Childhood obesity and its impact on the development of adolescent PCOS
- PMID: 24715515
- PMCID: PMC4103796
- DOI: 10.1055/s-0034-1371092
Childhood obesity and its impact on the development of adolescent PCOS
Abstract
Obesity exacerbates the reproductive and metabolic manifestations of polycystic ovary syndrome (PCOS). The symptoms of PCOS often begin in adolescence, and the rising prevalence of peripubertal obesity has prompted concern that the prevalence and severity of adolescent PCOS is increasing in parallel. Recent data have disclosed a high prevalence of hyperandrogenemia among peripubertal adolescents with obesity, suggesting that such girls are indeed at risk for developing PCOS. Obesity may impact the risk of PCOS via insulin resistance and compensatory hyperinsulinemia, which augments ovarian/adrenal androgen production and suppresses sex hormone-binding globulin (SHBG), thereby increasing androgen bioavailability. Altered luteinizing hormone (LH) secretion plays an important role in the pathophysiology of PCOS, and although obesity is generally associated with relative reductions of LH, higher LH appears to be the best predictor of increased free testosterone among peripubertal girls with obesity. Other potential mechanisms of obesity-associated hyperandrogenemia include enhanced androgen production in an expanded fat mass and potential effects of abnormal adipokine/cytokine levels. Adolescents with PCOS are at risk for comorbidities such as metabolic syndrome and impaired glucose tolerance, and concomitant obesity compounds these risks. For all of these reasons, weight loss represents an important therapeutic target in obese adolescents with PCOS.
Thieme Medical Publishers 333 Seventh Avenue, New York, NY 10001, USA.
Figures

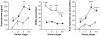
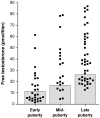

References
-
- [Anonymous], ACOG Committee on Practice Bulletins--Gynecology ACOG Practice Bulletin No. 108: polycystic ovary syndrome. Obstet Gynecol. 2009;114(4):936–949. - PubMed
-
- March WA, Moore VM, Willson KJ, Phillips DI, Norman RJ, Davies MJ. The prevalence of polycystic ovary syndrome in a community sample assessed under contrasting diagnostic criteria. Hum Reprod. 2010;25(2):544–551. - PubMed
-
- Moran LJ, Misso ML, Wild RA, Norman RJ. Impaired glucose tolerance, type 2 diabetes and metabolic syndrome in polycystic ovary syndrome: a systematic review and meta-analysis. Hum Reprod Update. 2010;16(4):347–363. - PubMed
-
- Lim SS, Davies MJ, Norman RJ, Moran LJ. Overweight, obesity and central obesity in women with polycystic ovary syndrome: a systematic review and meta-analysis. Hum Reprod Update. 2012;18(6):618–637. - PubMed
-
- McCartney CR, Prendergast KA, Chhabra S, et al. The association of obesity and hyperandrogenemia during the pubertal transition in girls: obesity as a potential factor in the genesis of postpubertal hyperandrogenism. J Clin Endocrinol Metab. 2006;91(5):1714–1722. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

