Role of cellular immunity in cow's milk allergy: pathogenesis, tolerance induction, and beyond
- PMID: 25002754
- PMCID: PMC4070503
- DOI: 10.1155/2014/249784
Role of cellular immunity in cow's milk allergy: pathogenesis, tolerance induction, and beyond
Abstract
Food allergy is an aberrant immune-mediated reaction against harmless food substances, such as cow's milk proteins. Due to its very early introduction, cow's milk allergy is one of the earliest and most common food allergies. For this reason cow's milk allergy can be recognized as one of the first indications of an aberrant inflammatory response in early life. Classically, cow's milk allergy, as is true for most other allergies as well, is primarily associated with abnormal humoral immune responses, that is, elevation of specific immunoglobulin E levels. There is growing evidence indicating that cellular components of both innate and adaptive immunity play significant roles during the pathogenesis of cow's milk allergy. This is true for the initiation of the allergic phenotype (stimulation and skewing towards sensitization), development and outgrowth of the allergic disease. This review discusses findings pertaining to roles of cellular immunity in allergic inflammation, and tolerance induction against cow's milk proteins. In addition, a possible interaction between immune mechanisms underlying cow's milk allergy and other types of inflammation (infections and noncommunicable diseases) is discussed.
Figures
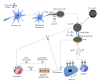
Similar articles
-
Goat Milk Allergy and a Potential Role for Goat Milk in Cow's Milk Allergy.Nutrients. 2024 Jul 24;16(15):2402. doi: 10.3390/nu16152402. Nutrients. 2024. PMID: 39125282 Free PMC article. Review.
-
[The role of specific IgE to evolution and prognosis of cow's milk protein allergies in children].Rev Med Chir Soc Med Nat Iasi. 2011 Oct-Dec;115(4):1012-7. Rev Med Chir Soc Med Nat Iasi. 2011. PMID: 22276438 Romanian.
-
Natural history of immunoglobulin E-mediated cow's milk allergy in a population of Argentine children.Arch Argent Pediatr. 2017 Aug 1;115(4):331-335. doi: 10.5546/aap.2017.eng.331. Arch Argent Pediatr. 2017. PMID: 28737860 English, Spanish.
-
Prevention of Allergy to a Major Cow's Milk Allergen by Breastfeeding in Mice Depends on Maternal Immune Status and Oral Exposure During Lactation.Front Immunol. 2020 Jul 21;11:1545. doi: 10.3389/fimmu.2020.01545. eCollection 2020. Front Immunol. 2020. PMID: 32849523 Free PMC article.
-
The natural history of cow's milk protein allergy/intolerance.Eur J Clin Nutr. 1995 Sep;49 Suppl 1:S13-8. Eur J Clin Nutr. 1995. PMID: 8647059 Review.
Cited by
-
Investigation of the effects of bovine collagen peptides and mixed berries on rheological properties and biological activity of egg white-based beverage via central composite design.Front Nutr. 2023 Feb 9;9:1011553. doi: 10.3389/fnut.2022.1011553. eCollection 2022. Front Nutr. 2023. PMID: 36846024 Free PMC article.
-
A specific synbiotic-containing amino acid-based formula in dietary management of cow's milk allergy: a randomized controlled trial.Clin Transl Allergy. 2019 Jan 15;9:5. doi: 10.1186/s13601-019-0241-3. eCollection 2019. Clin Transl Allergy. 2019. PMID: 30651972 Free PMC article.
-
Lactose Intolerance versus Cow's Milk Allergy in Infants: A Clinical Dilemma.Nutrients. 2024 Jan 31;16(3):414. doi: 10.3390/nu16030414. Nutrients. 2024. PMID: 38337698 Free PMC article. Review.
-
Neuroimmune circuits involved in β-lactoglobulin-induced food allergy.Brain Behav Immun Health. 2022 May 21;23:100471. doi: 10.1016/j.bbih.2022.100471. eCollection 2022 Aug. Brain Behav Immun Health. 2022. PMID: 35668724 Free PMC article.
-
Assessment of Inflammatory Markers in Children with Cow's Milk Allergy Treated with a Milk-Free Diet.Nutrients. 2021 Mar 24;13(4):1057. doi: 10.3390/nu13041057. Nutrients. 2021. PMID: 33805091 Free PMC article.
References
-
- Fiocchi A, Schünemann HJ, Brozek J, et al. Diagnosis and rationale for action against cow’s milk allergy (DRACMA): a summary report. Journal of Allergy and Clinical Immunology. 2010;126(6):1119.e1–1128.e1. - PubMed
-
- Koletzko S, Niggemann B, Arato A, et al. Diagnostic approach and management of cow’s-milk protein allergy in infants and children: Espghan gi committee practical guidelines. Journal of Pediatric Gastroenterology and Nutrition. 2012;55(2):221–229. - PubMed
-
- Sprikkelman AB, Heymans HSA, van Aalderen MMC. Development of allergic disorders in children with cow’s milk protein allergy or intolerance in infancy. Clinical and Experimental Allergy. 2000;30(10):1358–1363. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

