Blood culture contamination in hospitalized pediatric patients: a single institution experience
- PMID: 24868215
- PMCID: PMC4030119
- DOI: 10.3345/kjp.2014.57.4.178
Blood culture contamination in hospitalized pediatric patients: a single institution experience
Abstract
Purpose: Blood culture is the most important tool for detecting bacteremia in children with fever. However, blood culture contamination rates range from 0.6% to 6.0% in adults; rates for young children have been considered higher than these, although data are limited, especially in Korea. This study determined the contamination rate and risk factors in pediatric patients visiting the emergency room (ER) or being admitted to the ward.
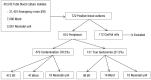
Methods: We conducted a retrospective chart review of blood cultures obtained from children who visited Yonsei Severance Hospital, Korea between 2006 and 2010. Positive blood cultures were labeled as true bacteremia or contamination according to Centers for Disease Control and Prevention/National Healthcare Safety Network definitions for laboratory-confirmed bloodstream infection, after exclusion of cultures drawn from preexisting central lines only.
Results: Among 40,542 blood cultures, 610 were positive, of which 479 were contaminations and 131 were true bacteremia (overall contamination rate, 1.18%). The contamination rate in the ER was significantly higher than in the ward (1.32% vs. 0.66%, P<0.001). The rate was higher in younger children (2.07%, 0.94%, and 0.61% in children aged <1 year, 1-6 years, and >6 years, respectively).
Conclusion: Overall, contamination rates were higher in younger children than in older children, given the difficulty of performing blood sampling in younger children. The contamination rates from the ER were higher than those from the ward, not accounted for only by overcrowding and lack of experience among personnel collecting samples. Further study to investigate other factors affecting contamination should be required.
Keywords: Bacteremia; Blood; Child; Contamination; Culture.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
Similar articles
-
Blood culture contamination in a tertiary care hospital of Saudi Arabia. A one-year study.Saudi Med J. 2020 May;41(5):508-515. doi: 10.15537/smj.2020.5.25052. Saudi Med J. 2020. PMID: 32373918 Free PMC article.
-
C-Reactive Protein Concentration Can Help to Identify Bacteremia in Children Visiting the Emergency Department: A Single Medical Center Experience.Pediatr Emerg Care. 2020 Jun;36(6):291-295. doi: 10.1097/PEC.0000000000001453. Pediatr Emerg Care. 2020. PMID: 29509648
-
Blood Cultures Drawn From Arterial Catheters Are Reliable for the Detection of Bloodstream Infection in Critically Ill Children.Pediatr Crit Care Med. 2018 May;19(5):e213-e218. doi: 10.1097/PCC.0000000000001462. Pediatr Crit Care Med. 2018. PMID: 29406376
-
Utility of blood cultures in febrile children with UTI.Am J Emerg Med. 2002 Jul;20(4):271-4. doi: 10.1053/ajem.2002.33786. Am J Emerg Med. 2002. PMID: 12098170
-
Multidisciplinary team review of best practices for collection and handling of blood cultures to determine effective interventions for increasing the yield of true-positive bacteremias, reducing contamination, and eliminating false-positive central line-associated bloodstream infections.Am J Infect Control. 2015 Nov;43(11):1222-37. doi: 10.1016/j.ajic.2015.06.030. Epub 2015 Aug 19. Am J Infect Control. 2015. PMID: 26298636 Review.
Cited by
-
Rapid molecular assays versus blood culture for bloodstream infections: a systematic review and meta-analysis.EClinicalMedicine. 2025 Jan 10;79:103028. doi: 10.1016/j.eclinm.2024.103028. eCollection 2025 Jan. EClinicalMedicine. 2025. PMID: 39968206 Free PMC article.
-
Using Machine Learning to Predict Bacteremia in Febrile Children Presented to the Emergency Department.Diagnostics (Basel). 2020 May 15;10(5):307. doi: 10.3390/diagnostics10050307. Diagnostics (Basel). 2020. PMID: 32429293 Free PMC article.
-
Clinical Significance of Isolates Known to Be Blood Culture Contaminants in Pediatric Patients.Medicina (Kaunas). 2019 Oct 17;55(10):696. doi: 10.3390/medicina55100696. Medicina (Kaunas). 2019. PMID: 31627324 Free PMC article.
-
Blood culture contamination in a tertiary care hospital: a retrospective three-year study.BMC Infect Dis. 2023 Jul 4;23(1):448. doi: 10.1186/s12879-023-08428-0. BMC Infect Dis. 2023. PMID: 37403044 Free PMC article.
-
Blood culture contamination in a tertiary care hospital of Saudi Arabia. A one-year study.Saudi Med J. 2020 May;41(5):508-515. doi: 10.15537/smj.2020.5.25052. Saudi Med J. 2020. PMID: 32373918 Free PMC article.
References
-
- Norberg A, Christopher NC, Ramundo ML, Bower JR, Berman SA. Contamination rates of blood cultures obtained by dedicated phlebotomy vs intravenous catheter. JAMA. 2003;289:726–729. - PubMed
-
- Marini MA, Truog AW. Reducing false-positive peripheral blood cultures in a pediatric emergency department. J Emerg Nurs. 2013;39:440–446. - PubMed
-
- Bates DW, Lee TH. Rapid classification of positive blood cultures: prospective validation of a multivariate algorithm. JAMA. 1992;267:1962–1966. - PubMed
-
- Center for Disease Control and Prevention; National Healthcare Safety Network (NHSN) Surveillance for central line-associated bloodstream infections [Internet] Atlanta: Center for Disease Control and Prevention; c2013. [cited 2013 Jul 18]. Available from: http://www.cdc.gov/nhsn/acute-care-hospital/clabsi/index.html.
LinkOut - more resources
Full Text Sources
Other Literature Sources