Do heart and respiratory rate variability improve prediction of extubation outcomes in critically ill patients?
- PMID: 24713049
- PMCID: PMC4057494
- DOI: 10.1186/cc13822
Do heart and respiratory rate variability improve prediction of extubation outcomes in critically ill patients?
Erratum in
- Crit Care. 2014;18(6):620
Abstract
Introduction: Prolonged ventilation and failed extubation are associated with increased harm and cost. The added value of heart and respiratory rate variability (HRV and RRV) during spontaneous breathing trials (SBTs) to predict extubation failure remains unknown.
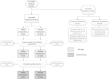
Methods: We enrolled 721 patients in a multicenter (12 sites), prospective, observational study, evaluating clinical estimates of risk of extubation failure, physiologic measures recorded during SBTs, HRV and RRV recorded before and during the last SBT prior to extubation, and extubation outcomes. We excluded 287 patients because of protocol or technical violations, or poor data quality. Measures of variability (97 HRV, 82 RRV) were calculated from electrocardiogram and capnography waveforms followed by automated cleaning and variability analysis using Continuous Individualized Multiorgan Variability Analysis (CIMVA™) software. Repeated randomized subsampling with training, validation, and testing were used to derive and compare predictive models.
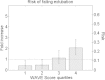
Results: Of 434 patients with high-quality data, 51 (12%) failed extubation. Two HRV and eight RRV measures showed statistically significant association with extubation failure (P <0.0041, 5% false discovery rate). An ensemble average of five univariate logistic regression models using RRV during SBT, yielding a probability of extubation failure (called WAVE score), demonstrated optimal predictive capacity. With repeated random subsampling and testing, the model showed mean receiver operating characteristic area under the curve (ROC AUC) of 0.69, higher than heart rate (0.51), rapid shallow breathing index (RBSI; 0.61) and respiratory rate (0.63). After deriving a WAVE model based on all data, training-set performance demonstrated that the model increased its predictive power when applied to patients conventionally considered high risk: a WAVE score >0.5 in patients with RSBI >105 and perceived high risk of failure yielded a fold increase in risk of extubation failure of 3.0 (95% confidence interval (CI) 1.2 to 5.2) and 3.5 (95% CI 1.9 to 5.4), respectively.
Conclusions: Altered HRV and RRV (during the SBT prior to extubation) are significantly associated with extubation failure. A predictive model using RRV during the last SBT provided optimal accuracy of prediction in all patients, with improved accuracy when combined with clinical impression or RSBI. This model requires a validation cohort to evaluate accuracy and generalizability.
Trial registration: ClinicalTrials.gov NCT01237886. Registered 13 October 2010.
Figures
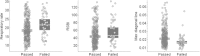

Similar articles
-
[Trend analysis of rapid shallow breathing indices during spontaneous breathing trial may improve predictive accuracy of extubation success].Zhonghua Yi Xue Za Zhi. 2013 Jan 29;93(5):357-61. Zhonghua Yi Xue Za Zhi. 2013. PMID: 23660208 Chinese.
-
A decision-tree model for predicting extubation outcome in elderly patients after a successful spontaneous breathing trial.Anesth Analg. 2010 Nov;111(5):1211-8. doi: 10.1213/ANE.0b013e3181f4e82e. Epub 2010 Sep 14. Anesth Analg. 2010. PMID: 20841406
-
Prediction of extubation outcome in mechanically ventilated patients: Development and validation of the Extubation Predictive Score (ExPreS).PLoS One. 2021 Mar 18;16(3):e0248868. doi: 10.1371/journal.pone.0248868. eCollection 2021. PLoS One. 2021. PMID: 33735250 Free PMC article.
-
The Usefulness of the Rapid Shallow Breathing Index in Predicting Successful Extubation: A Systematic Review and Meta-analysis.Chest. 2022 Jan;161(1):97-111. doi: 10.1016/j.chest.2021.06.030. Epub 2021 Jun 26. Chest. 2022. PMID: 34181953
-
Prediction of extubation outcome in critically ill patients: a systematic review and meta-analysis.Crit Care. 2021 Nov 15;25(1):391. doi: 10.1186/s13054-021-03802-3. Crit Care. 2021. PMID: 34782003 Free PMC article.
Cited by
-
Performance and comparison of artificial intelligence and human experts in the detection and classification of colonic polyps.BMC Gastroenterol. 2022 Dec 13;22(1):517. doi: 10.1186/s12876-022-02605-2. BMC Gastroenterol. 2022. PMID: 36513975 Free PMC article.
-
Cardiopulmonary coupling indices to assess weaning readiness from mechanical ventilation.Sci Rep. 2021 Aug 6;11(1):16014. doi: 10.1038/s41598-021-95282-2. Sci Rep. 2021. PMID: 34362950 Free PMC article.
-
Role of heart rate variability in predicting tracheal extubation failure: a systematic review and meta-analysis.Br J Anaesth. 2025 Apr;134(4):1225-1229. doi: 10.1016/j.bja.2024.12.030. Epub 2025 Jan 23. Br J Anaesth. 2025. PMID: 39855929 Free PMC article. No abstract available.
-
High Breath-by-Breath Variability Is Associated With Extubation Failure in Children.Crit Care Med. 2020 Aug;48(8):1165-1174. doi: 10.1097/CCM.0000000000004418. Crit Care Med. 2020. PMID: 32697487 Free PMC article.
-
Impact of ventilatory modes on the breathing variability in mechanically ventilated infants.Front Pediatr. 2014 Nov 25;2:132. doi: 10.3389/fped.2014.00132. eCollection 2014. Front Pediatr. 2014. PMID: 25505779 Free PMC article.
References
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

