Repositioning for pressure ulcer prevention in adults
- PMID: 24700291
- PMCID: PMC6769133
- DOI: 10.1002/14651858.CD009958.pub2
Repositioning for pressure ulcer prevention in adults
Update in
-
Repositioning for pressure injury prevention in adults.Cochrane Database Syst Rev. 2020 Jun 2;6(6):CD009958. doi: 10.1002/14651858.CD009958.pub3. Cochrane Database Syst Rev. 2020. PMID: 32484259 Free PMC article.
Abstract
Background: A pressure ulcer (PU), also referred to as a 'pressure injury', 'pressure sore', or 'bedsore' is defined as an area of localised tissue damage that is caused by unrelieved pressure, friction or shearing forces on any part of the body. PUs commonly occur in patients who are elderly and less mobile, and carry significant human and economic impacts. Immobility and physical inactivity are considered to be major risk factors for PU development and the manual repositioning of patients in hospital or long-term care is a common pressure ulcer prevention strategy.
Objectives: The objectives of this review were to:1) assess the effects of repositioning on the prevention of PUs in adults, regardless of risk or in-patient setting;2) ascertain the most effective repositioning schedules for preventing PUs in adults; and3) ascertain the incremental resource consequences and costs associated with implementing different repositioning regimens compared with alternate schedules or standard practice.
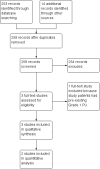
Search methods: We searched the following electronic databases to identify reports of the relevant randomised controlled trials: the Cochrane Wounds Group Specialised Register (searched 06 September 2013), the Cochrane Central Register of Controlled Trials (CENTRAL) (2013, Issue 8); Ovid MEDLINE (1948 to August, Week 4, 2013); Ovid EMBASE (1974 to 2013, Week 35); EBESCO CINAHL (1982 to 30 August 2013); and the reference sections of studies that were included in the review.
Selection criteria: Randomised controlled trials (RCTs), published or unpublished, that assessed the effects of any repositioning schedule or different patient positions and measured PU incidence in adults in any setting.
Data collection and analysis: Two review authors independently performed study selection, risk of bias assessment and data extraction.
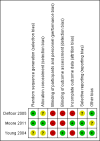
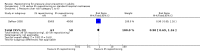
Main results: We included three RCTs and one economic study representing a total of 502 randomised participants from acute and long-term care settings. Two trials compared the 30º and 90º tilt positions using similar repositioning frequencies (there was a small difference in frequency of overnight repositioning in the 90º tilt groups between the trials). The third RCT compared alternative repositioning frequencies.All three studies reported the proportion of patients developing PU of any grade, stage or category. None of the trials reported on pain, or quality of life, and only one reported on cost. All three trials were at high risk of bias.The two trials of 30º tilt vs. 90º were pooled using a random effects model (I² = 69%) (252 participants). The risk ratio for developing a PU in the 30º tilt and the standard 90º position was very imprecise (pooled RR 0.62, 95% CI 0.10 to 3.97, P=0.62, very low quality evidence). This comparison is underpowered and at risk of a Type 2 error (only 21 events).In the third study, a cluster randomised trial, participants were randomised between 2-hourly and 3-hourly repositioning on standard hospital mattresses and 4 hourly and 6 hourly repositioning on viscoelastic foam mattresses. This study was also underpowered and at high risk of bias. The risk ratio for pressure ulcers (any category) with 2-hourly repositioning compared with 3-hourly repositioning on a standard mattress was imprecise (RR 0.90, 95% CI 0.69 to 1.16, very low quality evidence). The risk ratio for pressure ulcers (any category) was compatible with a large reduction and no difference between 4-hourly repositioning and 6-hourly repositioning on viscoelastic foam (RR 0.73, 95% CI 0.53 to 1.02, very low quality evidence).A cost-effectiveness analysis based on data derived from one of the included parallel RCTs compared 3-hourly repositioning using the 30º tilt overnight with standard care consisting of 6-hourly repositioning using the 90º lateral rotation overnight. In this evaluation the only included cost was nursing time. The intervention was reported to be cost saving compared with standard care (nurse time cost per patient €206.6 vs €253.1, incremental difference €-46.5; 95%CI: €-1.25 to €-74.60).
Authors' conclusions: Repositioning is an integral component of pressure ulcer prevention and treatment; it has a sound theoretical rationale, and is widely recommended and used in practice. The lack of robust evaluations of repositioning frequency and position for pressure ulcer prevention mean that great uncertainty remains but it does not mean these interventions are ineffective since all comparisons are grossly underpowered. Current evidence is small in volume and at risk of bias and there is currently no strong evidence of a reduction in pressure ulcers with the 30° tilt compared with the standard 90º position or good evidence of an effect of repositioning frequency. There is a clear need for high-quality, adequately-powered trials to assess the effects of position and optimal frequency of repositioning on pressure ulcer incidence.The limited data derived from one economic evaluation means it remains unclear whether repositioning every 3 hours using the 30º tilt is less costly in terms of nursing time and more effective than standard care involving repositioning every 6 hours using a 90º tilt.
Conflict of interest statement
Dr Brigid Gillespie; Dr Wendy Chaboyer; Dr Elizabeth McInnes; Dr Bridie Kent; Dr Jennifer Whitty and Dr Lukman Thalib have no conflicts of interest to declare.
Figures






References
References to studies included in this review
-
- Defloor T, Bacquer D, Grypdonck MH. The effect of various combinations of turning and pressure reducing devices on the incidence of pressure ulcers. International Journal of Nursing Studies 2005;42(1):37‐46. - PubMed
-
- Moore Z, Cowman S, Conroy RM. A randomised controlled clinical trial of repositioning, using the 30o tilt, for the prevention of pressure ulcers. Journal of Clinical Nursing 2011;20(17‐18):2633‐44. - PubMed
-
- Young T. The 30 degree tilt position vs the 90 degree lateral and supine positions in reducing the incidence of non‐blanching erythema in a hospital inpatient population: a randomised controlled trial. Journal of Tissue Viability 2004;14(3):88, 90, 92‐6. - PubMed
References to studies excluded from this review
-
- Vanderwee K, Grypdonck MHF, Bacquer D, Defloor T. Effectiveness of turning with unequal time intervals on the incidence of pressure ulcer lesions. Journal of Advanced Nursing 2007;57(1):59‐68. - PubMed
References to ongoing studies
-
- TURN Study. Ongoing study Started in 2008 and completed in June 2011.
Additional references
-
- Allman RM, Goode PS, Patrick MM, Burst N, Bartolucci AA. Pressure ulcer risk factors among hospitalised patients with activity limitation. JAMA 1995;273:865‐70. - PubMed
-
- Allman RM. Pressure ulcer prevalence, incidence, risk factors, and impact. Clinics in Geriatric Medicine 1997;13(3):421‐36. - PubMed
-
- Australian Institute of Health and Welfare. Australian Hospital Statistics 2007‐08. Health services series no. 33. Cat. No. HSE 71. Report. Canberra: Australian Governement, 2009.
-
- Australian Safety and Compensation Council. The costs of work‐related injury and illness for Australian employers, workers and the community. ASCC. Canberra, 2009.
-
- Australian Wound Management Association. Pan Pacific clinical practice guideline for the prevention and management of pressure Injury. Clinical GuidelineOctober 2011.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

