Retinal and optic nerve ischemia
- PMID: 25099097
- PMCID: PMC10563953
- DOI: 10.1212/01.CON.0000453315.82884.a1
Retinal and optic nerve ischemia
Abstract
Purpose of review: This review focuses on aspects of retinal and optic nerve ischemia that may be encountered by neurologists.
Recent findings: Recent guidelines have emphasized the similarities between cerebral and retinal ischemia in terms of etiologic workup, acute management, and subsequent stroke risk. However, although ischemic optic neuropathies reflect optic nerve ischemia, they result from local small vessel disease and are not associated with a higher risk of cerebral infarction. Their management is therefore very different from acute cerebral ischemia. It is essential to rule out giant cell arteritis in all patients with acute retinal or optic nerve ischemia.
Summary: Because the eye is vascularized by branches of the internal carotid artery, retinal ischemic symptoms are common in patients with anterior circulation ischemic strokes. Patients with central retinal artery occlusion, whether permanent or transient (responsible for transient visual loss), need to be evaluated and managed emergently similar to patients with cerebral ischemia, while anterior and posterior ischemic optic neuropathy are more concerning for giant cell arteritis.
Figures
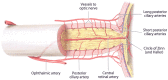
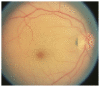
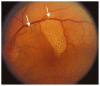
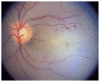
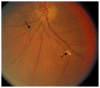
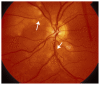
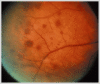
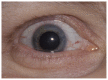
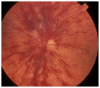
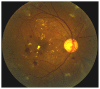
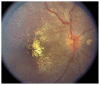
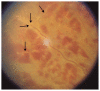
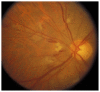
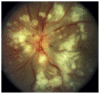

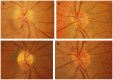

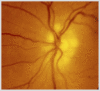

Similar articles
-
New concepts on acute ocular ischemia.Curr Opin Neurol. 2019 Feb;32(1):19-24. doi: 10.1097/WCO.0000000000000634. Curr Opin Neurol. 2019. PMID: 30461463 Review.
-
Idiopathic ischemic syndromes of the retina and optic nerve and their carotid origin.J Vasc Surg. 1985 Sep;2(5):649-53. doi: 10.1067/mva.1985.avs0020649. J Vasc Surg. 1985. PMID: 4032603
-
[Nonarteritic ischemic optic neuropathy animal model and its treatment applications].Nippon Ganka Gakkai Zasshi. 2014 Apr;118(4):331-61. Nippon Ganka Gakkai Zasshi. 2014. PMID: 24864434 Review. Japanese.
-
A novel rodent model of posterior ischemic optic neuropathy.JAMA Ophthalmol. 2013 Feb;131(2):194-204. doi: 10.1001/2013.jamaophthalmol.271. JAMA Ophthalmol. 2013. PMID: 23544206 Free PMC article.
-
[Anterior ischemic optic neuropathy associated with giant cell arteritis. Case report].Klin Oczna. 2006;108(1-3):124-7. Klin Oczna. 2006. PMID: 16883958 Polish.
Cited by
-
Restoration of vision by endovascular revascularization in Takayasu arteritis: A case series.J Cardiol Cases. 2018 Jul 12;18(4):123-127. doi: 10.1016/j.jccase.2018.05.013. eCollection 2018 Oct. J Cardiol Cases. 2018. PMID: 30279928 Free PMC article.
-
Cerebral magnetic resonance imaging of coincidental infarction and small vessel disease in retinal artery occlusion.Sci Rep. 2021 Jan 13;11(1):864. doi: 10.1038/s41598-020-80014-9. Sci Rep. 2021. PMID: 33441709 Free PMC article.
-
Acute retinal arterial ischemia.Ann Eye Sci. 2018 Jun;3:28. doi: 10.21037/aes.2018.05.04. Epub 2018 Jun 6. Ann Eye Sci. 2018. PMID: 30198015 Free PMC article.
-
Chronic ocular small vessel disease: An overview of diabetic retinopathy and its relationship with cardiovascular health.Am Heart J Plus. 2023 Feb 9;29:100270. doi: 10.1016/j.ahjo.2023.100270. eCollection 2023 May. Am Heart J Plus. 2023. PMID: 38510674 Free PMC article.
-
Oxidative Stress and Vascular Dysfunction in the Retina: Therapeutic Strategies.Antioxidants (Basel). 2020 Aug 17;9(8):761. doi: 10.3390/antiox9080761. Antioxidants (Basel). 2020. PMID: 32824523 Free PMC article. Review.
References
-
- Biousse V,, Newman NJ. Neuro-ophthalmology illustrated. New York, NY: Thieme, 2009.
-
- Schuenke M,, Schulte E,, Schumacher U, et al. THIEME atlas of anatomy: head and neuroanatomy. New York, NY: Thieme, 2007.
-
- Johnston SC,, Albers GW,, Gorelick PB, et al. National Stroke Association recommendations for systems of care for transient ischemic attack. Ann Neurol 2011; 69 (5): 872–877. - PubMed
-
- Furie KL,, Kasner SE,, Adams RJ, et al.; American Heart Association Stroke Council, Council on Cardiovascular Nursing, Council on Clinical Cardiology, and Interdisciplinary Council on Quality of Care and Outcomes Research. Guidelines for the prevention of stroke in patients with stroke or transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2011; 42 (1): 227–276. - PubMed
-
- Biousse V,, Trobe JD. Transient monocular visual loss. Am J Ophthalmol 2005; 140 (4): 717–721. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
