A population health approach to reducing observational intensity bias in health risk adjustment: cross sectional analysis of insurance claims
- PMID: 24721838
- PMCID: PMC3982718
- DOI: 10.1136/bmj.g2392
A population health approach to reducing observational intensity bias in health risk adjustment: cross sectional analysis of insurance claims
Abstract
Objective: To compare the performance of two new approaches to risk adjustment that are free of the influence of observational intensity with methods that depend on diagnoses listed in administrative databases.
Setting: Administrative data from the US Medicare program for services provided in 2007 among 306 US hospital referral regions.
Design: Cross sectional analysis.
Participants: 20% sample of fee for service Medicare beneficiaries residing in one of 306 hospital referral regions in the United States in 2007 (n = 5,153,877).
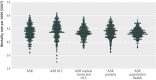
Main outcome measures: The effect of health risk adjustment on age, sex, and race adjusted mortality and spending rates among hospital referral regions using four indices: the standard Centers for Medicare and Medicaid Services--Hierarchical Condition Categories (HCC) index used by the US Medicare program (calculated from diagnoses listed in Medicare's administrative database); a visit corrected HCC index (to reduce the effects of observational intensity on frequency of diagnoses); a poverty index (based on US census); and a population health index (calculated using data on incidence of hip fractures and strokes, and responses from a population based annual survey of health from the Centers for Disease Control and Prevention).
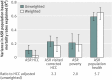
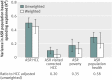
Results: Estimated variation in age, sex, and race adjusted mortality rates across hospital referral regions was reduced using the indices based on population health, poverty, and visit corrected HCC, but increased using the standard HCC index. Most of the residual variation in age, sex, and race adjusted mortality was explained (in terms of weighted R2) by the population health index: R2=0.65. The other indices explained less: R2=0.20 for the visit corrected HCC index; 0.19 for the poverty index, and 0.02 for the standard HCC index. The residual variation in age, sex, race, and price adjusted spending per capita across the 306 hospital referral regions explained by the indices (in terms of weighted R2) were 0.50 for the standard HCC index, 0.21 for the population health index, 0.12 for the poverty index, and 0.07 for the visit corrected HCC index, implying that only a modest amount of the variation in spending can be explained by factors most closely related to mortality. Further, once the HCC index is visit corrected it accounts for almost none of the residual variation in age, sex, and race adjusted spending.
Conclusion: Health risk adjustment using either the poverty index or the population health index performed substantially better in terms of explaining actual mortality than the indices that relied on diagnoses from administrative databases; the population health index explained the majority of residual variation in age, sex, and race adjusted mortality. Owing to the influence of observational intensity on diagnoses from administrative databases, the standard HCC index over-adjusts for regional differences in spending. Research to improve health risk adjustment methods should focus on developing measures of risk that do not depend on observation influenced diagnoses recorded in administrative databases.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure form at
Figures
References
-
- The Dartmouth atlas of health care. 2014. www.dartmouthatlas.org.
-
- NHS. RightCare. 2014. www.rightcare.nhs.uk/index.php/nhs-atlas.
-
- VPM Atlas. 2014. www.atlasvpm.org/avpm.
-
- Move your dot™: measuring, evaluating, and reducing hospital mortality rates (part 1). IHI Innovation Series white paper. Institute for Healthcare Improvement, 2003. 2013. www.IHI.org.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
