Pain sensation in pancreatic diseases is not uniform: the different facets of pancreatic pain
- PMID: 25083089
- PMCID: PMC4112857
- DOI: 10.3748/wjg.v20.i27.9154
Pain sensation in pancreatic diseases is not uniform: the different facets of pancreatic pain
Abstract
Aim: To systematically characterize specific pain patterns in the most frequent pancreatic diseases.
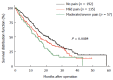
Methods: Pain in patients with chronic pancreatitis (n = 314), pancreatic cancer (n = 469), and other pancreatic tumors (n = 249) including mucinous (n = 20) and serous cystadenoma (n = 31), invasive (n = 37) and non-invasive intraductal papillary mucinous neoplasia (IPMN; n = 48), low stage (n = 18) and high stage neuroendocrine neoplasia (n = 44), and ampullary cancer (n = 51) was registered and correlated with clinicopathological data. Survival times were estimated by the Kaplan-Meier method. Patients alive at the follow-up time were censored. Survival curves were compared statistically using the log-rank test.
Results: Forty-nine point one percent of pancreatic cancer patients revealed no pain, whereas in chronic pancreatitis only 18.3% were pain free. In contrary, moderate/severe pain was registered in 15.1% in pancreatic cancer patients that was increased in chronic pancreatitis with up to 34.2%. Serous cystadenoma was asymptomatic in most cases (58.1%), whereas 78.9% of all mucinous cystadenoma patients suffered pain. In neuroendocrine neoplasia pain was not a key clinical symptom since 64% of low stage neuroendocrine neoplasia and 59% of high stage neuroendocrine neoplasia patients were pain free. Cancer localization in the pancreatic body and patients with malignant pancreatic neoplasms were associated with more severe pain. Tumor grading and stage did not show any impact on pain. Only in pancreatic cancer, pain was directly associated with impaired survival.
Conclusion: Pancreatic pain depicts different patterns of abdominal pain sensation according to the respective pancreatic disorder and does not allow a unification of the term pancreatic pain.
Keywords: Abdominal pain; Chronic pancreatitis; Intraductal papillary mucinous neoplasia; Pancreatic cancer; Pancreatic neoplasm.
Figures
References
-
- Mullady DK, Yadav D, Amann ST, O’Connell MR, Barmada MM, Elta GH, Scheiman JM, Wamsteker EJ, Chey WD, Korneffel ML, et al. Type of pain, pain-associated complications, quality of life, disability and resource utilisation in chronic pancreatitis: a prospective cohort study. Gut. 2011;60:77–84. - PMC - PubMed
-
- Andrén-Sandberg A, Hoem D, Gislason H. Pain management in chronic pancreatitis. Eur J Gastroenterol Hepatol. 2002;14:957–970. - PubMed
-
- Ammann RW, Akovbiantz A, Largiader F, Schueler G. Course and outcome of chronic pancreatitis. Longitudinal study of a mixed medical-surgical series of 245 patients. Gastroenterology. 1984;86:820–828. - PubMed
-
- Ceyhan GO, Bergmann F, Kadihasanoglu M, Altintas B, Demir IE, Hinz U, Müller MW, Giese T, Büchler MW, Giese NA, et al. Pancreatic neuropathy and neuropathic pain--a comprehensive pathomorphological study of 546 cases. Gastroenterology. 2009;136:177–186.e1. - PubMed
-
- Krech RL, Walsh D. Symptoms of pancreatic cancer. J Pain Symptom Manage. 1991;6:360–367. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical