Irritable bowel syndrome: the role of food in pathogenesis and management
- PMID: 24829543
- PMCID: PMC4014048
Irritable bowel syndrome: the role of food in pathogenesis and management
Abstract
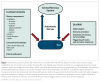
Irritable bowel syndrome (IBS) is a common functional gastrointestinal disorder that affects approximately 10% to 20% of the general adult population in Europe and the Americas and is characterized by abdominal pain and altered bowel habits in the absence of reliable biomarkers. The pathophysiology of IBS is poorly understood and is currently thought to represent a complex interplay among the gut microbiota, low-grade inflammation, impaired mucosal barrier function, visceral hypersensitivity, gut motility, and alterations in the gut-brain axis. In any individual patient, 1 or more of these factors may interact to generate symptoms. Although up to 50% of patients report postprandial exacerbation of symptoms, few studies have critically assessed the role of diet in IBS. Furthermore, although many patients with IBS adopt any one of a host of dietary changes in an attempt to alleviate their symptoms, there has been, up until recently little scientific basis for any dietary recommendation in IBS. This review discusses the contribution of diet to the pathophysiology and symptoms of IBS.
Keywords: FODMAPs; Irritable bowel syndrome; diet; food allergy; food intolerance; gluten; gut hormones.
Figures
References
-
- Lovell RM, Ford AC. Global prevalence of and risk factors for irritable bowel syndrome: a meta-analysis. Clin Gastroenterol Hepatol. 2012;10(7):712–721, e4. - PubMed
-
- Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC. Functional bowel disorders. Gastroenterology. 2006;130(5):1480–1491. - PubMed
-
- Drossman DA, Morris CB, Hu Y, et al. A prospective assessment of bowel habit in irritable bowel syndrome in women: defining an alternator. Gastroenterology. 2005;128(3):580–589. - PubMed
-
- Ludidi S, Conchillo JM, Keszthelyi D, et al. Rectal hypersensitivity as hallmark for irritable bowel syndrome: defining the optimal cutoff. Neurogastroenterol Motil. 2012;24(8):729–733, e345-e346. - PubMed
-
- Dinan TG, Quigley EM, Ahmed SM, et al. Hypothalamic-pituitary-gut axis dysregulation in irritable bowel syndrome: plasma cytokines as a potential bio-marker? Gastroenterology. 2006;130(2):304–311. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
