Mineralocorticoid and AT1 receptors in the paraventricular nucleus contribute to sympathetic hyperactivity and cardiac dysfunction in rats post myocardial infarct
- PMID: 24951624
- PMCID: PMC4146375
- DOI: 10.1113/jphysiol.2014.276584
Mineralocorticoid and AT1 receptors in the paraventricular nucleus contribute to sympathetic hyperactivity and cardiac dysfunction in rats post myocardial infarct
Abstract
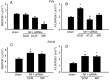
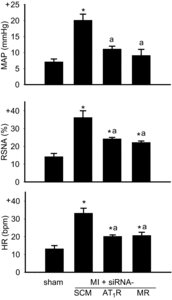
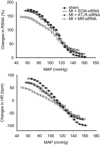
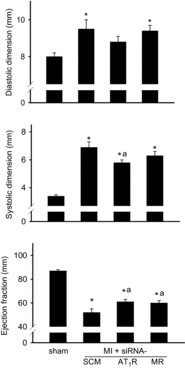
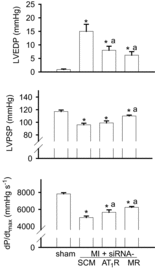
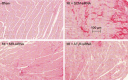
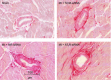
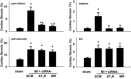
Intracerebroventricular infusion of a mineralocorticoid receptor (MR) or angiotensin II type 1 receptor (AT1R) blocker in rats attenuates sympathetic hyperactivity and progressive left ventricular (LV) dysfunction post myocardial infarction (MI). The present study examined whether knockdown of MRs or AT1Rs specifically in the paraventricular nucleus (PVN) contributes to these effects, and compared cardiac effects with those of systemic treatment with the β1-adrenergic receptor blocker metoprolol. The PVN of rats was infused with adeno-associated virus carrying small interfering RNA against either MR (AAV-MR-siRNA) or AT1R (AAV-AT1R-siRNA), or as control scrambled siRNA. At 4 weeks post MI, AT1R but not MR expression was increased in the PVN, excitatory renal sympathetic nerve activity and pressor responses to air stress were enhanced, and arterial baroreflex function was impaired; LV end-diastolic pressure (LVEDP) was increased and LV peak systolic pressure (LVPSP), ejection fraction (EF) and dP/dtmax decreased. AAV-MR-siRNA and AAV-AT1R-siRNA both normalized AT1R expression in the PVN, similarly ameliorated sympathetic and pressor responses to air stress, largely prevented baroreflex desensitization, and improved LVEDP, EF and dP/dtmax as well as cardiac interstitial (but not perivascular) fibrosis. In a second set of rats, metoprolol at 70 or 250 mg kg(-1) day(-1) in the drinking water for 4 weeks post MI did not improve LV function except for a decrease in LVEDP at the lower dose. These results suggest that in rats MR-dependent upregulation of AT1Rs in the PVN contributes to sympathetic hyperactivity, and LV dysfunction and remodelling post MI. In rats, normalizing MR-AT1R signalling in the PVN is a more effective strategy to improve LV dysfunction post MI than systemic β1 blockade.
© 2014 The Authors. The Journal of Physiology © 2014 The Physiological Society.
Figures

Similar articles
-
Knockdown of mineralocorticoid or angiotensin II type 1 receptor gene expression in the paraventricular nucleus prevents angiotensin II hypertension in rats.J Physiol. 2014 Aug 15;592(16):3523-36. doi: 10.1113/jphysiol.2014.275560. Epub 2014 Jun 27. J Physiol. 2014. PMID: 24973408 Free PMC article.
