Increased mortality associated with digoxin in contemporary patients with atrial fibrillation: findings from the TREAT-AF study
- PMID: 25125296
- PMCID: PMC4405246
- DOI: 10.1016/j.jacc.2014.03.060
Increased mortality associated with digoxin in contemporary patients with atrial fibrillation: findings from the TREAT-AF study
Abstract
Background: Despite endorsement of digoxin in clinical practice guidelines, there exist limited data on its safety in atrial fibrillation/flutter (AF).
Objectives: The goal of this study was to evaluate the association of digoxin with mortality in AF.
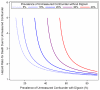
Methods: Using complete data of the TREAT-AF (The Retrospective Evaluation and Assessment of Therapies in AF) study from the U.S. Department of Veterans Affairs (VA) healthcare system, we identified patients with newly diagnosed, nonvalvular AF seen within 90 days in an outpatient setting between VA fiscal years 2004 and 2008. We used multivariate and propensity-matched Cox proportional hazards to evaluate the association of digoxin use with death. Residual confounding was assessed by sensitivity analysis.
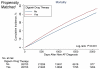
Results: Of 122,465 patients with 353,168 person-years of follow-up (age 72.1 ± 10.3 years, 98.4% male), 28,679 (23.4%) patients received digoxin. Cumulative mortality rates were higher for digoxin-treated patients than for untreated patients (95 vs. 67 per 1,000 person-years; p < 0.001). Digoxin use was independently associated with mortality after multivariate adjustment (hazard ratio [HR]: 1.26, 95% confidence interval [CI]: 1.23 to 1.29, p < 0.001) and propensity matching (HR: 1.21, 95% CI: 1.17 to 1.25, p < 0.001), even after adjustment for drug adherence. The risk of death was not modified by age, sex, heart failure, kidney function, or concomitant use of beta-blockers, amiodarone, or warfarin.
Conclusions: Digoxin was associated with increased risk of death in patients with newly diagnosed AF, independent of drug adherence, kidney function, cardiovascular comorbidities, and concomitant therapies. These findings challenge current cardiovascular society recommendations on use of digoxin in AF.
Keywords: atrial fibrillation; digoxin; mortality; safety.
Copyright © 2014 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Figures

Comment in
-
Outcomes with digoxin in atrial fibrillation: more data, no answers.J Am Coll Cardiol. 2014 Aug 19;64(7):669-71. doi: 10.1016/j.jacc.2014.04.070. J Am Coll Cardiol. 2014. PMID: 25125297 No abstract available.
-
Increased mortality by digoxin in patients with atrial fibrillation?J Am Coll Cardiol. 2015 Jan 20;65(2):220-1. doi: 10.1016/j.jacc.2014.09.081. J Am Coll Cardiol. 2015. PMID: 25593067 No abstract available.
-
Reply: increased mortality by digoxin in patients with atrial fibrillation?J Am Coll Cardiol. 2015 Jan 20;65(2):221. doi: 10.1016/j.jacc.2014.10.032. J Am Coll Cardiol. 2015. PMID: 25593068 No abstract available.
References
-
- Fang MC, Stafford RS, Ruskin JN, Singer DE. National trends in antiarrhythmic and antithrombotic medication use in atrial fibrillation. Arch Intern Med. 2004;164:55–60. - PubMed
-
- Anderson JL, Halperin JL, Albert NM, et al. Management of patients with atrial fibrillation (compilation of 2006 ACCF/AHA/ESC and 2011 ACCF/AHA/HRS recommendations): a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013;61:1935–44. - PubMed
-
- Camm AJ, Kirchhof P, Lip GY, et al. Guidelines for the management of atrial fibrillation: the Task Force for the Management of Atrial Fibrillation of the European Society of Cardiology (ESC) Eur Heart J. 2010;31:2369–429. - PubMed
-
- The Digitalis Investigation Group The effect of digoxin on mortality and morbidity in patients with heart failure. N Engl J Med. 1997;336:525–33. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

