Effect of vasopressin antagonism on renal handling of sodium and water and central and brachial blood pressure during inhibition of the nitric oxide system in healthy subjects
- PMID: 24965902
- PMCID: PMC4079642
- DOI: 10.1186/1471-2369-15-100
Effect of vasopressin antagonism on renal handling of sodium and water and central and brachial blood pressure during inhibition of the nitric oxide system in healthy subjects
Abstract
Background: Tolvaptan is a selective vasopressin receptor antagonist (V2R) that increases free water excretion. We wanted to test the hypotheses that tolvaptan changes both renal handling of water and sodium and systemic hemodynamics during basal conditions and during nitric oxide (NO)-inhibition with L-NG-monomethyl-arginine (L-NMMA).
Methods: Nineteen healthy subjects were enrolled in a randomized, placebo-controlled, double-blind, crossover study of two examination days. Tolvaptan 15 mg or placebo was given in the morning. L-NMMA was given as a bolus followed by continuous infusion during 60 minutes. We measured urine output(UO), free water clearance (CH2O), fractional excretion of sodium (FENa), urinary aquaporin-2 channels (u-AQP2) and epithelial sodium channels (u-ENaCγ), plasma vasopressin (p-AVP), central and brachial blood pressure(cBP, bBP).
Results: During baseline conditions, tolvaptan caused a significant increase in UO, CH2O and p-AVP, and FENa was unchanged. During L-NMMA infusion, UO and CH2O decreased more pronounced after tolvaptan than after placebo (-54 vs.-42% and -34 vs.-9% respectively). U-AQP2 decreased during both treatments, whereas u-ENaCγ decreased after placebo and increased after tolvaptan. CBP and bBP were unchanged.
Conclusion: During baseline conditions, tolvaptan increased renal water excretion. During NO-inhibition, the more pronounced reduction in renal water excretion after tolvaptan indicates that NO promotes water excretion in the principal cells, at least partly, via an AVP-dependent mechanism. The lack of decrease in u-AQP2 by tolvaptan could be explained by a counteracting effect of increased plasma vasopressin. The antagonizing effect of NO-inhibition on u-ENaC suggests that NO interferes with the transport via ENaC by an AVP-dependent mechanism.
Figures


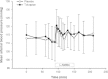
References
-
- Nielsen S, Kwon TH, Christensen BM, Promeneur D, Frokiaer J, Marples D. Physiology and pathophysiology of renal aquaporins. J Am Soc Nephrol. 1999;10(3):647–663. - PubMed
-
- Verbalis JG, Goldsmith SR, Greenberg A, Schrier RW, Sterns RH. Hyponatremia treatment guidelines 2007: expert panel recommendations. Am J Med. 2007;120(11 Suppl 1):S1–21. - PubMed
-
- Loffing J, Korbmacher C. Regulated sodium transport in the renal connecting tubule (CNT) via the epithelial sodium channel (ENaC) Pflugers Arch. 2009;458(1):111–135. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

