Resolution of pulmonary edema. Thirty years of progress
- PMID: 24881936
- PMCID: PMC4098087
- DOI: 10.1164/rccm.201403-0535OE
Resolution of pulmonary edema. Thirty years of progress
Abstract
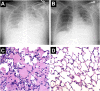
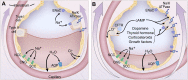
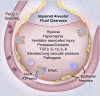
In the last 30 years, we have learned much about the molecular, cellular, and physiological mechanisms that regulate the resolution of pulmonary edema in both the normal and the injured lung. Although the physiological mechanisms responsible for the formation of pulmonary edema were identified by 1980, the mechanisms that explain the resolution of pulmonary edema were not well understood at that time. However, in the 1980s several investigators provided novel evidence that the primary mechanism for removal of alveolar edema fluid depended on active ion transport across the alveolar epithelium. Sodium enters through apical channels, primarily the epithelial sodium channel, and is pumped into the lung interstitium by basolaterally located Na/K-ATPase, thus creating a local osmotic gradient to reabsorb the water fraction of the edema fluid from the airspaces of the lungs. The resolution of alveolar edema across the normally tight epithelial barrier can be up-regulated by cyclic adenosine monophosphate (cAMP)-dependent mechanisms through adrenergic or dopamine receptor stimulation, and by several cAMP-independent mechanisms, including glucocorticoids, thyroid hormone, dopamine, and growth factors. Whereas resolution of alveolar edema in cardiogenic pulmonary edema can be rapid, the rate of edema resolution in most patients with acute respiratory distress syndrome (ARDS) is markedly impaired, a finding that correlates with higher mortality. Several mechanisms impair the resolution of alveolar edema in ARDS, including cell injury from unfavorable ventilator strategies or pathogens, hypoxia, cytokines, and oxidative stress. In patients with severe ARDS, alveolar epithelial cell death is a major mechanism that prevents the resolution of lung edema.
Figures
References
-
- Staub NC. The pathogenesis of pulmonary edema. Prog Cardiovasc Dis. 1980;23:53–80. - PubMed
-
- Staub NC. Pulmonary edema due to increased microvascular permeability. Annu Rev Med. 1981;32:291–312. - PubMed
-
- Staub NC. Pulmonary edema: physiologic approaches to management. Chest. 1978;74:559–564. - PubMed
-
- Wiedemann HP, Wheeler AP, Bernard GR, Thompson BT, Hayden D, deBoisblanc B, Connors AF, Jr, Hite RD, Harabin AL. Comparison of two fluid-management strategies in acute lung injury. N Engl J Med. 2006;354:2564–2575. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

