Perioperative changes in pro and anticoagulant factors in prostate cancer patients undergoing laparoscopic and robotic radical prostatectomy with different anaesthetic techniques
- PMID: 25129475
- PMCID: PMC4431486
- DOI: 10.1186/s13046-014-0063-z
Perioperative changes in pro and anticoagulant factors in prostate cancer patients undergoing laparoscopic and robotic radical prostatectomy with different anaesthetic techniques
Abstract
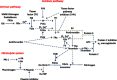
Background: Laparoscopic prostatectomy (LRP) may activate clotting system influencing the risk of perioperative thrombosis in patients with prostate cancer. Moreover, different anaesthetic techniques can also modify coagulant factors. Thus, the aim of this study was to investigate the effects on pro- and anti-coagulant and fibrinolytic factors of two established types of anaesthesia in patients with prostate cancer undergoing elective LRP.
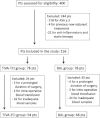
Methods: 102 patients with primary prostate cancer, who underwent conventional LRP or robot-assisted laparoscopic prostatectomy (RALP), were studied and divided into 2 groups to receive total intravenous anesthesia with target-controlled infusion (TIVA-TCI) or balanced inhalation anaesthesia (BAL) prior to surgery. Before the induction of anaesthesia (T0), 1 hr (T1) and 24 hrs post-surgery (T2), some pro-coagulant factors, fibronolysis markers, p-selectin and haemostatic system inhibitors were evaluated.
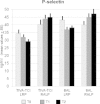
Results: Both TIVA-TCI and BAL patients showed a marked and significant increase in pro-coagulant factors and consequent reduction in haemostatic system inhibitors in the early post operative period (p ≤ 0.004 for each markers). Use of RALP showed a significant increase in prothrombotic markers as compared to LRP. In TIVA patients undergoing LRP, a significant reduction of p-selectin levels between T0 and T2 (p = 0.001) was observed as compared to BAL, suggesting a better protective effect on platelet activation of anaesthetic agents used for TIVA.
Conclusions: Both anaesthetic techniques significantly seem to increase the risk of thrombosis in prostate cancer patients undergoing LRP, mainly when the robotic device was utilized, encouraging the use of a peri-operative thromboembolic prophylaxis in these patients.
Trial registration: ClinicalTrials.gov NCT01998685.
Figures
Similar articles
-
Comparison of anesthetic management and outcomes of robot-assisted vs pure laparoscopic radical prostatectomy.J Clin Anesth. 2016 Dec;35:281-286. doi: 10.1016/j.jclinane.2016.08.014. Epub 2016 Oct 10. J Clin Anesth. 2016. PMID: 27871544
-
Switching from laparoscopic radical prostatectomy to robot assisted laparoscopic prostatectomy: comparing oncological outcomes and complications.Scand J Urol. 2018 Apr;52(2):116-121. doi: 10.1080/21681805.2017.1420099. Epub 2018 Jan 15. Scand J Urol. 2018. PMID: 29334304
-
Benchmarks for operative outcomes of robotic and open radical prostatectomy: results from the Health Professionals Follow-up Study.Eur Urol. 2015 Mar;67(3):432-8. doi: 10.1016/j.eururo.2014.01.039. Epub 2014 Feb 11. Eur Urol. 2015. PMID: 24582327 Free PMC article.
-
Laparoscopic and robot-assisted vs open radical prostatectomy for the treatment of localized prostate cancer: a Cochrane systematic review.BJU Int. 2018 Jun;121(6):845-853. doi: 10.1111/bju.14062. Epub 2017 Nov 17. BJU Int. 2018. PMID: 29063728
-
Minimally Invasive Radical Prostatectomy after Previous Bladder Outlet Surgery: A Systematic Review and Pooled Analysis of Comparative Studies.J Urol. 2019 Sep;202(3):511-517. doi: 10.1097/JU.0000000000000312. Epub 2019 Aug 8. J Urol. 2019. PMID: 31039100
Cited by
-
MicroRNA-195 suppresses tumor cell proliferation and metastasis by directly targeting BCOX1 in prostate carcinoma.J Exp Clin Cancer Res. 2015 Sep 4;34(1):91. doi: 10.1186/s13046-015-0209-7. J Exp Clin Cancer Res. 2015. PMID: 26338045 Free PMC article.
-
PCA3 in prostate cancer and tumor aggressiveness detection on 407 high-risk patients: a National Cancer Institute experience.J Exp Clin Cancer Res. 2015 Feb 6;34(1):15. doi: 10.1186/s13046-015-0127-8. J Exp Clin Cancer Res. 2015. PMID: 25651917 Free PMC article.
-
A meta-analysis of postoperative wound complications at the surgical site in prostate cancer patients undergoing robotic surgery.Int Wound J. 2024 Apr;21(4):e14560. doi: 10.1111/iwj.14560. Epub 2023 Dec 21. Int Wound J. 2024. Retraction in: Int Wound J. 2025 Apr;22(4):e70574. doi: 10.1111/iwj.70574. PMID: 38130091 Free PMC article. Retracted. Review.
-
Central nervous injury risk factors after endovascular repair of a thoracic aortic aneurysm with type B aortic dissection.World J Clin Cases. 2024 Aug 6;12(22):4873-4880. doi: 10.12998/wjcc.v12.i22.4873. World J Clin Cases. 2024. PMID: 39109032 Free PMC article.
-
Robotics versus open surgery: the impact on cytokine release and patient outcomes.J Robot Surg. 2025 Mar 26;19(1):125. doi: 10.1007/s11701-025-02282-9. J Robot Surg. 2025. PMID: 40138107 Review.
References
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

