Use of evidence-based interventions in acute coronary syndrome - Subanalysis of the ACCEPT registry
- PMID: 24652052
- PMCID: PMC4028936
- DOI: 10.5935/abc.20140033
Use of evidence-based interventions in acute coronary syndrome - Subanalysis of the ACCEPT registry
Abstract
Background: The recommendations in guidelines are based on evidence; however, there is a gap between recommendations and clinical practice.
Objective: To describe the practice of prescribing evidence-based treatments for patients with acute coronary syndrome in Brazil.
Methods: This study carried out a subanalysis of the ACCEPT registry, assessing epidemiological data and the prescription rate of acetylsalicylic acid, p2y12 inhibitors, antithrombotic drugs, beta-blockers, angiotensin-converting enzyme inhibitors/angiotensin-receptor blockers (IAT1RB), and statins. In addition, the quality of myocardial reperfusion in ST-segment elevation myocardial infarction was evaluated.
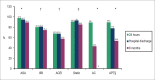
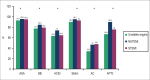
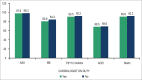
Results: This study assessed 2,453 patients. The prescription rates of acetylsalicylic acid, p2y12 inhibitors, antithrombotic drugs, beta-blockers, angiotensin-converting enzyme inhibitors/IAT1RB, and statins were as follows: in 24 hours - 97.6%, 89.5%, 89.1%, 80.2%, 67.9% and 90.6%; and at six months - 89.3%, 53.6%, 0%, 74.4%, 57.6% and 85.4%, respectively. Regarding ST-segment elevation myocardial infarction, only 35.9% and 25.3% of the patients underwent primary angioplasty and thrombolysis, respectively, within the recommended times.
Conclusion: This registry showed high initial prescription rates of antiplatelet drugs, antithrombotic drugs, and statins, and lower prescription rates of beta-blockers and angiotensin-converting enzyme inhibitors/IAT1RB. Independently of the class, the use of all drugs decreased by six months. Most patients with ST-segment elevation myocardial infarction did not undergo myocardial reperfusion within the time recommended.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures


Similar articles
-
Decade-Long Trends (2001 to 2011) in the Use of Evidence-Based Medical Therapies at the Time of Hospital Discharge for Patients Surviving Acute Myocardial Infarction.Am J Cardiol. 2016 Dec 15;118(12):1792-1797. doi: 10.1016/j.amjcard.2016.08.065. Epub 2016 Sep 13. Am J Cardiol. 2016. PMID: 27743577 Free PMC article.
-
Implementation of a Regional Network for ST-Segment-Elevation Myocardial Infarction (STEMI) Care and 30-Day Mortality in a Low- to Middle-Income City in Brazil: Findings From Salvador's STEMI Registry (RESISST).J Am Heart Assoc. 2018 Jul 6;7(14):e008624. doi: 10.1161/JAHA.118.008624. J Am Heart Assoc. 2018. PMID: 29980522 Free PMC article.
-
Long-Term Quality of Prescription for ST-Segment Elevation Myocardial Infarction (STEMI) Patients: A Real World 1-Year Follow-Up Study.Am J Cardiovasc Drugs. 2020 Feb;20(1):105-115. doi: 10.1007/s40256-019-00361-5. Am J Cardiovasc Drugs. 2020. PMID: 31300969 Free PMC article.
-
New recommendations from the 1999 American College of Cardiology/American Heart Association acute myocardial infarction guidelines.Ann Pharmacother. 2001 May;35(5):589-617. doi: 10.1345/aph.10319. Ann Pharmacother. 2001. PMID: 11346067 Review.
-
[The use of other drugs apart from antithrombotic and antiplatelet agents for the treatment of non-ST-elevation acute coronary syndromes].Anadolu Kardiyol Derg. 2006 Apr;6 Suppl 1:30-4. Anadolu Kardiyol Derg. 2006. PMID: 16613773 Review. Turkish.
Cited by
-
Reperfusion Therapy Optimization in Acute Myocardial Infarction with ST-Segment Elevation using WhatsApp®-Based Telemedicine.Arq Bras Cardiol. 2022 Mar;118(3):556-564. doi: 10.36660/abc.20201243. Arq Bras Cardiol. 2022. PMID: 35137785 Free PMC article. English, Portuguese.
-
Implementation of a Best Practice in Cardiology (BPC) Program Adapted from Get With The Guidelines®in Brazilian Public Hospitals: Study Design and Rationale.Arq Bras Cardiol. 2020 Jul;115(1):92-99. doi: 10.36660/abc.20190393. Epub 2020 Aug 7. Arq Bras Cardiol. 2020. PMID: 32187286 Free PMC article. English, Portuguese.
-
Prescription Rates for Antiplatelet Therapy (APT) in Coronary Artery Disease (CAD) - What Benchmark are We Aiming at in Continuing Medical Education (CME)?J Eur CME. 2020 Oct 23;9(1):1836866. doi: 10.1080/21614083.2020.1836866. J Eur CME. 2020. PMID: 33224627 Free PMC article.
-
Atherosclerosis and Inflammation: Still a Long Way to Go.Arq Bras Cardiol. 2020 Apr;114(4):699-700. doi: 10.36660/abc.20200219. Epub 2020 May 29. Arq Bras Cardiol. 2020. PMID: 32491005 Free PMC article. English, Portuguese. No abstract available.
-
Epidemiological Profile and Quality Indicators in Patients with Acute Coronary Syndrome in Northern Minas Gerais - Minas Telecardio 2 Project.Arq Bras Cardiol. 2016 Aug;107(2):106-15. doi: 10.5935/abc.20160095. Epub 2016 Jun 23. Arq Bras Cardiol. 2016. PMID: 27355471 Free PMC article.
References
-
- Andrade JP, Piva e Mattos LA, Carvalho AC, Machado CA, Oliveira GM. National physician qualification program in cardiovascular disease prevention and integral care. Arq Bras Cardiol. 2013;100(3):203–211. - PubMed
-
- Nicolau JC, Franken M, Lotufo PA, Carvalho AC, Marin JA, Neto, Lima FG, et al. Utilização de terapêuticas comprovadamente úteis no tratamento da coronariopatia aguda: comparação entre diferentes regiões brasileiras. Análise do registro brasileiro de síndromes coronarianas agudas (BRACE - Brazilian Registry on Acute Coronary Syndromes) . Arq Bras Cardiol. 2012;98(4):282–289. - PubMed
-
- Piegas LS, Avezum A, Guimaraes HP, Muniz AJ, Reis HJ, dos Santos ES, et al. Acute coronary syndrome behavior: results of a brazilian registry. Arq Bras Cardiol. 2013;100(6):502–510. - PubMed
-
- Berwanger O, Piva e Mattos LA, Martin JF, Lopes RD, Figueiredo EL, Magnoni D, et al. Evidence-based therapy prescription in high-cardiovascular risk patients: the react study. Arq Bras Cardiol. 2013;100(3):212–220. - PubMed
-
- Piegas LS, Feitosa G, Mattos LA, Nicolau JC, Rossi JM, Neto, Timerman A, et al. Sociedade Brasileira de Cardiologia Diretriz da Sociedade Brasileira de Cardiologia sobre tratamento do infarto agudo do miocárdio com supradesnível do segmento ST. Arq Bras Cardiol. 2009;93(6) supl.2:e179–e264. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

