Neuro-intensive treatment targeting intracranial hypertension improves outcome in severe bacterial meningitis: an intervention-control study
- PMID: 24667767
- PMCID: PMC3965390
- DOI: 10.1371/journal.pone.0091976
Neuro-intensive treatment targeting intracranial hypertension improves outcome in severe bacterial meningitis: an intervention-control study
Abstract
Objective: To evaluate the efficacy of early intracranial pressure (ICP)-targeted treatment, compared to standard intensive care, in adults with community acquired acute bacterial meningitis (ABM) and severely impaired consciousness.
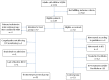
Design: A prospectively designed intervention-control comparison study of adult cases from September 2004 to January 2012.
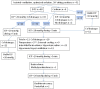
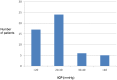
Patients: Included patients were confirmed ABM-cases, aged 16-75 years, with severely impaired mental status on admission. Fifty-two patients, given ICP-targeted treatment at the neuro-intensive care unit, and 53 control cases, treated with conventional intensive care, were included. All the patients received intensive care with mechanical ventilation, sedation, antibiotics and corticosteroids according to current guidelines. Additional ICP-treatment in the intervention group included cerebrospinal fluid drainage using external ventricular catheters (n = 48), osmotherapy (n = 21), hyperventilation (n = 13), external cooling (n = 9), gram-doses of methylprednisolone (n = 3) and deep barbiturate sedation (n = 2) aiming at ICP <20 mmHg and a cerebral perfusion pressure of >50 mmHg.
Measurements: The primary endpoint was mortality at two months and secondary endpoint was Glasgow outcome score and hearing ability at follow-up at 2-6 months.
Outcomes: The mortality was significantly lower in the intervention group compared to controls, 5/52 (10%) versus 16/53 (30%; relative risk reduction 68%; p<0.05). Furthermore, only 17 patients (32%) in the control group fully recovered compared to 28 (54%) in the intervention group (relative risk reduction 40%; p<0.05).
Conclusions: Early neuro-intensive care using ICP-targeted therapy, mainly cerebrospinal fluid drainage, reduces mortality and improves the overall outcome in adult patients with ABM and severely impaired mental status on admission.
Conflict of interest statement
Figures
References
-
- de Gans J, van de Beek D, European Dexamethasone in Adulthood Bacterial Meningitis Study I (2002) Dexamethasone in adults with bacterial meningitis. The New England journal of medicine 347: 1549–1556. - PubMed
-
- Durand ML, Calderwood SB, Weber DJ, Miller SI, Southwick FS, et al. (1993) Acute bacterial meningitis in adults. A review of 493 episodes. N Engl J Med 328: 21–28. - PubMed
-
- Thigpen MC, Whitney CG, Messonnier NE, Zell ER, Lynfield R, et al. (2011) Bacterial meningitis in the United States, 1998–2007. N Engl J Med 364: 2016–2025. - PubMed
-
- van de Beek D (2012) Progress and challenges in bacterial meningitis. Lancet 380: 1623–1624. - PubMed
-
- van de Beek D, de Gans J, Spanjaard L, Weisfelt M, Reitsma JB, et al. (2004) Clinical features and prognostic factors in adults with bacterial meningitis. N Engl J Med 351: 1849–1859. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

