Continuity and the costs of care for chronic disease
- PMID: 24638880
- PMCID: PMC4075052
- DOI: 10.1001/jamainternmed.2014.245
Continuity and the costs of care for chronic disease
Abstract
Importance: Better continuity of care is expected to improve patient outcomes and reduce health care costs, but patterns of use, costs, and clinical complications associated with the current patterns of care continuity have not been quantified.
Objective: To measure the association between care continuity, costs, and rates of hospitalizations, emergency department visits, and complications for Medicare beneficiaries with chronic disease.
Design, setting, and participants: Retrospective cohort study of insurance claims data for a 5% sample of Medicare beneficiaries experiencing a 12-month episode of care for congestive heart failure (CHF, n = 53,488), chronic obstructive pulmonary disease (COPD, n = 76,520), or type 2 diabetes mellitus (DM, n = 166,654) in 2008 and 2009.
Main outcomes and measures: Hospitalizations, emergency department visits, complications, and costs of care associated with the Bice-Boxerman continuity of care (COC) index, a measure of the outpatient COC related to conditions of interest.
Results: The mean (SD) COC index was 0.55 (0.31) for CHF, 0.60 (0.34) for COPD, and 0.50 (0.32) for DM. After multivariable adjustment, higher levels of continuity were associated with lower odds of inpatient hospitalization (odds ratios for a 0.1-unit increase in COC were 0.94 [95% CI, 0.93-0.95] for CHF, 0.95 [0.94-0.96] for COPD, and 0.95 [0.95-0.96] for DM), lower odds of emergency department visits (0.92 [0.91-0.92] for CHF, 0.93 [0.92-0.93] for COPD, and 0.94 [0.93-0.94] for DM), and lower odds of complications (odds ratio range, 0.92-0.96 across the 3 complication types and 3 conditions; all P < .001). For every 0.1-unit increase in the COC index, episode costs of care were 4.7% lower for CHF (95% CI, 4.4%-5.0%), 6.3% lower for COPD (6.0%-6.5%), and 5.1% lower for DM (5.0%-5.2%) in adjusted analyses.
Conclusions and relevance: Modest differences in care continuity for Medicare beneficiaries are associated with sizable differences in costs, use, and complications.
Conflict of interest statement
All authors report no conflicts of interest.
Figures
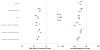
Comment in
-
Care continuity and care coordination: what counts?JAMA Intern Med. 2014 May;174(5):749-50. doi: 10.1001/jamainternmed.2013.14331. JAMA Intern Med. 2014. PMID: 24638199 No abstract available.
References
-
- Bodenheimer T. Coordinating care--a perilous journey through the health care system. N Engl J Med. 2008 Mar 6;358(10):1064–1071. - PubMed
-
- Pham HH, Schrag D, O’Malley AS, Wu B, Bach PB. Care patterns in Medicare and their implications for pay for performance. New England Journal of Medicine. 2007 Mar 15;356(11):1130–1139. - PubMed
-
- National Priorities Partnership. [Accessed February 24, 2010];National Priorities and Goals: Aligning Our Efforts to Transform America’s Healthcare. 2008 http://www.nationalprioritiespartnership.org/uploadedFiles/NPP/08-253-NQ....
-
- Institute of Medicine. Priority areas for national action: transforming health care quality. Washington, DC: National Academies Press; 2003. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

