In-game Management of Common Joint Dislocations
- PMID: 24790695
- PMCID: PMC4000468
- DOI: 10.1177/1941738113499721
In-game Management of Common Joint Dislocations
Abstract
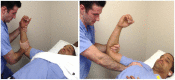
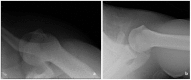
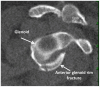
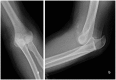
Context: Sideline management of sports-related joint dislocations often places the treating medical professional in a challenging position. These injuries frequently require prompt evaluation, diagnosis, reduction, and postreduction management before they can be evaluated at a medical facility. Our objective is to review the mechanism, evaluation, reduction, and postreduction management of sports-related dislocations to the shoulder, elbow, finger, knee, patella, and ankle joints.
Evidence acquisition: A literature review was performed using the PubMed database to evaluate previous and current publications focused on joint dislocations. This review focused on articles published between 1980 and 2013.
Study design: Clinical review.
Level of evidence: Level 4.
Results: The clinician should weigh the benefits and risks of on-field reduction based on their knowledge of the injury and the presence of associated injuries.
Conclusion: When properly evaluated and diagnosed, most sports-related dislocations can be reduced and initially managed at the game.
Keywords: dislocation; joint; reduction; review; sideline; sport.
Conflict of interest statement
The following authors declared potential conflicts of interest: Matthew V. Smith, MD, is a consultant for ISTO Technologies, Inc, and Jeremy J. McCormick, MD, has grants or grants pending from Wright Medical Technologies, Inc., Midwest Stone, Inc., and Integra Life Sciences, Inc., and received payments for lectures from Synthes, Inc.
Figures
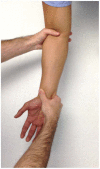
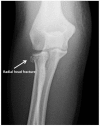
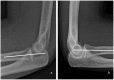
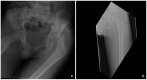
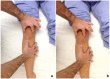
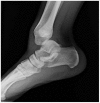
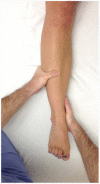
Similar articles
-
Pitch-side management of acute shoulder dislocations: a conceptual review.BMJ Open Sport Exerc Med. 2017 Mar 12;2(1):e000116. doi: 10.1136/bmjsem-2016-000116. eCollection 2016. BMJ Open Sport Exerc Med. 2017. PMID: 28879022 Free PMC article.
-
Sideline coverage: when to get radiographs? A review of clinical decision tools.Sports Health. 2014 May;6(3):274-8. doi: 10.1177/1941738114529701. Sports Health. 2014. PMID: 24790698 Free PMC article.
-
Managing dislocations of the hip, knee, and ankle in the emergency department.Emerg Med Pract. 2017 Dec;19(12):1-28. Epub 2017 Dec 1. Emerg Med Pract. 2017. PMID: 29185671 Review.
-
Sideline Management of Joint Dislocations.Curr Sports Med Rep. 2016 May-Jun;15(3):140-53. doi: 10.1249/JSR.0000000000000266. Curr Sports Med Rep. 2016. PMID: 27172077
-
Jam Injuries of the Finger: Diagnosis and Management of Injuries to the Interphalangeal Joints Across Multiple Sports and Levels of Experience.Sports Health. 2016 Sep;8(5):469-78. doi: 10.1177/1941738116658643. Epub 2016 Jul 15. Sports Health. 2016. PMID: 27421747 Free PMC article. Review.
Cited by
-
Closed-Reduction Techniques for Glenohumeral-, Patellofemoral-, and Interphalangeal-Joint Dislocations.J Athl Train. 2020 Jul 15;55(8):0. doi: 10.4085/1062-6050-0311.19. J Athl Train. 2020. PMID: 32688375 Free PMC article. Review.
-
Prevalence and risk factors for nerve injury following shoulder dislocation.Musculoskelet Surg. 2023 Sep;107(3):345-350. doi: 10.1007/s12306-022-00769-4. Epub 2022 Nov 29. Musculoskelet Surg. 2023. PMID: 36445531 Free PMC article.
-
Mid- to long-term functional outcome and return to sport after elbow dislocation in bouldering: a clinical retrospective cohort study.Arch Orthop Trauma Surg. 2024 Jul;144(7):3145-3151. doi: 10.1007/s00402-024-05397-0. Epub 2024 Jun 13. Arch Orthop Trauma Surg. 2024. PMID: 38869659 Free PMC article.
-
Posterior shoulder dislocation in a 10-year-old child: Case report.Ann Med Surg (Lond). 2018 Aug 18;33:32-35. doi: 10.1016/j.amsu.2018.08.005. eCollection 2018 Sep. Ann Med Surg (Lond). 2018. PMID: 30167300 Free PMC article.
-
National Athletic Trainers' Association Position Statement: Immediate Management of Appendicular Joint Dislocations.J Athl Train. 2018 Dec;53(12):1117-1128. doi: 10.4085/1062-6050-97-12. Epub 2019 Jan 4. J Athl Train. 2018. PMID: 30609383 Free PMC article.
References
-
- Anakwe RE, Middleton SD, Jenkins PJ, McQueen MM, Court-Brown CM. Patient-reported outcomes after simple dislocation of the elbow. J Bone Joint Surg Am. 2011;93:1220-1226 - PubMed
-
- Benjamin HJ, Hang BT. Common acute upper extremity injuries in sports. Clin Pediatric Emerg Med. 2007;8(1):15-30
-
- Cohen MS, Hastings H, II. Acute elbow dislocation: evaluation and management. J Am Acad Orthop Surg. 1998;6:15-23 - PubMed
-
- Davids JR, Talbott RD. Luxatio erecta humeri. A case report. Clin Orthop Relat Res. 1990;(252):144-149 - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

