Recurrent Clostridium difficile infections: the importance of the intestinal microbiota
- PMID: 24966611
- PMCID: PMC4064086
- DOI: 10.3748/wjg.v20.i23.7416
Recurrent Clostridium difficile infections: the importance of the intestinal microbiota
Abstract
Clostridium difficile infections (CDI) are a leading cause of antibiotic-associated and nosocomial diarrhea. Despite effective antibiotic treatments, recurrent infections are common. With the recent emergence of hypervirulent isolates of C. difficile, CDI is a growing epidemic with higher rates of recurrence, increasing severity and mortality. Fecal microbiota transplantation (FMT) is an alternative treatment for recurrent CDI. A better understanding of intestinal microbiota and its role in CDI has opened the door to this promising therapeutic approach. FMT is thought to resolve dysbiosis by restoring gut microbiota diversity thereby breaking the cycle of recurrent CDI. Since the first reported use of FMT for recurrent CDI in 1958, systematic reviews of case series and case report have shown its effectiveness with high resolution rates compared to standard antibiotic treatment. This article focuses on current guidelines for CDI treatment, the role of intestinal microbiota in CDI recurrence and current evidence about FMT efficacy, adverse effects and acceptability.
Keywords: Clostridium difficile infection; Clostridium difficile recurrence; Fecal microbiota transplantation; Microbiota; Stool transplantation.
Figures

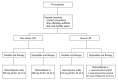


References
-
- Cohen SH, Gerding DN, Johnson S, Kelly CP, Loo VG, McDonald LC, Pepin J, Wilcox MH. Clinical practice guidelines for Clostridium difficile infection in adults: 2010 update by the society for healthcare epidemiology of America (SHEA) and the infectious diseases society of America (IDSA) Infect Control Hosp Epidemiol. 2010;31:431–455. - PubMed
-
- Jones AM, Kuijper EJ, Wilcox MH. Clostridium difficile: a European perspective. J Infect. 2013;66:115–128. - PubMed
-
- Miller BA, Chen LF, Sexton DJ, Anderson DJ. Comparison of the burdens of hospital-onset, healthcare facility-associated Clostridium difficile Infection and of healthcare-associated infection due to methicillin-resistant Staphylococcus aureus in community hospitals. Infect Control Hosp Epidemiol. 2011;32:387–390. - PubMed
-
- Kelly CP, LaMont JT. Clostridium difficile--more difficult than ever. N Engl J Med. 2008;359:1932–1940. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

