Interventions to increase influenza vaccination rates of those 60 years and older in the community
- PMID: 24999919
- PMCID: PMC6464876
- DOI: 10.1002/14651858.CD005188.pub3
Interventions to increase influenza vaccination rates of those 60 years and older in the community
Update in
-
Interventions to increase influenza vaccination rates of those 60 years and older in the community.Cochrane Database Syst Rev. 2018 May 30;5(5):CD005188. doi: 10.1002/14651858.CD005188.pub4. Cochrane Database Syst Rev. 2018. PMID: 29845606 Free PMC article.
Abstract
Background: The effectiveness of interventions to increase the uptake of influenza vaccination in people aged 60 and older is uncertain.
Objectives: To assess access, provider, system and societal interventions to increase the uptake of influenza vaccination in people aged 60 years and older in the community.
Search methods: We searched CENTRAL (2014, Issue 5), MEDLINE (January 1950 to May week 3 2014), EMBASE (1980 to June 2014), AgeLine (1978 to 4 June 2014), ERIC (1965 to June 2014) and CINAHL (1982 to June 2014).
Selection criteria: Randomised controlled trials (RCTs) of interventions to increase influenza vaccination uptake in people aged 60 and older.
Data collection and analysis: Two review authors independently assessed study quality and extracted influenza vaccine uptake data.
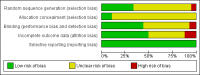
Main results: This update identified 13 new RCTs; the review now includes a total of 57 RCTs with 896,531 participants. The trials included community-dwelling seniors in high-income countries. Heterogeneity limited meta-analysis. The percentage of trials with low risk of bias for each domain was as follows: randomisation (33%); allocation concealment (11%); blinding (44%); missing data (49%) and selective reporting (100%). Increasing community demand (32 trials, 10 strategies)The interventions with a statistically significant result were: three trials (n = 64,200) of letter plus leaflet/postcard compared to letter (odds ratio (OR) 1.11, 95% confidence interval (CI) 1.07 to 1.15); two trials (n = 614) of nurses/pharmacists educating plus vaccinating patients (OR 3.29, 95% CI 1.91 to 5.66); single trials of a phone call from a senior (n = 193) (OR 3.33, 95% CI 1.79 to 6.22), a telephone invitation versus clinic drop-in (n = 243) (OR 2.72, 95% CI 1.55 to 4.76), a free groceries lottery (n = 291) (OR 1.04, 95% CI 0.62 to 1.76) and nurses educating and vaccinating patients (n = 485) (OR 152.95, 95% CI 9.39 to 2490.67).We did not pool the following trials due to considerable heterogeneity: postcard/letter/pamphlets (16 trials, n = 592,165); tailored communications (16 trials, n = 388,164); customised letter/phone-call (four trials, n = 82,465) and client-based appraisals (three trials, n = 4016), although several trials showed the interventions were effective. Enhancing vaccination access (10 trials, six strategies)The interventions with a statistically significant result were: two trials (n = 2112) of home visits compared to clinic invitation (OR 1.30, 95% CI 1.05 to 1.61); two trials (n = 2251) of free vaccine (OR 2.36, 95% CI 1.98 to 2.82) and one trial (n = 321) of patient group visits (OR 24.85, 95% CI 1.45 to 425.32). One trial (n = 350) of a home visit plus vaccine encouragement compared to a home visit plus safety advice was non-significant.We did not pool the following trials due to considerable heterogeneity: nurse home visits (two trials, n = 2069) and free vaccine compared to no intervention (two trials, n = 2250). Provider- or system-based interventions (17 trials, 11 strategies)The interventions with a statistically significant result were: two trials (n = 2815) of paying physicians (OR 2.22, 95% CI 1.77 to 2.77); one trial (n = 316) of reminding physicians about all their patients (OR 2.47, 95% CI 1.53 to 3.99); one trial (n = 8376) of posters plus postcards (OR 2.03, 95% CI 1.86 to 2.22); one trial (n = 1360) of chart review/feedback (OR 3.43, 95% CI 2.37 to 4.97) and one trial (n = 27,580) of educational outreach/feedback (OR 0.77, 95% CI 0.72 to 0.81).Trials of posters plus postcards versus posters (n = 5753), academic detailing (n = 1400) and increasing staff vaccination rates (n = 26,432) were non-significant.We did not pool the following trials due to considerable heterogeneity: reminding physicians (four trials, n = 202,264) and practice facilitators (three trials, n = 2183), although several trials showed the interventions were effective. Interventions at the societal level We identified no RCTs of interventions at the societal level.
Authors' conclusions: There are interventions that are effective for increasing community demand for vaccination, enhancing access and improving provider/system response. Heterogeneity limited pooling of trials.
Conflict of interest statement
Roger E Thomas: none known. Diane L Lorenzetti: none known.
Figures






























Update of
-
Interventions to increase influenza vaccination rates of those 60 years and older in the community.Cochrane Database Syst Rev. 2010 Sep 8;(9):CD005188. doi: 10.1002/14651858.CD005188.pub2. Cochrane Database Syst Rev. 2010. Update in: Cochrane Database Syst Rev. 2014 Jul 07;(7):CD005188. doi: 10.1002/14651858.CD005188.pub3. PMID: 20824843 Updated.
Comment in
-
Cochrane review summary: Interventions to increase influenza vaccination rates of those 60 years and older in the community.Prim Health Care Res Dev. 2015 May;16(3):221-3. doi: 10.1017/S1463423615000110. Epub 2015 Apr 8. Prim Health Care Res Dev. 2015. PMID: 25853928 No abstract available.
References
References to studies included in this review
-
- Abramson ZH, Avni O, Levi O, Miskin IN. Is the influenza vaccination rate of elderly patients affected by raising the vaccination rate of the staff at their primary health care clinics?. Israel Medical Association Journal 2011;13:325‐8. - PubMed
- Abramson ZH, Avni O, Levi O, Miskin IN. Randomized trial of a program to increase staff influenza vaccination in primary care clinics. Annals of Family Medicine 2010;8:293‐8. [DOI: 10.1370/afm.1132] - DOI - PMC - PubMed
-
- Barnas GP, McKinney WP. Postcard reminders and influenza vaccination. Journal of the American Geriatrics Society 1989;37(2):195. - PubMed
-
- Beck A, Scott J, Williams P, Robertson B, Jackson D, Gade G, et al. A randomized controlled trial of group outpatient visits for chronically ill older HMO members: The Cooperative Health Care Clinic. Journal of the American Geriatrics Society 1997;45:543‐9. - PubMed
References to studies excluded from this review
-
- Ahmed F, Friedman C, Franks A, Latts LM, Nugent EW, France EK, et al. Effect of the frequency of delivery of reminders and an influenza tool kit on increasing influenza vaccination rates among adults with high‐risk conditions. American Journal of Managed Care 2004;10:698‐702. - PubMed
-
- Alemi F, Alemagno SA, Goldhagen J, Ash L, Finkelstein B, Lavin A, et al. Computer reminders improve on‐time immunization rates. Medical Care 1996;34(Suppl 10):45‐51. - PubMed
-
- Alexy BB, Elnitsky C. Rural mobile health unit: outcomes. Public Health Nursing 1998;15(1):3‐11. - PubMed
-
- Allsup S, Haycox A, Regan M, Gosney M. Is influenza vaccination cost effective for healthy people between ages 65 and 74 years? A randomised controlled trial. Vaccine 2004;23:639‐45. - PubMed
-
- Anderson C, Martin H. Effectiveness of patient recall system on immunization rates for influenza. Journal of Family Practice 1979;9(4):727‐30. - PubMed
References to studies awaiting assessment
-
- Lee SS. Is the use of physician reminder sticker on medical records effective for improving the rate of recommending influenza vaccination?. Korean Academy of Family Medicine 2003;24(8):715‐20.
-
- Song Y, Oh J, Han S, Choi C. Effectiveness of telephone and postcard reminders for the influenza vaccination: a study in the elderly who have visited a family practice center in a tertiary care hospital. Korean Journal of Preventive Medicine 2000;33(1):109‐16.
Additional references
-
- Ashby‐Hughes B, Nickerson N. Provider endorsement: the strongest cue in prompting high‐risk adults to receive influenza and pneumococcal immunizations. Clinical Excellence for Nurse Practitioners 1999;3(2):97‐104. - PubMed
-
- Ballada D, Biasio LR, Cascio G, D'Alessandro D, Donatelli I, Fara GM, et al. Attitudes and behavior of health care personnel regarding influenza vaccination. European Journal of Epidemiology 1994;10:63‐8. - PubMed
-
- Blank PR, Schwenkglenks M, Szucs TD. Disparities in influenza vaccination coverage rates by target group in five European countries: trends over seven consecutive seasons. Infection 2009;37(5):390‐400. - PubMed
-
- Bordley WC, Chelminski A, Margolis PA, Kraus R, Szilagyi PG, Vann JJ. The effect of audit and feedback on immunization delivery: a systematic review. American Journal of Preventive Medicine 2000;18(4):343‐50. - PubMed
-
- Briss PA, Rodewald LE, Hinman AR, Shefer AM, Strikas RA, Bernie RR, et al. Reviews of evidence regarding interventions to improve vaccination coverage in children, adolescents, and adults. American Journal of Preventive Medicine 2000;18(Suppl 1):97‐140. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

