Worse patient-reported outcome after lateral approach than after anterior and posterolateral approach in primary hip arthroplasty. A cross-sectional questionnaire study of 1,476 patients 1-3 years after surgery
- PMID: 24954494
- PMCID: PMC4164862
- DOI: 10.3109/17453674.2014.934183
Worse patient-reported outcome after lateral approach than after anterior and posterolateral approach in primary hip arthroplasty. A cross-sectional questionnaire study of 1,476 patients 1-3 years after surgery
Abstract
Background: The surgical approach in total hip arthroplasty (THA) is often based on surgeon preference and local traditions. The anterior muscle-sparing approach has recently gained popularity in Europe. We tested the hypothesis that patient satisfaction, pain, function, and health-related quality of life (HRQoL) after THA is not related to the surgical approach.
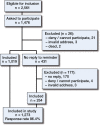
Patients: 1,476 patients identified through the Norwegian Arthroplasty Register were sent questionnaires 1-3 years after undergoing THA in the period from January 2008 to June 2010. Patient-reported outcome measures (PROMs) included the hip disability osteoarthritis outcome score (HOOS), the Western Ontario and McMaster Universities osteoarthritis index (WOMAC), health-related quality of life (EQ-5D-3L), visual analog scales (VAS) addressing pain and satisfaction, and questions about complications. 1,273 patients completed the questionnaires and were included in the analysis.
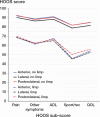
Results: Adjusted HOOS scores for pain, other symptoms, activities of daily living (ADL), sport/recreation, and quality of life were significantly worse (p < 0.001 to p = 0.03) for the lateral approach than for the anterior approach and the posterolateral approach (mean differences: 3.2-5.0). These results were related to more patient-reported limping with the lateral approach than with the anterior and posterolateral approaches (25% vs. 12% and 13%, respectively; p < 0.001).
Interpretation: Patients operated with the lateral approach reported worse outcomes 1-3 years after THA surgery. Self-reported limping occurred twice as often in patients who underwent THA with a lateral approach than in those who underwent THA with an anterior or posterolateral approach. There were no significant differences in patient-reported outcomes after THA between those who underwent THA with a posterolateral approach and those who underwent THA with an anterior approach.
Figures

References
-
- Amlie E, Hovik O, Reikeras O. Dislocation after total hip arthroplasty with 28 and 32-mm femoral head . J Orthop Traumatol. 2010;11(2):111–5. - PMC - PubMed
-
- Arthursson AJ, Furnes O, Espehaug B, Havelin LI, Soreide JA. Prosthesis survival after total hip arthroplasty—does surgical approach ... . Acta Orthop. 2007;78(6):719–29. - PubMed
-
- Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt L. Validation study of WOMAC: a health status instrument for measuring clin... . J Orthop Rheumatol. 1988;1:95–108. - PubMed
-
- Bistolfi A, Crova M, Rosso F, Titolo P, Ventura S, Massazza G. Dislocation rate after hip arthroplasty within the first postoperative y... . Hip Int. 2011;21(5):559–64. - PubMed
-
- Bystrom S, Espehaug B, Furnes O, Havelin LI. Femoral head size is a risk factor for total hip luxation: a study of 42... . Acta Orthop Scand. 2003;74(5):514–24. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