-
Sympathetic hyperactivity and cardiac dysfunction post-MI: different impact of specific CNS versus general AT1 receptor blockade.J Mol Cell Cardiol. 2007 Oct;43(4):479-86. doi: 10.1016/j.yjmcc.2007.07.047. Epub 2007 Jul 21. J Mol Cell Cardiol. 2007. PMID: 17714732
-
Chronic central versus systemic blockade of AT(1) receptors and cardiac dysfunction in rats post-myocardial infarction.Am J Physiol Heart Circ Physiol. 2009 Sep;297(3):H968-75. doi: 10.1152/ajpheart.00317.2009. Epub 2009 Jul 17. Am J Physiol Heart Circ Physiol. 2009. PMID: 19617416
-
Role of brain aldosterone and mineralocorticoid receptors in aldosterone-salt hypertension in rats.Neuroscience. 2016 Feb 9;314:90-105. doi: 10.1016/j.neuroscience.2015.11.055. Epub 2015 Nov 30. Neuroscience. 2016. PMID: 26656220
-
Mineralocorticoid receptors, inflammation and sympathetic drive in a rat model of systolic heart failure.Exp Physiol. 2010 Jan;95(1):19-25. doi: 10.1113/expphysiol.2008.045948. Epub 2009 Jul 31. Exp Physiol. 2010. PMID: 19648480 Free PMC article. Review.
Cited by
-
Adeno-associated virus-mediated gene therapy in cardiovascular disease.Curr Opin Cardiol. 2015 May;30(3):228-34. doi: 10.1097/HCO.0000000000000159. Curr Opin Cardiol. 2015. PMID: 25783685 Free PMC article. Review.
-
Is RAS the Link Between COVID-19 and Increased Stress in Head and Neck Cancer Patients?Front Cell Dev Biol. 2021 Jul 15;9:714999. doi: 10.3389/fcell.2021.714999. eCollection 2021. Front Cell Dev Biol. 2021. PMID: 34336866 Free PMC article. Review.
-
Angiotensin II Type 1a Receptors in the Subfornical Organ Modulate Neuroinflammation in the Hypothalamic Paraventricular Nucleus in Heart Failure Rats.Neuroscience. 2018 Jun 15;381:46-58. doi: 10.1016/j.neuroscience.2018.04.012. Epub 2018 Apr 21. Neuroscience. 2018. PMID: 29684507 Free PMC article.
-
Update on angiotensin II: new endocrine connections between the brain, adrenal glands and the cardiovascular system.Endocr Connect. 2017 Oct;6(7):R131-R145. doi: 10.1530/EC-17-0161. Epub 2017 Aug 30. Endocr Connect. 2017. PMID: 28855243 Free PMC article. Review.
-
Counter-regulatory renin-angiotensin system in cardiovascular disease.Nat Rev Cardiol. 2020 Feb;17(2):116-129. doi: 10.1038/s41569-019-0244-8. Epub 2019 Aug 19. Nat Rev Cardiol. 2020. PMID: 31427727 Free PMC article. Review.
References
-
- Ahmad M, White R, Tan J, Huang BS, Leenen FHH. Angiotensin-converting enzyme inhibitors, inhibition of brain and peripheral angiotensin-converting enzymes, and left ventricular dysfunction in rats after myocardial infarction. J Cardiovasc Pharmacol. 2008;51:565–572. - PubMed
-
- Bristow MR. Treatment of chronic heart failure with β-adrenergic receptor antagonists: a convergence of receptor pharmacology and clinical cardiology. Circ Res. 2011;109:1176–1194. - PubMed
-
- Chen A, Huang BS, Wang H-W, Ahmad M, Leenen FHH. Knockdown of mineralocorticoid or angiotensin II type 1 receptor gene expression in the paraventricular nucleus prevents angiotensin II hypertension in rats. J Physiol. 2014 (in press) Doi: 10.1113/jphysiol.2014.275560. - DOI - PMC - PubMed
-
- DiBona GF, Jones SY, Brooks VL. ANG II receptor blockade and arterial baroreflex regulation of renal nerve activity in cardiac failure. Am J Physiol Regul Integr Comp Physiol. 1995;269:R1189–R1196. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

