Risk factors and indications for readmission after lower extremity amputation in the American College of Surgeons National Surgical Quality Improvement Program
- PMID: 24985536
- PMCID: PMC4254086
- DOI: 10.1016/j.jvs.2014.05.050
Risk factors and indications for readmission after lower extremity amputation in the American College of Surgeons National Surgical Quality Improvement Program
Abstract
Background: Postoperative readmission, recently identified as a marker of hospital quality in the Affordable Care Act, is associated with increased morbidity, mortality, and health care costs, yet data on readmission after lower extremity amputation (LEA) are limited. We evaluated risk factors for readmission and postdischarge adverse events after LEA in the American College of Surgeons National Surgical Quality Improvement Program (NSQIP).
Methods: All patients undergoing transmetatarsal (TMA), below-knee (BKA), or above-knee amputation (AKA) in the 2011-2012 NSQIP were identified. Independent predischarge predictors of 30-day readmission were determined by multivariable logistic regression. Readmission indication and reinterventions, available in the 2012 NSQIP only, were also evaluated.
Results: We identified 5732 patients undergoing amputation (TMA, 12%; BKA, 51%; AKA, 37%). Readmission rate was 18%. Postdischarge mortality rate was 5% (TMA, 2%; BKA, 3%; AKA, 8%; P < .001). Overall complication rate was 43% (in-hospital, 32%; postdischarge, 11%). Reoperation was for wound-related complication or additional amputation in 79% of cases. Independent predictors of readmission included chronic nursing home residence (odds ratio [OR], 1.3; 95% confidence interval [CI], 1.0-1.7), nonelective surgery (OR, 1.4; 95% CI, 1.1-1.7), prior revascularization/amputation (OR, 1.4; 95% CI, 1.1-1.7), preoperative congestive heart failure (OR, 1.7; 95% CI, 1.2-2.4), and preoperative dialysis (OR, 1.5; 95% CI, 1.2-1.9). Guillotine amputation (OR, 0.6; 95% CI, 0.4-0.9) and non-home discharge (OR, 0.7; 95% CI, 0.6-1.0) were protective of readmission. Wound-related complications accounted for 49% of readmissions.
Conclusions: Postdischarge morbidity, mortality, and readmission are common after LEA. Closer follow-up of high-risk patients, optimization of medical comorbidities, and aggressive management of wound infection may play a role in decreasing readmission and postdischarge adverse events.
Copyright © 2014 Society for Vascular Surgery. Published by Elsevier Inc. All rights reserved.
Figures
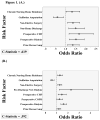

References
-
- Medicare Payment Advisory Commission (U.S.) Report to the Congress: promoting greater efficiency in Medicare. Washington, DC: Med PAC; 2007.
-
- United States., United States. Congress. House. Office of the Legislative Counsel, United States. Congress. House. Committee on Ways and Means., United States. Congress. House. Committee on Energy and Commerce., United States. Congress. House. Committee on Education and Labor. Compilation of Patient Protection and Affordable Care Act: as amended through November 1, 2010 including Patient Protection and Affordable Care Act health-related portions of the Health Care and Education Reconciliation Act of 2010. Washington: U.S. Government Printing Office; 2010.
-
- Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360:1418–28. - PubMed
-
- Vogel TR, Kruse RL. Risk factors for readmission after lower extremity procedures for peripheral artery disease. J Vasc Surg. 2013;58:90–7. e1–4. - PubMed
-
- McPhee JT, Barshes NR, Ho KJ, Madenci A, Ozaki CK, Nguyen LL, et al. Predictive factors of 30-day unplanned readmission after lower extremity bypass. J Vasc Surg. 2013;57:955–62. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

