Meta-analysis of methicillin-resistant Staphylococcus aureus colonization and risk of infection in dialysis patients
- PMID: 24652802
- PMCID: PMC4147983
- DOI: 10.1681/ASN.2013091028
Meta-analysis of methicillin-resistant Staphylococcus aureus colonization and risk of infection in dialysis patients
Abstract
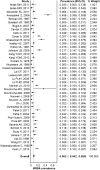
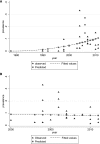
Patients undergoing dialysis are particularly vulnerable to methicillin-resistant Staphylococcus aureus (MRSA) infections. We performed a meta-analysis of published studies to estimate the prevalence of MRSA colonization in dialysis patients, time trends, and long-term risk of subsequent MRSA infections. Our search of the PubMed and Embase databases returned 5743 nonduplicate citations, from which we identified 38 relevant studies that included data on 5596 dialysis patients. The estimated prevalence of MRSA colonization was 6.2% (95% confidence interval [95% CI], 4.2% to 8.5%). The prevalence increased over time but remained stable after 2000. Stratification of patients according to dialysis modality and setting revealed that 7.2% (95% CI, 4.9% to 9.9%) of patients on hemodialysis were colonized with MRSA compared with 1.3% (95% CI, 0.5% to 2.4%) of patients on peritoneal dialysis (P=0.01), and that a statistically significant difference existed in the percentage of colonized inpatients and outpatients (14.2% [95% CI, 8.0% to 21.8%] versus 5.4% [95% CI, 3.5% to 7.7%], respectively; P=0.04). Notably, the risk of developing MRSA infections increased among colonized hemodialysis patients compared with noncolonized patients (relative risk, 11.5 [95% CI, 4.7 to 28.0]). The long-term (6-20 months) probability of developing a MRSA infection was 19% among colonized hemodialysis patients compared with only 2% among noncolonized patients. In summary, 6.2% of dialysis patients are MRSA colonized, and the average prevalence of colonization has remained stable since 2000. Colonization in hemodialysis patients is associated with increased risk of MRSA infection.
Copyright © 2014 by the American Society of Nephrology.
Figures

References
-
- Kaye KS, Anderson DJ, Choi Y, Link K, Thacker P, Sexton DJ: The deadly toll of invasive methicillin-resistant Staphylococcus aureus infection in community hospitals. Clin Infect Dis 46: 1568–1577, 2008 - PubMed
-
- Centers for Disease Control and Prevention (CDC) : Invasive methicillin-resistant Staphylococcus aureus infections among dialysis patients—United States, 2005. MMWR Morb Mortal Wkly Rep 56: 197–199, 2007 - PubMed
-
- Centers for Disease Control and Prevention (CDC): Active Bacterial Core Surveillance Report: Emerging Infections Program Network, Methicillin- Resistant Staphylococcus aureus, 2011. Available at: http://www.cdc.gov/abcs/reports findings/survreports/mrsa11.pdf Accessed September 3, 2013
-
- von Eiff C, Becker K, Machka K, Stammer H, Peters G, Study Group : Nasal carriage as a source of Staphylococcus aureus bacteremia. N Engl J Med 344: 11–16, 2001 - PubMed
-
- Saxena AK, Panhotra BR, Al-hafiz AA, Sundaram DS, Abu-Oyun B, Al Mulhim K: Cefotaxime-heparin lock prophylaxis against hemodialysis catheter-related sepsis among Staphylococcus aureus nasal carriers. Saudi J Kidney Dis Transpl 23: 743–754, 2012 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

