A comparison study between periosteum and resorbable collagen membrane on iliac block bone graft resorption in the rabbit calvarium
- PMID: 24886656
- PMCID: PMC4024311
- DOI: 10.1186/1746-160X-10-15
A comparison study between periosteum and resorbable collagen membrane on iliac block bone graft resorption in the rabbit calvarium
Abstract
Background: To compare the different resorption patterns between resorbable membrane barrier and periosteum after iliac block bone grafting radiographically and histologically.
Methods: Eighteen mature male rabbits weighing from 2.0 to 2.5 kg were used. The recipient site was the rabbit skull, and autogenous iliac bone was used as the grafting material. The harvested iliac block bones were divided in the following groups: autogenous iliac block bone with preservation of the periosteum (the periosteum group), autogenous iliac block bone covered with a resorbable collagen membrane (Biomesh®, Samyang Co, Korea) after removing the periosteum (the collagen membrane group), and autogenous iliac block bones with removal of the periosteum (the control group). In each experimental group, periosteum or resorbable collagen membrane of the donor site was fixed directed to the periosteum of the recipient site. The specimens were examined macroscopically, radiographically, histologically, and histomorphometrically at every 2, 4, and 8 weeks.
Results: All groups presented excellent bone graft healing state without inflammation, dehiscence, or displacement. The radiolucency increased from mild to moderate in all groups over the experiment. The mean thickness of the upper end of the cortical iliac bone graft was statistically significantly different between the control group and the periosteum group, between the four-week and eight-week control group, and between the four- week and eight-week periosteum group (p & 0.05).
Conclusion: This study suggests that both the periosteum and the resorbable collagen membrane may help to prevent soft tissue infiltration into the bone graft and to reduce bone graft resorption compared to block graft alone.
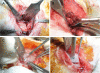
Figures





Similar articles
-
Effect of periosteum attached to autogenous iliac block bone graft on bone resorption in rabbits.J Craniofac Surg. 2015 May;26(3):642-6. doi: 10.1097/SCS.0000000000001417. J Craniofac Surg. 2015. PMID: 25933150
-
Guided bone regeneration at the donor site of iliac bone grafts for future use as autogenous grafts.Plast Reconstr Surg. 2005 Sep 15;116(4):1068-75; discussion 1076. doi: 10.1097/01.prs.0000178783.44190.ec. Plast Reconstr Surg. 2005. PMID: 16163096
-
Effect of isolation of periosteum and dura on the healing of rabbit calvarial inlay bone grafts.Plast Reconstr Surg. 2001 Feb;107(2):454-62. doi: 10.1097/00006534-200102000-00022. Plast Reconstr Surg. 2001. PMID: 11214061
-
The Effect of Membrane Coverage on the Resorption of Autogenous Intraoral Block Grafts in Horizontal Ridge Augmentation: A Systematic Review of Literature and Meta-Analysis: Inevitability or an Iatrogenic Vulnerability?J Evid Based Dent Pract. 2018 Dec;18(4):275-289. doi: 10.1016/j.jebdp.2017.11.001. Epub 2017 Nov 21. J Evid Based Dent Pract. 2018. PMID: 30514442
-
Autogenous bone harvesting and grafting in advanced jaw resorption: morbidity, resorption and implant survival.Eur J Oral Implantol. 2014 Summer;7 Suppl 2:S203-17. Eur J Oral Implantol. 2014. PMID: 24977256 Review.
Cited by
-
Biomimetic characteristics of mussel adhesive protein-loaded collagen membrane in guided bone regeneration of rabbit calvarial defects.J Periodontal Implant Sci. 2018 Oct 24;48(5):305-316. doi: 10.5051/jpis.2018.48.5.305. eCollection 2018 Oct. J Periodontal Implant Sci. 2018. PMID: 30405938 Free PMC article.
-
Allogenic Bone Graft Enriched by Periosteal Stem Cell and Growth Factors for Osteogenesis in Critical Size Bone Defect in Rabbit Model: Histopathological and Radiological Evaluation.Iran J Pathol. 2020 Summer;15(3):205-216. doi: 10.30699/ijp.2020.101715.2013. Epub 2020 Apr 21. Iran J Pathol. 2020. PMID: 32754216 Free PMC article.
-
Effect of Isolating the Periosteum With a Resorbable Barrier Membrane on Neoangiogenesis in Guided Bone Regeneration: An Experimental Study.Cureus. 2025 Mar 24;17(3):e81069. doi: 10.7759/cureus.81069. eCollection 2025 Mar. Cureus. 2025. PMID: 40271309 Free PMC article.
References
-
- Garg AK. Bone biology, harvesting, grafting for dental implants: rationale and clinical applications. 551 Kimberly Drive Carol Stream, IL 60188 USA: Quintessence Pub. Co; 2004.
-
- Keller EE, Tolman DE, Eckert S. Surgical-prosthodontic reconstruction of advanced maxillary bone compromise with autogenous onlay block bone grafts and osseointegrated endosseous implants: a 12 year study of 32 consecutive patients. Int J Oral Maxillofac Implants. 1999;14:197–209. - PubMed
-
- Macewen SW. The growth of bone pp James Maclehose and sons. 1912.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

