Autoimmunity and the gut
- PMID: 24900918
- PMCID: PMC4036413
- DOI: 10.1155/2014/152428
Autoimmunity and the gut
Abstract
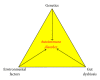
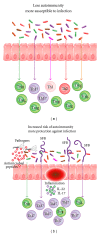
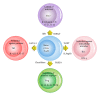
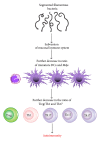
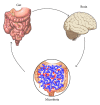
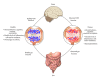
Autoimmune diseases have increased dramatically worldwide since World War II. This is coincidental with the increased production and use of chemicals both in industrial countries and agriculture, as well as the ease of travel from region to region and continent to continent, making the transfer of a pathogen or pathogens from one part of the world to another much easier than ever before. In this review, triggers of autoimmunity are examined, principally environmental. The number of possible environmental triggers is vast and includes chemicals, bacteria, viruses, and molds. Examples of these triggers are given and include the mechanism of action and method by which they bring about autoimmunity.
Figures
Similar articles
-
Infection, vaccines and other environmental triggers of autoimmunity.Autoimmunity. 2005 May;38(3):235-45. doi: 10.1080/08916930500050277. Autoimmunity. 2005. PMID: 16126512
-
Infectious diseases and autoimmunity.J Infect Dev Ctries. 2011 Oct 13;5(10):679-87. doi: 10.3855/jidc.2061. J Infect Dev Ctries. 2011. PMID: 21997935 Review.
-
Environmental Basis of Autoimmunity.Clin Rev Allergy Immunol. 2016 Jun;50(3):287-300. doi: 10.1007/s12016-015-8493-8. Clin Rev Allergy Immunol. 2016. PMID: 25998909 Review.
-
Impact of gut microbiota on gut-distal autoimmunity: a focus on T cells.Immunology. 2019 Apr;156(4):305-318. doi: 10.1111/imm.13037. Epub 2019 Jan 21. Immunology. 2019. PMID: 30560993 Free PMC article. Review.
-
Animal models used to examine the role of the environment in the development of autoimmune disease: findings from an NIEHS Expert Panel Workshop.J Autoimmun. 2012 Dec;39(4):285-93. doi: 10.1016/j.jaut.2012.05.020. Epub 2012 Jun 27. J Autoimmun. 2012. PMID: 22748431 Free PMC article. Review.
Cited by
-
Exposures to uranium and arsenic alter intraepithelial and innate immune cells in the small intestine of male and female mice.Toxicol Appl Pharmacol. 2020 Sep 15;403:115155. doi: 10.1016/j.taap.2020.115155. Epub 2020 Jul 22. Toxicol Appl Pharmacol. 2020. PMID: 32710956 Free PMC article.
-
Gut microbes as future therapeutics in treating inflammatory and infectious diseases: Lessons from recent findings.J Nutr Biochem. 2018 Nov;61:111-128. doi: 10.1016/j.jnutbio.2018.07.010. Epub 2018 Aug 16. J Nutr Biochem. 2018. PMID: 30196243 Free PMC article. Review.
-
Contrasting Autoimmune Comorbidities in Microscopic Colitis and Inflammatory Bowel Diseases.Life (Basel). 2023 Feb 27;13(3):652. doi: 10.3390/life13030652. Life (Basel). 2023. PMID: 36983808 Free PMC article.
-
Is Fecal Calprotectin an Applicable Biomarker of Gut Immune System Activation in Chronic Inflammatory Demyelinating Polyneuropathy? - A Pilot Study.Front Hum Neurosci. 2021 Nov 12;15:733070. doi: 10.3389/fnhum.2021.733070. eCollection 2021. Front Hum Neurosci. 2021. PMID: 34867240 Free PMC article.
-
Molecular Interaction Network Approach (MINA) identifies association of novel candidate disease genes.MethodsX. 2019 May 31;6:1286-1291. doi: 10.1016/j.mex.2019.05.031. eCollection 2019. MethodsX. 2019. PMID: 31198690 Free PMC article.
References
-
- Bach J-F. The effect of infections on susceptibility to autoimmune and allergic diseases. The New England Journal of Medicine. 2002;347(12):911–920. - PubMed
-
- Vojdani A. Antibodies as predictors of complex autoimmune diseases and cancer. International Journal of Immunopathology and Pharmacology. 2008;21(3):553–566. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

