Ultrasound-guided rectus sheath block or wound infiltration in children: a randomized blinded study of analgesia and bupivacaine absorption
- PMID: 24853314
- PMCID: PMC4125512
- DOI: 10.1111/pan.12438
Ultrasound-guided rectus sheath block or wound infiltration in children: a randomized blinded study of analgesia and bupivacaine absorption
Abstract
Background: Rectus sheath block can provide analgesia following umbilical hernia repair. However, conflicting reports on its analgesic effectiveness exist. No study has investigated plasma local anesthetic concentration following ultrasound-guided rectus sheath block (USGRSB) in children.
Objectives: Compare the effectiveness and bupivacaine absorption following USGRSB or wound infiltration (WI) for umbilical hernia repair in children.
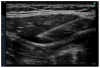
Methods: A randomized blinded study comparing WI with USGRSB in 40 children undergoing umbilical hernia repair was performed. Group WI (n = 20) received wound infiltration 1 mg·kg(-1) 0.25% bupivacaine. Group RS (n = 20) received USGRSB 0.5 mg·kg(-1) 0.25% bupivacaine per side in the posterior rectus sheath compartment. Pain scores and rescue analgesia were recorded. Blood samples were drawn at 0, 10, 20, 30, 45, and 60 min.
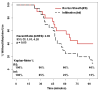
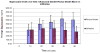
Results: Patients in the WI group had a twofold increased risk of requiring morphine (hazard ratio 2.06, 95% CI 1.01, 4.20, P = 0.05). When required, median time to first morphine dose was longer in the USGRSB group (65.5 min vs. 47.5 min, P = 0.049). Peak plasma bupivacaine concentration was higher following USGRSB than WI (median: 631.9 ng·ml(-1) IQR: 553.9-784.1 vs. 389.7 ng·ml(-1) IQR: 250.5-502.7, P = 0.002). Tmax was longer in the USGRSB group (median 45 min IQR: 30-60 vs. 20 min IQR: 20-45, P = 0.006).
Conclusions: USGRSB provides more effective analgesia than WI for umbilical hernia repair. USGRSB with 1 mg·kg(-1) 0.25% bupivacaine is associated with safe plasma bupivacaine concentration that peaks higher and later than WI. Caution against using larger volumes of higher concentration local anesthetic for USGRSB is advised.
Keywords: age, outpatient; ambulatory, local anesthetics; drugs; drugs, regional; pain, child; pharmacokinetics; ultrasound, regional.
© 2014 John Wiley & Sons Ltd.
Figures

Similar articles
-
Prospective randomized observer-blinded study comparing the analgesic efficacy of ultrasound-guided rectus sheath block and local anaesthetic infiltration for umbilical hernia repair.Br J Anaesth. 2011 Nov;107(5):790-5. doi: 10.1093/bja/aer263. Epub 2011 Aug 19. Br J Anaesth. 2011. PMID: 21856778 Clinical Trial.
-
The Effect of Rectus Sheath Block as a Supplement of General Anesthesia on Postoperative Analgesia in Adult Patient Undergoing Umbilical Hernia Repair.Pril (Makedon Akad Nauk Umet Odd Med Nauki). 2017 Dec 1;38(3):135-142. doi: 10.2478/prilozi-2018-0014. Pril (Makedon Akad Nauk Umet Odd Med Nauki). 2017. PMID: 29668467 Clinical Trial.
-
Comparison of the analgesic efficacy of ultrasound-guided rectus sheath block and local anesthetic infiltration for laparoscopic percutaneous extraperitoneal closure in children.Paediatr Anaesth. 2017 May;27(5):516-523. doi: 10.1111/pan.13085. Epub 2017 Feb 15. Paediatr Anaesth. 2017. PMID: 28198572 Clinical Trial.
-
Comparison of rectus sheath block and local anesthetic for analgesia in pediatric umbilical hernia repair: A systematic review and meta-analysis.Medicine (Baltimore). 2022 Sep 9;101(36):e30391. doi: 10.1097/MD.0000000000030391. Medicine (Baltimore). 2022. PMID: 36086758 Free PMC article.
-
Perineural Liposomal Bupivacaine Is Not Superior to Nonliposomal Bupivacaine for Peripheral Nerve Block Analgesia.Anesthesiology. 2021 Feb 1;134(2):147-164. doi: 10.1097/ALN.0000000000003651. Anesthesiology. 2021. PMID: 33372953
Cited by
-
Comparison between rectus sheath block with 0.25% ropivacaine and local anesthetic infiltration with 0.5% ropivacaine for laparoscopic inguinal hernia repair in children.Nagoya J Med Sci. 2019 Aug;81(3):341-349. doi: 10.18999/nagjms.81.3.341. Nagoya J Med Sci. 2019. PMID: 31579326 Free PMC article. Clinical Trial.
-
The use of ultrasound guidance for perioperative neuraxial and peripheral nerve blocks in children.Cochrane Database Syst Rev. 2019 Feb 27;2(2):CD011436. doi: 10.1002/14651858.CD011436.pub3. Cochrane Database Syst Rev. 2019. PMID: 30820938 Free PMC article.
-
Levobupivacaine concentration for the ultrasound-guided rectus sheath block in children undergoing umbilical skin incision: An up-and-down dose-finding study.Indian J Anaesth. 2024 Feb;68(2):196-199. doi: 10.4103/ija.ija_514_23. Epub 2024 Jan 29. Indian J Anaesth. 2024. PMID: 38435644 Free PMC article. No abstract available.
-
Ultrasound-guided rectus sheath block, caudal analgesia, or surgical site infiltration for pediatric umbilical herniorrhaphy: a prospective, double-blinded, randomized comparison of three regional anesthetic techniques.J Pain Res. 2017 Nov 9;10:2629-2634. doi: 10.2147/JPR.S144259. eCollection 2017. J Pain Res. 2017. PMID: 29184439 Free PMC article.
-
[Peripheral truncal blocks-Overview and assessment].Anaesthesist. 2020 Dec;69(12):860-877. doi: 10.1007/s00101-020-00809-3. Anaesthesist. 2020. PMID: 32620990 Review. German.
References
-
- Finnerty O, Carney J, McDonnell JG. Trunk blocks for abdominal surgery. Anaesthesia. 2010;65(Suppl 1):76–83. - PubMed
-
- Bhalla T, Sawardekar A, Dewhirst E, Jagannathan N, Tobias JD. Ultrasound-guided trunk and core blocks in infants and children. J Anesth. 2013;27:109–23. - PubMed
-
- Willschke H, Bosenberg A, Marhofer P, Johnston S, Kettner SC, Wanzel O, Kapral S. Ultrasonography-guided rectus sheath block in paediatric anaesthesia--a new approach to an old technique. Br J Anaesth. 2006;97:244–9. - PubMed
-
- Willschke H, Bosenberg A, Marhofer P, Johnston S, Kettner S, Eichenberger U, Wanzel O, Kapral S. Ultrasonographic-guided ilioinguinal/iliohypogastric nerve block in pediatric anesthesia: what is the optimal volume? Anesth Analg. 2006;102:1680–4. - PubMed
-
- Weintraud M, Lundblad M, Kettner SC, Willschke H, Kapral S, Lonnqvist PA, Koppatz K, Turnheim K, Bosenberg A, Marhofer P. Ultrasound versus landmark-based technique for ilioinguinal-iliohypogastric nerve blockade in children: the implications on plasma levels of ropivacaine. Anesth Analg. 2009;108:1488–92. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

