Adaptive servoventilation for treatment of opioid-associated central sleep apnea
- PMID: 24932143
- PMCID: PMC4031404
- DOI: 10.5664/jcsm.3788
Adaptive servoventilation for treatment of opioid-associated central sleep apnea
Abstract
Rationale: Opioids have become part of contemporary treatment in the management of chronic pain. Although severe daytime ventilatory depression is uncommon, chronic use of opioids could be associated with severe central and obstructive sleep apnea.
Objectives: To determine the acute efficacy, and prolonged use of adaptive servoventilation (ASV) to treat central sleep apnea in patients on chronic opioids.
Methods: Twenty patients on opioid therapy referred for evaluation of obstructive sleep apnea (OSA) were found to have central sleep apnea (CSA). The first 16 patients underwent continuous positive airway pressure (CPAP) titration, which showed persistent CSA. With the notion that CSA will be eliminated with continued use of CPAP, 4 weeks later, 9 of the 16 patients underwent a second CPAP titration which proved equally ineffective. Therefore, therapy with CPAP was abandoned. All patients underwent ASV titration.
Main results: Diagnostic polysomnography showed an average apnea-hypopnea index (AHI) of 61/h and a central-apnea index (CAI) of 32/h. On CPAP 1, AHI was 34/h and CAI was 20/h. Respective indices on CPAP 2 were AHI 33/h and CAI 19/h. During titration with ASV, CAI was 0/h and the average HI was 11/h on final pressures. With a reduction in AHI, oxyhemoglobin saturation nadir increased from 83% to 90%, and arousal index decreased from 29/h of sleep to 12/h on final ASV pressures. Seventeen patients were followed for a minimum of 9 months and up to 6 years. The mean long-term adherence was 5.1 ± 2.5 hours.
Conclusions: Chronic use of opioids could be associated with severe CSA which remains resistant to CPAP therapy. ASV device is effective in the treatment of CSA and over the long run, most patients remain compliant with the device. Randomized long-term studies are necessary to determine if treatment of sleep apnea with ASV improves quality of life and the known mortality associated with opioids.
Keywords: ASV; CPAP; CSA; morphine; oxycontin.
Figures

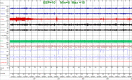

Comment in
-
The epidemic of opioid use: implications for the sleep physician.J Clin Sleep Med. 2014 Jun 15;10(6):645-6. doi: 10.5664/jcsm.3790. J Clin Sleep Med. 2014. PMID: 24932144 Free PMC article. No abstract available.
References
-
- Teichtahl H, Promdromidis A, Miller B, et al. Sleep-disordered breathing in stable methadone programme patients: a pilot program. Addiction. 2001;96:395–403. - PubMed
-
- Farney RJ, Walker JM, Cloward T, et al. Sleep-disordered breathing associated with long-term opioid therapy. Chest. 2003;123:632–9. - PubMed
-
- Wang D, Teichtahl H, Drummer O, et al. Central sleep apnea in stable methadone maintenance treatment patients. Chest. 2005;228:1348–56. - PubMed
-
- Webster L, Choi Y, Desai H, et al. Sleep disordered breathing and chronic opioid therapy. Pain Med. 2008;9:425–32. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

