Caudal mucogingival lesions secondary to traumatic dental occlusion in 27 cats: macroscopic and microscopic description, treatment and follow-up
- PMID: 25001492
- PMCID: PMC11104163
- DOI: 10.1177/1098612X14541264
Caudal mucogingival lesions secondary to traumatic dental occlusion in 27 cats: macroscopic and microscopic description, treatment and follow-up
Abstract
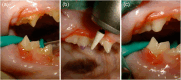
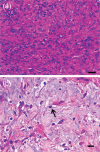
The main aim of this retrospective study was to describe clinical and histopathological findings in cats with mucogingival lesions developed at the contact point of the premolar and molar teeth of the opposite quadrant. Cases were retrieved following manual review of the medical records, dental records and photographic documentation of all feline dental patients visited in the period between February 2001 and August 2011. Cats showing different lesions at different times were calculated as multiple cases. A total of 27 cats (31 cases) with 44 lesions (26 proliferations [59%], 11 clefts [25%] and seven foveae [16%]) were included. Mean age at the time of the first visit was 6.6 years. The lesion object of the study was the main reason for presentation in only five cases (16%). Proliferations showed two different histopathological patterns and had characteristics in common with human oral pyogenic granuloma. Successful treatment was achieved in all cases by removing the occlusal contact by dental extraction or coronal reduction, possibly associated with lesion excision. This study underlines the need for a thorough oral examination and evaluation of dental occlusion in all patients. Causes for the development of traumatic occlusion may include an acquired overbite (possibly secondary to selective dental extraction), congenital or post-traumatic malocclusion, abnormal latero-lateral mobility of the mandible, occlusal drift of the premolar and molar teeth, and/or alveolar bone expansion.
© ISFM and AAFP 2014.
Conflict of interest statement
The authors do not have any potential conflicts of interest to declare.
Figures





Similar articles
-
Clinicopathologic characterization of oral pyogenic granuloma in 8 cats.J Vet Dent. 2014 Summer;31(2):80-6. doi: 10.1177/089875641403100203. J Vet Dent. 2014. PMID: 25185331
-
Clinical Characterisation of Caudal Traumatic Malocclusions and Treatment Outcomes in Cats (2018-2022).J Vet Dent. 2024 Mar;41(2):114-121. doi: 10.1177/08987564231181055. Epub 2023 Jun 13. J Vet Dent. 2024. PMID: 37312535
-
Scanning electron microscopic description of cellular activity and mineral changes in feline odontoclastic resorptive lesions.J Vet Dent. 2001 Dec;18(4):171-6. J Vet Dent. 2001. PMID: 11968898
-
Radiographic evaluation and treatment of feline dental resorptive lesions.Vet Clin North Am Small Anim Pract. 2005 Jul;35(4):943-62, vii-viii. doi: 10.1016/j.cvsm.2005.03.008. Vet Clin North Am Small Anim Pract. 2005. PMID: 15979520 Review.
-
Tooth resorption in cats: pathophysiology and treatment options.J Feline Med Surg. 2015 Jan;17(1):37-43. doi: 10.1177/1098612X14560098. J Feline Med Surg. 2015. PMID: 25527492 Free PMC article. Review.
Cited by
-
Feline minor salivary gland adenocarcinoma: retrospective case series and literature review.J Feline Med Surg. 2023 Aug;25(8):1098612X231189973. doi: 10.1177/1098612X231189973. J Feline Med Surg. 2023. PMID: 37606891 Free PMC article. Review.
-
Malocclusion in cats associated with mandibular soft tissue trauma: a retrospective case-control study.J Feline Med Surg. 2023 Oct;25(10):1098612X231202322. doi: 10.1177/1098612X231202322. J Feline Med Surg. 2023. PMID: 37906203 Free PMC article.
-
Transoral approach for mandibular and sublingual sialoadenectomy in a cat.Can Vet J. 2021 May;62(5):497-500. Can Vet J. 2021. PMID: 33967289 Free PMC article.
References
-
- Awange DO, Wakoli KA, Onyango JF, et al.. Reactive localised inflammatory hyperplasia of the oral mucosa. East Afr Med J 2009; 86: 79–82. - PubMed
-
- Baricevic M, Mravak-Stipetic M, Majstorovic M, et al.. Oral mucosal lesions during orthodontic treatment. Int J Paediatr Dent 2011; 21: 96–102. - PubMed
-
- Bellows J. Oral pathology. In: Bellows J. (ed). Feline dentistry: oral assessment, treatment, and preventative care. Ames, IA: Wiley-Blackwell, 2010, pp 101–148.
-
- Bellows J. Treatment of periodontal disease. In: Bellows J. (ed). Feline dentistry: oral assessment, treatment, and preventative care. Ames, IA: Wiley-Blackwell, 2010, pp 181–195.
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

