Lung transplantation in idiopathic pulmonary fibrosis: a systematic review of the literature
- PMID: 25127540
- PMCID: PMC4151866
- DOI: 10.1186/1471-2466-14-139
Lung transplantation in idiopathic pulmonary fibrosis: a systematic review of the literature
Abstract
Background: Idiopathic pulmonary fibrosis (IPF) is a distinct form of interstitial pneumonia with unknown origin and poor prognosis. Current pharmacologic treatments are limited and lung transplantation is a viable option for appropriate patients. The aim of this review was to summarize lung transplantation survival in IPF patients overall, between single (SLT) vs. bilateral lung transplantation (BLT), pre- and post Lung Allocation Score (LAS), and summarize wait-list survival.
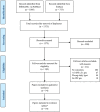
Methods: A systematic review of English-language studies published in Medline or Embase between 1990 and 2013 was performed. Eligible studies were those of observational design reporting survival post-lung transplantation or while on the wait list among IPF patients.
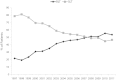
Results: Median survival post-transplantation among IPF patients is estimated at 4.5 years. From ISHLT and OPTN data, one year survival ranged from 75% - 81%; 3-year: 59% - 64%; and 5-year: 47% - 53%. Post-transplant survival is lower for IPF vs. other underlying pre-transplant diagnoses. The proportion of IPF patients receiving BLT has steadily increased over the last decade and a half. Unadjusted analyses suggest improved long-term survival for BLT vs. SLT; after adjustment for patient characteristics, the differences tend to disappear. IPF patients account for the largest proportion of patients on the wait list and while wait list time has decreased, the number of transplants for IPF patients has increased over time. OPTN data show that wait list mortality is higher for IPF patients vs. other diagnoses. The proportion of IPF patients who died while awaiting transplantation ranged from 14% to 67%. While later transplant year was associated with increased survival, no significant differences were noted pre vs. post LAS implementation; however a high LAS vs low LAS was associated with decreased one-year survival.
Conclusions: IPF accounts for the largest proportion of patients awaiting lung transplants, and IPF is associated with higher wait-list and post-transplant mortality vs. other diagnoses. Improved BLT vs. SLT survival may be the result of selection bias. Survival pre- vs. post LAS appears to be similar except for IPF patients with high LAS, who have lower survival compared to pre-LAS. Data on post-transplant morbidity outcomes are sparse.
Figures
References
-
- Raghu G, Collard HR, Egan JJ, Martinez FJ, Behr J, Brown KK, Colby TV, Cordier JF, Flaherty KR, Lasky JA, Lynch DA, Ryu JH, Swigris JJ, Wells AU, Ancochea J, Bouros D, Carvalho C, Costabel U, Ebina M, Hansell DM, Johkoh T, Kim DS, King TE Jr, Kondoh Y, Myers J, Müller NL, Nicholson AG, Richeldi L, Selman M, Dudden RF, Griss BS, Protzko SL, Schünemann HJ. ATS/ERS/JRS/ALAT Committee on Idiopathic Pulmonary Fibrosis. An Official ATS/ERS/JRS/ALAT Statement: Idiopathic pulmonary fibrosis: Evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med. 2011;183(6):788–824. doi: 10.1164/rccm.2009-040GL. - DOI - PMC - PubMed
-
- Selman M, Carrillo G, Estrada A, Mejia M, Becerril C, Cisneros J, Gaxiola M, Pérez-Padilla R, Navarro C, Richards T, Dauber J, King TE Jr, Pardo A, Kaminski N. Accelerated variant of idiopathic pulmonary fibrosis: clinical behavior and gene expression pattern. PLoS One. 2007;2:e482. doi: 10.1371/journal.pone.0000482. - DOI - PMC - PubMed
-
- Collard HR, Moore BB, Flaherty KR, Brown KK, Kaner RJ, King TE, Lasky JA, Loyd JE, Noth I, Olman MA Jr, Lasky JA, Loyd JE, Noth I, Olman MA, Raghu G, Roman J, Ryu JH, Zisman DA, Hunninghake GW, Colby TV, Egan JJ, Hansell DM, Johkoh T, Kaminski N, Kim DS, Kondoh Y, Lynch DA, Müller-Quernheim J, Myers JL, Nicholson AG, Selman M, Toews GB, Wells AU, Martinez FJ. Idiopathic Pulmonary Fibrosis Clinical Research Network Investigators. Acute Exacerbations of Idiopathic Pulmonary Fibrosis. Am J Respir Crit Care Med. 2007;176(7):636–643. doi: 10.1164/rccm.200703-463PP. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical