when we talk about intensive care unit strain.Ann Am Thorac Soc. 2014 Feb;11(2):219-20. doi: 10.1513/AnnalsATS.201311-406ED. Ann Am Thorac Soc. 2014. PMID: 24575987 No abstract available.
References
-
- Hanson CW, III, Deutschman CS, Anderson HL, III, Reilly PM, Behinger EC, Schwab CW, Price J. Effects of an organized critical care service on outcomes and resource utilization: a cohort study. Crit Care Med. 1999;27:270–274. - PubMed
-
- Pronovost PJ, Angus DC, Dorman T, Robinson KA, Dremsizov TT, Young TL. Physician staffing patterns and clinical outcomes in critically ill patients: a systematic review. JAMA. 2002;288:2151–2162. - PubMed
-
- Ely EW, Baker AM, Dunagan DP, Burke HL, Smith AC, Kelly PT, Johnson MM, Browder RW, Bowton DL, Haponik EF. Effect on the duration of mechanical ventilation of identifying patients capable of breathing spontaneously. N Engl J Med. 1996;335:1864–1869. - PubMed
-
- Kahn JM, Goss CH, Heagerty PJ, Kramer AA, O’Brien CR, Rubenfeld GD. Hospital volume and the outcomes of mechanical ventilation. N Engl J Med. 2006;355:41–50. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical