Pancreatitis-imaging approach
- PMID: 25133027
- PMCID: PMC4133524
- DOI: 10.4291/wjgp.v5.i3.252
Pancreatitis-imaging approach
Abstract
Pancreatitis is defined as the inflammation of the pancreas and considered the most common pancreatic disease in children and adults. Imaging plays a significant role in the diagnosis, severity assessment, recognition of complications and guiding therapeutic interventions. In the setting of pancreatitis, wider availability and good image quality make multi-detector contrast-enhanced computed tomography (MD-CECT) the most used imaging technique. However, magnetic resonance imaging (MRI) offers diagnostic capabilities similar to those of CT, with additional intrinsic advantages including lack of ionizing radiation and exquisite soft tissue characterization. This article reviews the proposed definitions of revised Atlanta classification for acute pancreatitis, illustrates a wide range of morphologic pancreatic parenchymal and associated peripancreatic changes for different types of acute pancreatitis. It also describes the spectrum of early and late chronic pancreatitis imaging findings and illustrates some of the less common types of chronic pancreatitis, with special emphasis on the role of CT and MRI.
Keywords: Acute pancreatitis; Autoimmune pancreatitis; Chronic pancreatitis; Computed tomography; Magnetic resonance imaging; Motion-resistant imaging; Revised Atlanta classification.
Figures

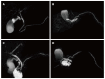
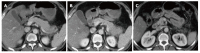
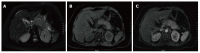
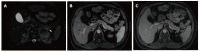
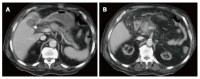
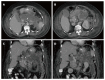
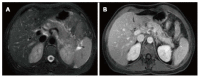
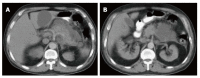
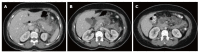
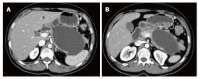
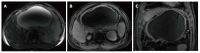
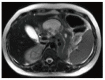
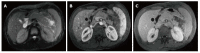
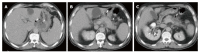
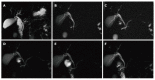
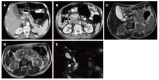
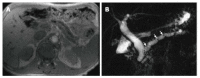
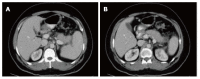
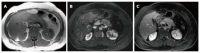
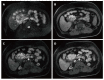
References
-
- Bradley EL. A clinically based classification system for acute pancreatitis. Summary of the International Symposium on Acute Pancreatitis, Atlanta, Ga, September 11 through 13, 1992. Arch Surg. 1993;128:586–590. - PubMed
-
- Petrov MS, Shanbhag S, Chakraborty M, Phillips AR, Windsor JA. Organ failure and infection of pancreatic necrosis as determinants of mortality in patients with acute pancreatitis. Gastroenterology. 2010;139:813–820. - PubMed
-
- Shanbhogue AK, Fasih N, Surabhi VR, Doherty GP, Shanbhogue DK, Sethi SK. A clinical and radiologic review of uncommon types and causes of pancreatitis. Radiographics. 2009;29:1003–1026. - PubMed
-
- Etemad B, Whitcomb DC. Chronic pancreatitis: diagnosis, classification, and new genetic developments. Gastroenterology. 2001;120:682–707. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

