Evidence that HIV-1 CRF01_AE is associated with low CD4+T cell count and CXCR4 co-receptor usage in recently infected young men who have sex with men (MSM) in Shanghai, China
- PMID: 24586795
- PMCID: PMC3931781
- DOI: 10.1371/journal.pone.0089462
Evidence that HIV-1 CRF01_AE is associated with low CD4+T cell count and CXCR4 co-receptor usage in recently infected young men who have sex with men (MSM) in Shanghai, China
Erratum in
- PLoS One. 2014;9(5):e97395
Abstract
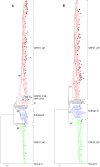
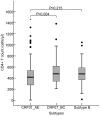
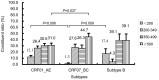
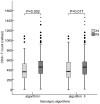
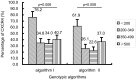
Men who have sex with men (MSM) have recently accounted for an alarmingly increasing proportion of HIV-1 transmission in China. In order to investigate the immune status as a result of CRF01_AE infection and CXCR4 co-receptor usage in a young Shanghai-based HIV-1-infected MSM population in Shanghai, 364 HIV-1-infected MSM with average age of 22.7 years old, newly diagnosed between Jan 2009 and Jul 2013 were analyzed for CD4+T cell count, subtyping using phylogenetic analysis, and viral co-receptor tropism using Geno2pheno and webPSSM in combination. A total of 276 individuals were identified as recently infected. Subtype assignment were as follows: 176 (63.8%) CRF01_AE, 77 (27.9%) CRF07_BC, and 23 (8.3%) subtype B. Besides, 24 second-generation recombinant strains were identified. A lower CD4+T cell count at baseline survey was observed among CRF01_AE strain-infected individuals, compared to those who were infected with CRF07_BC (P<0.01). The frequency of baseline CD4+T cell count <200 was higher and the frequency of CD4 T counts >500 lower in CRF01_AE infection than CRF07_BC infection. It is worth noting that 32.4%-40.9% of CRF01_AE strain-infected individuals were predicted to carry CXCR4-tropic viruses whereas none of CRF07_BC and subtype B were found to be as CXCR4-tropic viruses (P<0.001). As could be expected CXCR4 tropism was associated with lower CD4 T counts. This study revealed that CRF01_AE strains with high frequency of CXCR4 tropism are prevailing in the young MSM population in China and could potentially cause a severe loss of CD4+T cell count and rapid disease progression. A regular surveillance of HIV-1 subtypes, CD4+T cell count and viral co-receptor usage would be greatly beneficial for effectively monitoring disease progression, improvement of antiretroviral therapy strategy and prompt intervention of transmission.
Conflict of interest statement
Figures
Similar articles
-
HIV-1 Genetic Diversity and Its Impact on Baseline CD4+T Cells and Viral Loads among Recently Infected Men Who Have Sex with Men in Shanghai, China.PLoS One. 2015 Jun 29;10(6):e0129559. doi: 10.1371/journal.pone.0129559. eCollection 2015. PLoS One. 2015. PMID: 26121491 Free PMC article.
-
After 18 months of antiretroviral therapy, total HIV DNA decreases more pronouncedly in patients infected by CRF01_AE than in those infected by subtype B and CRF07_BC.Microbiol Immunol. 2018 Apr;62(4):248-254. doi: 10.1111/1348-0421.12578. Epub 2018 Mar 26. Microbiol Immunol. 2018. PMID: 29377267
-
Low CD4 count was characterized in recent HIV CRF01_AE infection and it rapidly increased to reach a peak in the first year since ART initiation.BMC Infect Dis. 2025 Mar 31;25(1):443. doi: 10.1186/s12879-025-10799-5. BMC Infect Dis. 2025. PMID: 40165131 Free PMC article.
-
Distinct genetic clusters in HIV-1 CRF01_AE-infected patients induced variable degrees of CD4+ T-cell loss.mBio. 2024 Mar 13;15(3):e0334923. doi: 10.1128/mbio.03349-23. Epub 2024 Feb 22. mBio. 2024. PMID: 38385695 Free PMC article.
-
Rapid CD4+ T-cell decline is associated with coreceptor switch among MSM primarily infected with HIV-1 CRF01_AE in Northeast China.AIDS. 2019 Jan 27;33(1):13-22. doi: 10.1097/QAD.0000000000001981. AIDS. 2019. PMID: 30102662
Cited by
-
Substitution of gp120 C4 region compensates for V3 loss-of-fitness mutations in HIV-1 CRF01_AE co-receptor switching.Emerg Microbes Infect. 2023 Dec;12(1):e2169196. doi: 10.1080/22221751.2023.2169196. Emerg Microbes Infect. 2023. PMID: 36647730 Free PMC article.
-
Critical amino acid residues and potential N-linked glycosylation sites contribute to circulating recombinant form 01_AE pathogenesis in Northeast China.AIDS. 2019 Jul 15;33(9):1431-1439. doi: 10.1097/QAD.0000000000002197. AIDS. 2019. PMID: 30889014 Free PMC article.
-
Existence of Replication-Competent Minor Variants with Different Coreceptor Usage in Plasma from HIV-1-Infected Individuals.J Virol. 2020 Jun 1;94(12):e00193-20. doi: 10.1128/JVI.00193-20. Print 2020 Jun 1. J Virol. 2020. PMID: 32295903 Free PMC article.
-
HIV-1 genotype diversity and distribution characteristics among heterosexually transmitted population in Jiangsu province, China.Virol J. 2019 Apr 25;16(1):51. doi: 10.1186/s12985-019-1162-4. Virol J. 2019. PMID: 31023323 Free PMC article.
-
Prevalence of different HIV-1 subtypes in sexual transmission in China: a systematic review and meta-analysis.Epidemiol Infect. 2016 Jul;144(10):2144-53. doi: 10.1017/S0950268816000212. Epub 2016 Feb 19. Epidemiol Infect. 2016. PMID: 26892485 Free PMC article.
References
-
- Ministry of Health of the People’s Republic of China. 2012 China AIDS Response Progress Report. 5–6.
-
- Wang L, Norris JL, Li DM, Guo W, Ding ZW, et al. (2012) HIV prevalence and influencing factors analysis of sentinel surveillance among men who have sex with men in China, 2003–2011. Chin Med J (Engl) 125: 1857–1861. - PubMed
-
- Zhang X, Li S, Li X, Xu J, Li D, et al. (2007) Characterization of HIV-1 subtypes and viral antiretroviral drug resistance in men who have sex with men in Beijing, China. AIDS 21 Suppl 8S59–65. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

