Novel Use of Hydromorphone as a Pretreatment Agent: A Double-blind, Randomized, Controlled Study in Adult Korean Surgical Patients
- PMID: 24648574
- PMCID: PMC3955243
- DOI: 10.1016/j.curtheres.2011.02.001
Novel Use of Hydromorphone as a Pretreatment Agent: A Double-blind, Randomized, Controlled Study in Adult Korean Surgical Patients
Abstract
Background: Hydromorphone is a potent μ-opioid selective agonist that has an onset time within 5 minutes and reaches peak effect between 10 and 20 minutes. However, it may show immediate analgesic effect to rocuronium-induced pain because of its peripheral analgesic property and also may attenuate noxious stimuli from tracheal intubation during induction. The opioid receptors are known to be present in peripheral sensory nerve terminals as well as in the dorsal root ganglion and the central terminal of primary afferent nerves. Therefore, we hypothesized that hydromorphone may be considered a potent pretreatment or adjuvant drug during the induction of anesthesia with its peripherally and centrally mediated analgesia.
Objective: The aim of this study was to compare the effects of pretreatment with hydromorphone in reducing rocuronium-induced withdrawal movements and hemodynamic changes during tracheal intubation with the effects of fentanyl and normal saline.
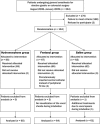
Methods: In this double-blind, randomized, controlled study, consecutive adult patients aged 20 to 70 years who were scheduled to undergo general anesthesia for elective gastric or colorectal surgery at the Samsung Seoul Hospital (Seoul, Republic of Korea) were randomly assigned to receive 5 mL hydromorphone 0.03 mg/kg or fentanyl 2 μg/kg or normal saline. Thirty seconds after administering the study drug, anesthesia was induced with 2.5% thiopental sodium 5 mg/kg. After loss of consciousness, rocuronium 0.6 mg/kg was injected and immediate withdrawal movements were recorded. Two minutes after rocuronium injection, tracheal intubation was performed and hemodynamic changes were observed.
Results: A total of 194 patients were enrolled, with 65 in the hydromorphone group, 67 in the fentanyl group, and 62 in the saline group. The overall incidence of withdrawal movements was significantly lower in the hydromorphone group (2 patients; 3.1%) and the fentanyl group (5 patients; 7.5%) (both, P < 0.001) than in the saline group (36 patients; 58.1%). The mean arterial pressure (MAP) and heart rate (HR) after intubation (median [interquartile range]) in the fentanyl group (101.5 [84-115] mm Hg; 93.5 [82-102] beats per minute [bpm]) and the hydromorphone group (93.0 [83-106] mm Hg; 90.0 [86.3-93.6] bpm) were significantly lower than these measures in the saline group (111.5 [105-123] mm Hg; 103.5 [96-113] bpm) (fentanyl group MAP and HR, P < 0.001; hydromorphone group MAP and HR, P < 0.001).
Conclusions: Pretreatment with hydromorphone and fentanyl may have similar effectiveness in reducing withdrawal movements in response to rocuronium injection pain and inducing immediate general anesthesia.
Keywords: hydromorphone; induction of anesthesia; injection pain; rocuronium; withdrawal movement.
Figures

References
-
- Oh A.Y., Seo K.S., Goo E.K. Prevention of withdrawal movement associated with injection of rocuronium in children: Comparison of remifentanil, alfentanil and fentanyl. Acta Anaesthesiol Scand. 2007;51:1190–1193. - PubMed
-
- Stein C., Schäfer M., Hassan A.H. Peripheral opioid receptors. Ann Med. 1995;27:219–221. - PubMed
-
- Blunk J.A., Seifert F., Schmelz M. Injection pain of rocuronium and vecuronium is evoked by direct activation of nociceptive nerve endings. Eur J Anaesthesiol. 2003;20:245–253. - PubMed
-
- Kindgen-Milles D., Klement W., Arndt J.O. The nociceptive systems of skin, paravascular tissue and hand veins of humans and their sensitivity to bradykinin. Neurosci Lett. 1994;181:39–42. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

