Chronic hypertension and pregnancy outcomes: systematic review and meta-analysis
- PMID: 24735917
- PMCID: PMC3988319
- DOI: 10.1136/bmj.g2301
Chronic hypertension and pregnancy outcomes: systematic review and meta-analysis
Abstract
Objective: To provide an accurate assessment of complications of pregnancy in women with chronic hypertension, including comparison with population pregnancy data (US) to inform pre-pregnancy and antenatal management strategies.
Design: Systematic review and meta-analysis.
Data sources: Embase, Medline, and Web of Science were searched without language restrictions, from first publication until June 2013; the bibliographies of relevant articles and reviews were hand searched for additional reports.
Study selection: Studies involving pregnant women with chronic hypertension, including retrospective and prospective cohorts, population studies, and appropriate arms of randomised controlled trials, were included.
Data extraction: Pooled incidence for each pregnancy outcome was reported and, for US studies, compared with US general population incidence from the National Vital Statistics Report (2006).
Results: 55 eligible studies were identified, encompassing 795,221 pregnancies. Women with chronic hypertension had high pooled incidences of superimposed pre-eclampsia (25.9%, 95% confidence interval 21.0% to 31.5 %), caesarean section (41.4%, 35.5% to 47.7%), preterm delivery <37 weeks' gestation (28.1% (22.6 to 34.4%), birth weight <2500 g (16.9%, 13.1% to 21.5%), neonatal unit admission (20.5%, 15.7% to 26.4%), and perinatal death (4.0%, 2.9% to 5.4%). However, considerable heterogeneity existed in the reported incidence of all outcomes (τ(2)=0.286-0.766), with a substantial range of incidences in individual studies around these averages; additional meta-regression did not identify any influential demographic factors. The incidences (the meta-analysis average from US studies) of adverse outcomes in women with chronic hypertension were compared with women from the US national population dataset and showed higher risks in those with chronic hypertension: relative risks were 7.7 (95% confidence interval 5.7 to 10.1) for superimposed pre-eclampsia compared with pre-eclampsia, 1.3 (1.1 to 1.5) for caesarean section, 2.7 (1.9 to 3.6) for preterm delivery <37 weeks' gestation, 2.7 (1.9 to 3.8) for birth weight <2500 g, 3.2 (2.2 to 4.4) for neonatal unit admission, and 4.2 (2.7 to 6.5) for perinatal death.
Conclusions: This systematic review, reporting meta-analysed data from studies of pregnant women with chronic hypertension, shows that adverse outcomes of pregnancy are common and emphasises a need for heightened antenatal surveillance. A consistent strategy to study women with chronic hypertension is needed, as previous study designs have been diverse. These findings should inform counselling and contribute to optimisation of maternal health, drug treatment, and pre-pregnancy management in women affected by chronic hypertension.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure form at
Figures

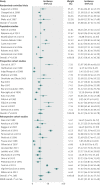
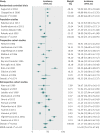
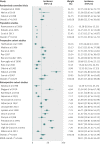



Comment in
-
Chronic hypertension during pregnancy.BMJ. 2014 Apr 15;348:g2655. doi: 10.1136/bmj.g2655. BMJ. 2014. PMID: 24736417 No abstract available.
References
-
- Haddad B, Sibai BM. Chronic hypertension in pregnancy. Ann Med 1999;31:246-52. - PubMed
-
- Livingston JC, Sibai BM. Chronic hypertension in pregnancy. Obstet Gynecol Clin North Am 2001;28:447-63. - PubMed
-
- Yoder SR, Thornburg LL, Bisognano JD. Hypertension in pregnancy and women of childbearing age. Am J Med 2009;122:890-5. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
