Numerical simulation of callus healing for optimization of fracture fixation stiffness
- PMID: 24991809
- PMCID: PMC4081589
- DOI: 10.1371/journal.pone.0101370
Numerical simulation of callus healing for optimization of fracture fixation stiffness
Abstract
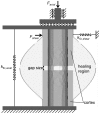
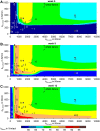
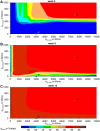
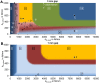
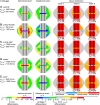
The stiffness of fracture fixation devices together with musculoskeletal loading defines the mechanical environment within a long bone fracture, and can be quantified by the interfragmentary movement. In vivo results suggested that this can have acceleratory or inhibitory influences, depending on direction and magnitude of motion, indicating that some complications in fracture treatment could be avoided by optimizing the fixation stiffness. However, general statements are difficult to make due to the limited number of experimental findings. The aim of this study was therefore to numerically investigate healing outcomes under various combinations of shear and axial fixation stiffness, and to detect the optimal configuration. A calibrated and established numerical model was used to predict fracture healing for numerous combinations of axial and shear fixation stiffness under physiological, superimposed, axial compressive and translational shear loading in sheep. Characteristic maps of healing outcome versus fixation stiffness (axial and shear) were created. The results suggest that delayed healing of 3 mm transversal fracture gaps will occur for highly flexible or very rigid axial fixation, which was corroborated by in vivo findings. The optimal fixation stiffness for ovine long bone fractures was predicted to be 1000-2500 N/mm in the axial and >300 N/mm in the shear direction. In summary, an optimized, moderate axial stiffness together with certain shear stiffness enhances fracture healing processes. The negative influence of one improper stiffness can be compensated by adjustment of the stiffness in the other direction.
Conflict of interest statement
Figures

Similar articles
-
Disadvantages of interfragmentary shear on fracture healing--mechanical insights through numerical simulation.J Orthop Res. 2014 Jul;32(7):865-72. doi: 10.1002/jor.22617. Epub 2014 Mar 20. J Orthop Res. 2014. PMID: 24648331
-
Prediction of the time course of callus stiffness as a function of mechanical parameters in experimental rat fracture healing studies--a numerical study.PLoS One. 2014 Dec 22;9(12):e115695. doi: 10.1371/journal.pone.0115695. eCollection 2014. PLoS One. 2014. PMID: 25532060 Free PMC article.
-
Shear movement at the fracture site delays healing in a diaphyseal fracture model.J Orthop Res. 2003 Nov;21(6):1011-7. doi: 10.1016/S0736-0266(03)00098-6. J Orthop Res. 2003. PMID: 14554213
-
[Mechanical modification of callus healing].Chirurg. 2000 Sep;71(9):989-94. doi: 10.1007/s001040051172. Chirurg. 2000. PMID: 11043114 Review. German.
-
Effect of mechanical stability on fracture healing--an update.Injury. 2007 Mar;38 Suppl 1:S3-10. doi: 10.1016/j.injury.2007.02.005. Injury. 2007. PMID: 17383483 Review.
Cited by
-
Weak Points of Double-Plate Stabilization Used in the Treatment of Distal Humerus Fracture through Finite Element Analysis.J Clin Med. 2024 Feb 11;13(4):1034. doi: 10.3390/jcm13041034. J Clin Med. 2024. PMID: 38398347 Free PMC article.
-
Minimally Invasive Internal Fixation of Femoral Shaft Fractures-A Biomechanical Study with a Disruptive Technique.Life (Basel). 2021 Nov 17;11(11):1254. doi: 10.3390/life11111254. Life (Basel). 2021. PMID: 34833130 Free PMC article.
-
Comparison between Novel Anatomical Locking Guide Plate and Conventional Locking Plate for Acetabular Fractures: A Finite Element Analysis.Life (Basel). 2023 Oct 24;13(11):2108. doi: 10.3390/life13112108. Life (Basel). 2023. PMID: 38004248 Free PMC article.
-
Methods to accelerate fracture healing - a narrative review from a clinical perspective.Front Immunol. 2024 Jun 7;15:1384783. doi: 10.3389/fimmu.2024.1384783. eCollection 2024. Front Immunol. 2024. PMID: 38911851 Free PMC article. Review.
-
[Mechanobiology of fracture healing part 2 : Relevance for internal fixation of fractures].Unfallchirurg. 2017 Jan;120(1):23-31. doi: 10.1007/s00113-016-0281-2. Unfallchirurg. 2017. PMID: 27975121 German.
References
-
- Bhandari M, Tornetta P, Sprague S, Najibi S, Petrisor T, et al. (2003) Predictors of reoperation following operative management of fractures of the tibial shaft. Journal of Orthopaedic Trauma 17: 353–361. - PubMed
-
- Einhorn TA (1995) Enhancement of fracture healing. Journal of Bone and Joint Surgery-American Volume 77A: 940–956. - PubMed
-
- Karladani AH, Granhed H, Karrholm J, Styf J (2001) The influence of fracture etiology and type on fracture healing: a review of 104 consecutive tibial shaft fractures. Archives of Orthopaedic and Trauma Surgery 121: 325–328. - PubMed
-
- Brinker MR, O’Connor DP (2004) The incidence of fractures and dislocations referred for orthopaedic services in a capitated population. Journal of Bone and Joint Surgery-American Volume 86A: 290–297. - PubMed
-
- Praemer A, Furner S, Rice DP (1992) Musculoskeletal conditions in the United States. Rosemont, IL: American Academy of Orthopaedic Surgeons Park Ridge.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

