Comparative associations of muscle mass and muscle strength with mortality in dialysis patients
- PMID: 25074839
- PMCID: PMC4186520
- DOI: 10.2215/CJN.10261013
Comparative associations of muscle mass and muscle strength with mortality in dialysis patients
Abstract
Background and objectives: Reduced muscle mass and strength are prevalent conditions in dialysis patients. However, muscle strength and muscle mass are not congruent; muscle strength can diminish even though muscle mass is maintained or increased. This study addresses phenotype and mortality associations of these muscle dysfunction entities alone or in combination (i.e., concurrent loss of muscle mass and strength/mobility, here defined as sarcopenia).
Design, setting, participants, & measurements: This study included 330 incident dialysis patients (203 men, mean age 53±13 years, and mean GFR 7±2 ml/min per 1.73 m(2)) recruited between 1994 and 2010 and followed prospectively for up to 5 years. Low muscle mass (by dual-energy x-ray absorptiometry appendicular mass index) and low muscle strength (by handgrip) were defined against young reference populations according to the European Working Group on Sarcopenia in Older People.
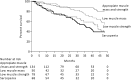
Results: Whereas 20% of patients had sarcopenia, low muscle mass and low muscle strength alone were observed in a further 24% and 15% of patients, respectively. Old age, comorbidities, protein-energy wasting, physical inactivity, low albumin, and inflammation associated with low muscle strength, but not with low muscle mass (multivariate ANOVA interactions). During follow-up, 95 patients (29%) died and both conditions associated with mortality as separate entities. When combined, individuals with low muscle mass alone were not at increased risk of mortality (adjusted hazard ratio [HR], 1.23; 95% confidence interval [95% CI], 0.56 to 2.67). Individuals with low muscle strength were at increased risk, irrespective of their muscle stores being appropriate (HR, 1.98; 95% CI, 1.01 to 3.87) or low (HR, 1.93; 95% CI, 1.01 to 3.71).
Conclusions: Low muscle strength was more strongly associated with aging, protein-energy wasting, physical inactivity, inflammation, and mortality than low muscle mass. Assessment of muscle functionality may provide additional diagnostic and prognostic information to muscle-mass evaluation.
Keywords: CKD; ESRD; malnutrition; mortality risk; nutrition.
Copyright © 2014 by the American Society of Nephrology.
Figures

References
-
- US Renal Data System : USRDS 2012 Annual Data Report: Atlas of Chronic Kidney Disease and End-Stage Renal Disease in the United States, Bethesda, MD, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, 2012
-
- Carrero JJ, Chmielewski M, Axelsson J, Snaedal S, Heimbürger O, Bárány P, Suliman ME, Lindholm B, Stenvinkel P, Qureshi AR: Muscle atrophy, inflammation and clinical outcome in incident and prevalent dialysis patients. Clin Nutr 27: 557–564, 2008 - PubMed
-
- Heimbürger O, Qureshi AR, Blaner WS, Berglund L, Stenvinkel P: Hand-grip muscle strength, lean body mass, and plasma proteins as markers of nutritional status in patients with chronic renal failure close to start of dialysis therapy. Am J Kidney Dis 36: 1213–1225, 2000 - PubMed
-
- Carrero JJ, Stenvinkel P, Cuppari L, Ikizler TA, Kalantar-Zadeh K, Kaysen G, Mitch WE, Price SR, Wanner C, Wang AY, ter Wee P, Franch HA: Etiology of the protein-energy wasting syndrome in chronic kidney disease: A consensus statement from the International Society of Renal Nutrition and Metabolism (ISRNM). J Ren Nutr 23: 77–90, 2013 - PubMed
-
- Fielding RA, Vellas B, Evans WJ, Bhasin S, Morley JE, Newman AB, Abellan van Kan G, Andrieu S, Bauer J, Breuille D, Cederholm T, Chandler J, De Meynard C, Donini L, Harris T, Kannt A, Keime Guibert F, Onder G, Papanicolaou D, Rolland Y, Rooks D, Sieber C, Souhami E, Verlaan S, Zamboni M: Sarcopenia: An undiagnosed condition in older adults. Current consensus definition: Prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc 12: 249–256, 2011 - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

