Critical blood pressure threshold dependence of hypertensive injury and repair in a malignant nephrosclerosis model
- PMID: 24958497
- PMCID: PMC4162752
- DOI: 10.1161/HYPERTENSIONAHA.114.03609
Critical blood pressure threshold dependence of hypertensive injury and repair in a malignant nephrosclerosis model
Abstract
Most patients with essential hypertension do not exhibit substantial renal damage. Renal autoregulation by preventing glomerular transmission of systemic pressures has been postulated to mediate this resistance. Conversely, malignant nephrosclerosis (MN) has been postulated to develop when severe hypertension exceeds a critical ceiling. If the concept is valid, even modest blood pressure (BP) reductions to below this threshold regardless of antihypertensive class (1) should prevent MN and (2) lead to the healing of the already developed MN lesions. Both predicates were tested using BP radiotelemetry in the stroke-prone spontaneously hypertensive rats receiving 1% NaCl as drinking fluid for 4 weeks. Severe hypertension (final 2 weeks average systolic BP, >200 mm Hg) and MN (histological damage score 36±5; n=27) developed in the untreated stroke-prone spontaneously hypertensive rats but were prevented by all antihypertensive classes (enalapril [n=15], amlodipine [n=13], or a hydralazine/hydrochlorothiazide combination [n=15]) if the final 2-week systolic BP remained <190 mm Hg. More impressively, modest systolic BP reductions to 160 to 180 mm Hg (hydralazine/hydrochlorothiazide regimen) initiated at ≈4 weeks in additional untreated rats after MN had already developed (injury score 35±4 in the right kidney removed before therapy) led to a striking resolution of the vascular and glomerular MN injury over 2 to 3 weeks (post-therapy left kidney injury score 9±2, P<0.0001; n=27). Proteinuria also declined rapidly from 122±9.5 mg/24 hours before therapy to 20.5±3.6 mg 1 week later. These data clearly demonstrate the barotrauma-mediated pathogenesis of MN and the striking capacity for spontaneous and rapid repair of hypertensive kidney damage if new injury is prevented.
Keywords: calcium channel blockers; hypertension; renal circulation; renin-angiotensin system.
© 2014 American Heart Association, Inc.
Conflict of interest statement
None
Figures



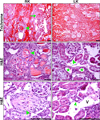

Similar articles
-
Renoprotection by ACE inhibition or aldosterone blockade is blood pressure-dependent.Hypertension. 2003 Feb;41(2):201-6. doi: 10.1161/01.hyp.0000049881.25304.73. Hypertension. 2003. PMID: 12574082
-
Impact of antihypertensive treatments on erectile responses in aging spontaneously hypertensive rats.J Hypertens. 2006 Jan;24(1):159-68. doi: 10.1097/01.hjh.0000198025.91976.8b. J Hypertens. 2006. PMID: 16331114
-
Efficacy of Antihypertensive Drugs of Different Classes After Renal Denervation in Spontaneously Hypertensive Rats.Hypertension. 2023 Jun;80(6):e90-e100. doi: 10.1161/HYPERTENSIONAHA.122.20756. Epub 2023 Mar 31. Hypertension. 2023. PMID: 36999443
-
Hypertensive renal damage: insights from animal models and clinical relevance.Curr Hypertens Rep. 2004 Apr;6(2):145-53. doi: 10.1007/s11906-004-0091-8. Curr Hypertens Rep. 2004. PMID: 15010020 Review.
-
Renal protection in hypertensive patients: selection of antihypertensive therapy.Drugs. 2005;65 Suppl 2:29-39. doi: 10.2165/00003495-200565002-00005. Drugs. 2005. PMID: 16398060 Review.
Cited by
-
From malignant hypertension to hypertension-MOD: a modern definition for an old but still dangerous emergency.J Hum Hypertens. 2016 Aug;30(8):463-6. doi: 10.1038/jhh.2015.112. Epub 2015 Nov 19. J Hum Hypertens. 2016. PMID: 26582411 Review.
-
Ischaemic stroke and pre-eclampsia in the third trimester of pregnancy: a diagnostic and therapeutic challenge.BMJ Case Rep. 2019 Dec 5;12(12):e229635. doi: 10.1136/bcr-2019-229635. BMJ Case Rep. 2019. PMID: 31811103 Free PMC article.
-
Animal Models of Hypertension: A Scientific Statement From the American Heart Association.Hypertension. 2019 Jun;73(6):e87-e120. doi: 10.1161/HYP.0000000000000090. Hypertension. 2019. PMID: 30866654 Free PMC article. Review.
-
Hemodynamic basis for the limited renal injury in rats with angiotensin II-induced hypertension.Am J Physiol Renal Physiol. 2015 Feb 1;308(3):F252-60. doi: 10.1152/ajprenal.00596.2014. Epub 2014 Dec 4. Am J Physiol Renal Physiol. 2015. PMID: 25477472 Free PMC article.
-
RNA sequencing reveals induction of specific renal inflammatory pathways in a rat model of malignant hypertension.J Mol Med (Berl). 2021 Dec;99(12):1727-1740. doi: 10.1007/s00109-021-02133-8. Epub 2021 Sep 15. J Mol Med (Berl). 2021. PMID: 34528115 Free PMC article.
References
-
- US Renal Data System. USRDS 2013 Annual Data Report. National Kidney Foundation, Inc: Published by Elsevier Inc; 2013.
-
- Bidani AK, Griffin KA. Pathophysiology of hypertensive renal damage: Implications for therapy. Hypertension. 2004;44:1–7. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

