Pediatric non-alcoholic fatty liver disease: New insights and future directions
- PMID: 24799990
- PMCID: PMC4009477
- DOI: 10.4254/wjh.v6.i4.217
Pediatric non-alcoholic fatty liver disease: New insights and future directions
Abstract
One of the most common complications of childhood obesity is the non-alcoholic fatty liver disease (NAFLD), which is the most common form of liver disease in children. NAFLD is defined by hepatic fat infiltration > 5% hepatocytes, as assessed by liver biopsy, in the absence of excessive alcohol intake, viral, autoimmune and drug-induced liver disease. It encompasses a wide spectrum of liver diseases ranging from simple steatosis to non-alcoholic steatohepatitis, which, in turn, can evolve into cirrhosis and end stage liver disease. Obesity and insulin resistance are the main risk factors for pediatric NAFLD. In fact, NAFLD is strongly associated with the clinical features of insulin resistance especially the metabolic syndrome, prediabetes and type 2 diabetes mellitus (T2D). In particular, it has been clearly shown in obese youth that the prevalence of metabolic syndrome, pre-diabetes and type 2 diabetes increases with NAFLD severity progression. Evidence that not all of the obese patients develop NAFLD suggests that the disease progression is likely to depend on complex interplay between environmental factors and genetic predisposition. Recently, a non-synonymous SNP (rs738409), characterized by a C to G substitution encoding an isoleucine to methionine substitution at the amino acid position 148 in the patatin like phospholipase containing domain 3 gene (PNPLA3), has been associated with hepatic steatosis in a multiethnic cohort of adults as well as in children. Another important polymorphisms that acts with PNPLA3 to convey susceptibility to fatty liver in obese youths is the rs1260326 polymorphism in the glucokinase regulatory protein. The pharmacological approach in NAFLD children poorly adherent to or being unresponsive/partially responsive to lifestyle changes, is aimed at acting upon specific targets involved in the pathogenesis. There are some therapeutic approaches that are being studied in children. This article reviews the current knowledge regarding the pediatric fatty liver disease, the new insights and the future directions.
Keywords: Fructose; Glucokinase regulatory protein; Insulin resistance; Non alcoholic fatty liver disease; Obesity; PNPLA3.
Figures
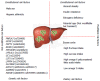
References
-
- Schwimmer JB, Deutsch R, Kahen T, Lavine JE, Stanley C, Behling C. Prevalence of fatty liver in children and adolescents. Pediatrics. 2006;118:1388–1393. - PubMed
-
- Brunt EM. Pathology of nonalcoholic fatty liver disease. Nat Rev Gastroenterol Hepatol. 2010;7:195–203. - PubMed
-
- Nobili V, Reale A, Alisi A, Morino G, Trenta I, Pisani M, Marcellini M, Raucci U. Elevated serum ALT in children presenting to the emergency unit: Relationship with NAFLD. Dig Liver Dis. 2009;41:749–752. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

