Delayed parasite clearance after treatment with dihydroartemisinin-piperaquine in Plasmodium falciparum malaria patients in central Vietnam
- PMID: 25224002
- PMCID: PMC4249535
- DOI: 10.1128/AAC.02746-14
Delayed parasite clearance after treatment with dihydroartemisinin-piperaquine in Plasmodium falciparum malaria patients in central Vietnam
Abstract
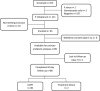
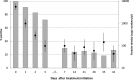
Reduced susceptibility of Plasmodium falciparum toward artemisinin derivatives has been reported from the Thai-Cambodian and Thai-Myanmar borders. Following increasing reports from central Vietnam of delayed parasite clearance after treatment with dihydroartemisinin-piperaquine (DHA-PPQ), the current first-line treatment, we carried out a study on the efficacy of this treatment. Between September 2012 and February 2013, we conducted a 42-day in vivo and in vitro efficacy study in Quang Nam Province. Treatment was directly observed, and blood samples were collected twice daily until parasite clearance. In addition, genotyping, quantitative PCR (qPCR), and in vitro sensitivity testing of isolates was performed. The primary endpoints were parasite clearance rate and time. The secondary endpoints included PCR-corrected and uncorrected cure rates, qPCR clearance profiles, in vitro sensitivity results (for chloroquine, dihydroartemisinin, and piperaquine), and genotyping for mutations in the Kelch 13 propeller domain. Out of 672 screened patients, 95 were recruited and 89 available for primary endpoint analyses. The median parasite clearance time (PCT) was 61.7 h (interquartile range [IQR], 47.6 to 83.2 h), and the median parasite clearance rate had a slope half-life of 6.2 h (IQR, 4.4 to 7.5 h). The PCR-corrected efficacy rates were estimated at 100% at day 28 and 97.7% (95% confidence interval, 91.2% to 99.4%) at day 42. At day 3, the P. falciparum prevalence by qPCR was 2.5 times higher than that by microscopy. The 50% inhibitory concentrations (IC50s) of isolates with delayed clearance times (≥ 72 h) were significantly higher than those with normal clearance times for all three drugs. Delayed parasite clearance (PCT, ≥ 72 h) was significantly higher among day 0 samples carrying the 543 mutant allele (47.8%) than those carrying the wild-type allele (1.8%; P = 0.048). In central Vietnam, the efficacy of DHA-PPQ is still satisfactory, but the parasite clearance time and rate are indicative of emerging artemisinin resistance. (This study has been registered at ClinicalTrials.gov under registration no. NCT01775592.).
Copyright © 2014, American Society for Microbiology. All Rights Reserved.
Figures
References
-
- Noedl H, Se Y, Sriwichai S, Schaecher K, Teja-Isavadharm P, Smith B, Rutvisuttinunt W, Bethell D, Surasri S, Fukuda MM, Socheat D, Chan Thap L. 2010. Artemisinin resistance in Cambodia: a clinical trial designed to address an emerging problem in Southeast Asia. Clin. Infect. Dis. 51:e82–e89. 10.1086/657120. - DOI - PubMed
-
- Amaratunga C, Sreng S, Suon S, Phelps ES, Stepniewska K, Lim P, Zhou C, Mao S, Anderson JM, Lindegardh N, Jiang H, Song J, Su XZ, White NJ, Dondorp AM, Anderson TJ, Fay MP, Mu J, Duong S, Fairhurst RM. 2012. Artemisinin-resistant Plasmodium falciparum in Pursat province, western Cambodia: a parasite clearance rate study. Lancet Infect. Dis. 12:851–858. 10.1016/S1473-3099(12)70181-0. - DOI - PMC - PubMed
-
- Dondorp AM, Nosten F, Yi P, Das D, Phyo AP, Tarning J, Lwin KM, Ariey F, Hanpithakpong W, Lee SJ, Ringwald P, Silamut K, Imwong M, Chotivanich K, Lim P, Herdman T, An SS, Yeung S, Singhasivanon P, Day NP, Lindegardh N, Socheat D, White NJ. 2009. Artemisinin resistance in Plasmodium falciparum malaria. N. Engl. J. Med. 361:455–467. 10.1056/NEJMoa0808859. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

