Importance of dynamic aortic evaluation in planning TEVAR
- PMID: 24967170
- PMCID: PMC4052412
- DOI: 10.3978/j.issn.2225-319X.2014.04.05
Importance of dynamic aortic evaluation in planning TEVAR
Abstract
Dynamic aortic evaluation in planning thoracic endovascular aortic repair (TEVAR) is important to provide optimal stent graft sizing. Static imaging protocols do not consider normal aortic dynamics and may lead to stent graft to aorta mismatch, causing stent graft related complications, such as type I endoleak and stent graft migration. Dynamic imaging can assist in accurate stent graft selection and sizing preoperatively, and evaluate stent graft performance during follow-up. To create new imaging technologies, integration of knowledge between diverse scientific fields is essential (i.e., engineering, informatics and medicine). Different dynamic imaging modalities, such as electrocardiographic-gated computed tomography angiography (ECG-gated CTA) and four-dimensional phase-contrast MRI (4D PC-MRI), are progressively investigated and implemented into clinical practice as important instruments in preoperative planning for TEVAR. In time, further application of dynamic imaging tools for preoperative screening and follow-up after TEVAR might lead to better outcomes for patients. The advances in dynamic imaging for evaluation of the thoracic aorta using new imaging modalities and their future perspectives are addressed in this manuscript.
Keywords: Dynamic imaging; computational fluid dynamics (CFD); thoracic aortic disease; thoracic endovascular aortic repair (TEVAR); type B aortic dissection.
Figures
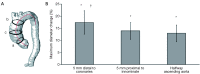
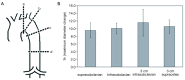
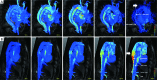
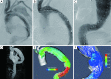
References
-
- van Keulen JW, van Prehn J, Prokop M, et al. Dynamics of the aorta before and after endovascular aneurysm repair: a systematic review. Eur J Vasc Endovasc Surg 2009;38:586-96 - PubMed
-
- Laskowski I, Verhagen HJ, Gagne PJ, et al. Current state of dynamic imaging in endovascular aortic aneurysm repair. J Endovasc Ther 2007;14:807-12 - PubMed
-
- van Herwaarden JA, Bartels LW, Muhs BE, et al. Dynamic magnetic resonance angiography of the aneurysm neck: conformational changes during the cardiac cycle with possible consequences for endograft sizing and future design. J Vasc Surg 2006;44:22-8 - PubMed
-
- van Prehn J, Schlösser FJ, Muhs BE, et al. Oversizing of aortic stent grafts for abdominal aneurysm repair: a systematic review of the benefits and risks. Eur J Vasc Endovasc Surg 2009;38:42-53 - PubMed
-
- Muhs BE, Vincken KL, van Prehn J, et al. Dynamic cine-CT angiography for the evaluation of the thoracic aorta; insight in dynamic changes with implications for thoracic endograft treatment. Eur J Vasc Endovasc Surg 2006;32:532-6 - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
