Effect of endoscopic sphincterotomy for suspected sphincter of Oddi dysfunction on pain-related disability following cholecystectomy: the EPISOD randomized clinical trial
- PMID: 24867013
- PMCID: PMC4428324
- DOI: 10.1001/jama.2014.5220
Effect of endoscopic sphincterotomy for suspected sphincter of Oddi dysfunction on pain-related disability following cholecystectomy: the EPISOD randomized clinical trial
Abstract
Importance: Abdominal pain after cholecystectomy is common and may be attributed to sphincter of Oddi dysfunction. Management often involves endoscopic retrograde cholangiopancreatography (ERCP) with manometry and sphincterotomy.
Objective: To determine whether endoscopic sphincterotomy reduces pain and whether sphincter manometric pressure is predictive of pain relief.
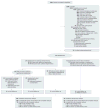
Design, setting, and patients: Multicenter, sham-controlled, randomized trial involving 214 patients with pain after cholecystectomy without significant abnormalities on imaging or laboratory studies, and no prior sphincter treatment or pancreatitis randomly assigned (August 6, 2008-March 23, 2012) to undergo sphincterotomy or sham therapy at 7 referral medical centers. One-year follow-up was blinded. The final follow-up visit was March 21, 2013.
Interventions: After ERCP, patients were randomized 2:1 to sphincterotomy (n = 141) or sham (n = 73) irrespective of manometry findings. Those randomized to sphincterotomy with elevated pancreatic sphincter pressures were randomized again (1:1) to biliary or to both biliary and pancreatic sphincterotomies. Seventy-two were entered into an observational study with conventional ERCP managemeny.
Main outcomes and measures: Success of treatment was defined as less than 6 days of disability due to pain in the prior 90 days both at months 9 and 12 after randomization, with no narcotic use and no further sphincter intervention.
Results: Twenty-seven patients (37%; 95% CI, 25.9%-48.1%) in the sham treatment group vs 32 (23%; 95% CI, 15.8%-29.6%) in the sphincterotomy group experienced successful treatment (adjusted risk difference, -15.6%; 95% CI, -28.0% to -3.3%; P = .01). Of the patients with pancreatic sphincter hypertension, 14 (30%; 95% CI, 16.7%-42.9%) who underwent dual sphincterotomy and 10 (20%; 95% CI, 8.7%-30.5%) who underwent biliary sphincterotomy alone experienced successful treatment. Thirty-seven treated patients (26%; 95% CI,19%-34%) and 25 patients (34%; 95% CI, 23%-45%) in the sham group underwent repeat ERCP interventions (P = .22). Manometry results were not associated with the outcome. No clinical subgroups appeared to benefit from sphincterotomy more than others. Pancreatitis occurred in 15 patients (11%) after primary sphincterotomies and in 11 patients (15%) in the sham group. Of the nonrandomized patients in the observational study group, 5 (24%; 95% CI, 6%-42%) who underwent biliary sphincterotomy, 12 (31%; 95% CI, 16%-45%) who underwent dual sphincterotomy, and 2 (17%; 95% CI, 0%-38%) who did not undergo sphincterotomy had successful treatment.
Conclusions and relevance: In patients with abdominal pain after cholecystectomy undergoing ERCP with manometry, sphincterotomy vs sham did not reduce disability due to pain. These findings do not support ERCP and sphincterotomy for these patients.
Trial registration: clinicaltrials.gov Identifier: NCT00688662.
Conflict of interest statement
All authors have completed and submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Dr Cotton reported that he has received a gift of endoscopic accessories (sphincterotomes) from Cook Medical to be used in the study, to prevent patients being unblinded by getting a bill, consults for Olympus America, and receives royalties from Cook Medical for devices not used in the study. Dr Romagnuolo reported that he consults and receives lecture fees from Olympus and Cook Medical. Dr Fogel reported that he consults for Cook Endoscopy and Boston Scientific and receives lecture fees from Olympus. Dr Tarnasky reported that he consults for and has received lecture fees from Boston Scientific. Dr Aliperti reported that he receives lecture fees from Oklahoma Endoscopy Society. Dr Freeman reported that he has had research grants from Boston Scientific and Cook Endoscopy. Dr Jamidar reported that he consults for Boston Scientific and receives lecture fees from Olympus and Boston Scientific. Drs Serrano reported that he was an employee of NIDDK during key parts of the study. Dr Elta reported that she consults for Olympus. Drs Drossman and Elta reported that they were compensated from the EPISOD grant as consultants. Dr Robuck reported that she was an employee of NIDDK during the key parts of the study and is now retired. All of the others authors had some effort funded by the grant from NIDDK to perform this study and were reimbursed for expenses involved in traveling to investigator meetings. No other disclosures are reported.
Figures

Comment in
-
Why did the sham-treated EPISOD study subjects do so well? Important lessons for research and practice.Gastrointest Endosc. 2019 May;89(5):1054-1055. doi: 10.1016/j.gie.2018.11.006. Epub 2018 Nov 14. Gastrointest Endosc. 2019. PMID: 30447217 Free PMC article. No abstract available.
References
-
- Berger MY, Olde Hartman TC, Bohnen AM. Abdominal symptoms: do they disappear after cholecystectomy? Surg Endosc. 2003;17(11):1723–1728. - PubMed
-
- Behar J, Corazziari E, Guelrud M, Hogan W, Sherman S, Toouli J. Functional gallbladder and sphincter of Oddi disorders. Gastroenterology. 2006;130(5):1498–1509. - PubMed
-
- Sherman S, Lehman GA. Sphincter of Oddi dysfunction: diagnosis and treatment. JOP. 2001;2(6):382–400. - PubMed
-
- Freeman ML, DiSario JA, Nelson DB, et al. Risk factors for post-ERCP pancreatitis: a prospective, multicenter study. Gastrointest Endosc. 2001;54(4):425–434. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

