Hepatitis B vaccine responsiveness and clinical outcomes in HIV controllers
- PMID: 25144773
- PMCID: PMC4140789
- DOI: 10.1371/journal.pone.0105591
Hepatitis B vaccine responsiveness and clinical outcomes in HIV controllers
Abstract
Background: Hepatitis B virus (HBV) vaccine responsiveness is associated with reduced risk of AIDS or death in HIV-infected individuals. Although HIV controllers (HIC) typically have favorable immunologic and clinical characteristics compared to non-controllers, vaccine responsiveness has not been studied.
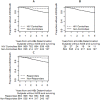
Methods and findings: In the U.S. Military HIV Natural History Study, HBV vaccine response was defined as antibody to hepatitis B surface antigen (anti-HBs) ≥ 10 IU/L after last vaccination. For determination of vaccine responsiveness, HIC (n = 44) and treatment-naïve non-controllers (n = 476) were not on highly active antiretroviral therapy (HAART) when vaccinated while treated non-controllers (n = 284) received all HBV vaccine doses during viral load (VL)-suppressive HAART. Progression to AIDS or death was also compared for all HIC (n = 143) and non-controllers (n = 1566) with documented anti-HBs regardless of the timing of HBV vaccination. Positive vaccine responses were more common in HIC (65.9%) compared to HAART-naïve non-controllers (36.6%; P<0.001), but similar to non-controllers on HAART (59.9%; P = 0.549). Factors associated with vaccine response for HIC compared to HAART-naïve non-controllers include HIC status (OR 2.65, 95% CI 1.23-5.89; P = 0.014), CD4 count at last vaccination (OR 1.28, 1.15-1.45 for every 100 cells/uL; P<0.001), and number of vaccine doses administered (OR 0.56, 0.35-0.88; P = 0.011). When HIC were compared to non-controllers on HAART, only CD4 count at last vaccination was significant (OR 1.23, 1.1-1.38 for every 100 cells/uL; P<0.001). The rate of AIDS or death per 100 person/years for HIC compared to non-controllers was 0.14 (95% CI 0-0.76) versus 0.98 (95% CI 0.74-1.28) for vaccine responders and 0 (95% CI 0-2.22) versus 4.11 (95% CI 3.38-4.96) for non-responders, respectively.
Conclusions: HIC have improved HBV vaccine responsiveness compared to treatment-naïve non-controllers, but similar to those on VL-suppressive HAART. Progression to AIDS or death can be predicted by HBV vaccine responder status for non-controllers, however these events are rarely observed in HIC.
Conflict of interest statement
Figures
References
-
- Okulicz JF, Marconi VC, Landrum ML, Wegner S, Weintrob A, et al. (2009) Clinical outcomes of elite controllers, viremic controllers, and long-term nonprogressors in the US Department of Defense HIV natural history study. J Infect Dis 200: 1714–1723. - PubMed
-
- Lambotte O, Boufassa F, Madec Y, Nguyen A, Goujard C, et al. (2005) HIV controllers: a homogeneous group of HIV-1-infected patients with spontaneous control of viral replication. Clin Infect Dis 41: 1053–1056. - PubMed
-
- Grabar S, Selinger-Leneman H, Abgrall S, Pialoux G, Weiss L, et al. (2009) Prevalence and comparative characteristics of long-term nonprogressors and HIV controller patients in the French Hospital Database on HIV. AIDS 23: 1163–1169. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

