Inducible protein-10, a potential driver of neurally controlled interleukin-10 and morbidity in human blunt trauma
- PMID: 24584064
- PMCID: PMC4133186
- DOI: 10.1097/CCM.0000000000000248
Inducible protein-10, a potential driver of neurally controlled interleukin-10 and morbidity in human blunt trauma
Abstract
Objective: Blunt trauma and traumatic spinal cord injury induce systemic inflammation that contributes to morbidity. Dysregulated neural control of systemic inflammation postinjury is likely exaggerated in patients with traumatic spinal cord injury. We used in silico methods to discern dynamic inflammatory networks that could distinguish systemic inflammation in traumatic spinal cord injury from blunt trauma.
Design: Retrospective study.
Settings: Tertiary care institution.
Patients: Twenty-one severely injured thoracocervical traumatic spinal cord injury patients and matched 21 severely injured blunt trauma patients without spinal cord injury.
Intervention: None.
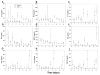
Measurements and main results: Serial blood samples were obtained from days 1 to 14 postinjury. Twenty-four plasma inflammatory mediators were quantified. Statistical significance between the two groups was determined by two-way analysis of variance. Dynamic Bayesian network inference was used to suggest dynamic connectivity and central inflammatory mediators. Circulating interleukin-10 was significantly elevated in thoracocervical traumatic spinal cord injury group versus non-spinal cord injury group, whereas interleukin-1β, soluble interleukin-2 receptor-α, interleukin-4, interleukin-5, interleukin-7, interleukin-13, interleukin-17, macrophage inflammatory protein 1α and 1β, granulocyte-macrophage colony-stimulating factor, and interferon-γ were significantly reduced in traumatic spinal cord injury group versus non-spinal cord injury group. Dynamic Bayesian network suggested that post-spinal cord injury interleukin-10 is driven by inducible protein-10, whereas monocyte chemotactic protein-1 was central in non-spinal cord injury dynamic networks. In a separate validation cohorts of 356 patients without spinal cord injury and 85 traumatic spinal cord injury patients, individuals with plasma inducible protein-10 levels more than or equal to 730 pg/mL had significantly prolonged hospital and ICU stay and days on mechanical ventilator versus patients with plasma inducible protein-10 level less than 730 pg/mL.
Conclusion: This is the first study to compare the dynamic systemic inflammatory responses of traumatic spinal cord injury patients versus patients without spinal cord injury, suggesting a key role for inducible protein-10 in driving systemic interleukin-10 and morbidity and highlighting the potential utility of in silico tools to identify key inflammatory drivers.
Figures








Comment in
-
Data-driven, evidenced-based, computational modeling research is still needed in trauma research.Crit Care Med. 2014 Jun;42(6):1566-7. doi: 10.1097/CCM.0000000000000269. Crit Care Med. 2014. PMID: 24836802 No abstract available.
References
-
- Thuret S, Moon LD, Gage FH. Therapeutic interventions after spinal cord injury. Nat Rev Neurosci. 2006;7:628–643. - PubMed
-
- Burt BM, Afifi HY, Wantz GE, et al. Traumatic lumbar hernia: report of cases and comprehensive review of the literature. J Trauma. 2004;57:1361–1370. - PubMed
-
- Cripps RA, Lee BB, Wing P, et al. A global map for traumatic spinal cord injury epidemiology: towards a living data repository for injury prevention. Spinal Cord. 2011;49:493–501. - PubMed
-
- Gris D, Hamilton EF, Weaver LC. The systemic inflammatory response after spinal cord injury damages lungs and kidneys. Exp Neurol. 2008;211:259–270. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

