Exhaled breath profiling for diagnosing acute respiratory distress syndrome
- PMID: 24767549
- PMCID: PMC4021554
- DOI: 10.1186/1471-2466-14-72
Exhaled breath profiling for diagnosing acute respiratory distress syndrome
Abstract
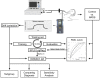
Background: The acute respiratory distress syndrome (ARDS) is a common, devastating complication of critical illness that is characterized by pulmonary injury and inflammation. The clinical diagnosis may be improved by means of objective biological markers. Electronic nose (eNose) technology can rapidly and non-invasively provide breath prints, which are profiles of volatile metabolites in the exhaled breath. We hypothesized that breath prints could facilitate accurate diagnosis of ARDS in intubated and ventilated intensive care unit (ICU) patients.
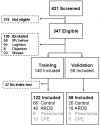
Methods: Prospective single-center cohort study with training and temporal external validation cohort. Breath of newly intubated and mechanically ventilated ICU-patients was analyzed using an electronic nose within 24 hours after admission. ARDS was diagnosed and classified by the Berlin clinical consensus definition. The eNose was trained to recognize ARDS in a training cohort and the diagnostic performance was evaluated in a temporal external validation cohort.
Results: In the training cohort (40 patients with ARDS versus 66 controls) the diagnostic model for ARDS showed a moderate discrimination, with an area under the receiver-operator characteristic curve (AUC-ROC) of 0.72 (95%-confidence interval (CI): 0.63-0.82). In the external validation cohort (18 patients with ARDS versus 26 controls) the AUC-ROC was 0.71 [95%-CI: 0.54 - 0.87]. Restricting discrimination to patients with moderate or severe ARDS versus controls resulted in an AUC-ROC of 0.80 [95%-CI: 0.70 - 0.90]. The exhaled breath profile from patients with cardiopulmonary edema and pneumonia was different from that of patients with moderate/severe ARDS.
Conclusions: An electronic nose can rapidly and non-invasively discriminate between patients with and without ARDS with modest accuracy. Diagnostic accuracy increased when only moderate and severe ARDS patients were considered. This implicates that breath analysis may allow for rapid, bedside detection of ARDS, especially if our findings are reproduced using continuous exhaled breath profiling.
Trial registration: NTR2750, registered 11 February 2011.
Figures
Similar articles
-
Breath metabolomics for diagnosis of acute respiratory distress syndrome.Crit Care. 2024 Mar 23;28(1):96. doi: 10.1186/s13054-024-04882-7. Crit Care. 2024. PMID: 38521944 Free PMC article.
-
Exhaled breath metabolomics as a noninvasive diagnostic tool for acute respiratory distress syndrome.Eur Respir J. 2014 Jul;44(1):188-97. doi: 10.1183/09031936.00005614. Epub 2014 Apr 17. Eur Respir J. 2014. PMID: 24743964
-
Diagnosis of acute respiratory distress syndrome (DARTS) by bedside exhaled breath octane measurements in invasively ventilated patients: protocol of a multicentre observational cohort study.Ann Transl Med. 2021 Aug;9(15):1262. doi: 10.21037/atm-21-1384. Ann Transl Med. 2021. PMID: 34532399 Free PMC article.
-
Diagnosis of acute respiratory distress syndrome by exhaled breath analysis.Ann Transl Med. 2018 Jan;6(2):33. doi: 10.21037/atm.2018.01.17. Ann Transl Med. 2018. PMID: 29430450 Free PMC article. Review.
-
Predictive Modeling of Acute Respiratory Distress Syndrome Using Machine Learning: Systematic Review and Meta-Analysis.J Med Internet Res. 2025 May 13;27:e66615. doi: 10.2196/66615. J Med Internet Res. 2025. PMID: 40359510 Free PMC article.
Cited by
-
Breath analysis for detection and trajectory monitoring of acute respiratory distress syndrome in swine.ERJ Open Res. 2022 Feb 14;8(1):00154-2021. doi: 10.1183/23120541.00154-2021. eCollection 2022 Jan. ERJ Open Res. 2022. PMID: 35174248 Free PMC article.
-
BreathDx - molecular analysis of exhaled breath as a diagnostic test for ventilator-associated pneumonia: protocol for a European multicentre observational study.BMC Pulm Med. 2017 Jan 3;17(1):1. doi: 10.1186/s12890-016-0353-7. BMC Pulm Med. 2017. PMID: 28049457 Free PMC article.
-
Breath metabolomics for diagnosis of acute respiratory distress syndrome.Crit Care. 2024 Mar 23;28(1):96. doi: 10.1186/s13054-024-04882-7. Crit Care. 2024. PMID: 38521944 Free PMC article.
-
Precision Medicine in Neonates: Future Perspectives for the Lung.Front Pediatr. 2020 Oct 30;8:586061. doi: 10.3389/fped.2020.586061. eCollection 2020. Front Pediatr. 2020. PMID: 33251166 Free PMC article. Review.
-
Exhaled Biomarkers for Point-of-Care Diagnosis: Recent Advances and New Challenges in Breathomics.Micromachines (Basel). 2023 Feb 4;14(2):391. doi: 10.3390/mi14020391. Micromachines (Basel). 2023. PMID: 36838091 Free PMC article. Review.
References
-
- Ards Definition Task Force T. Acute respiratory distress syndrome: The berlin definition. JAMA. 2012;307:2526–2533. - PubMed
-
- Thille AW, Esteban A, Fernández-Segoviano P, Rodriguez J-M, Aramburu J-A, Peñuelas O, Cortés-Puch I, Cardinal-Fernández P, Lorente JA, Frutos-Vivar F. Comparison of the Berlin definition for acute respiratory distress syndrome with autopsy. Am J Respir Crit Care Med. 2013;187:761–767. doi: 10.1164/rccm.201211-1981OC. - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

